Types Of Surgery For Diabetes
The following are the most commonly utilized and approved operations performed in the United States and their known impact on type 2 diabetes. View detailed descriptions of common bariatric surgery procedures.
Roux-en-y Gastric Bypass :
The gastric bypass has now been performed for over 50 years. This operation alters the gastrointestinal tract allowing food to avoid most of the stomach and the upper portion of the small intestine. The operation results in significant weight loss, remission of type 2 diabetes in nearly 80 percent of patients, and improvement of diabetes in an additional 15 percent.
Improvement of diabetes after gastric bypass surgery occurs within days to weeks after surgery, even before much weight is lost. Most importantly, this surgery results in changes to the metabolism and hormones produced in the intestines that affect the bodys ability to achieve and maintain a healthy weight.
Sleeve Gastrectomy :
The sleeve is an operation that removes a portion of the stomach. The remaining stomach is narrow and provides a much smaller reservoir for food. The procedure also changes the metabolism and hormones produced by the intestines. These metabolic and hormonal changes result in an improvement in diabetes. Over 60 percent of patients will have remission of their type 2 diabetes after sleeve gastrectomy.
Biliopancreatic Diversion with Duodenal Switch :
Single Anastomosis Duodeno-Ileal Bypass with Sleeve Gastrectomy :
Why Is My Blood Glucose Level High How Does This Happen
The process of digestion includes breaking down the food you eat into various different nutrient sources. When you eat carbohydrates , your body breaks this down into sugar . When glucose is in your bloodstream, it needs help a “key” to get into its final destination where it’s used, which is inside your body’s cells . This help or “key” is insulin.
Insulin is a hormone made by your pancreas, an organ located behind your stomach. Your pancreas releases insulin into your bloodstream. Insulin acts as the key that unlocks the cell wall door, which allows glucose to enter your bodys cells. Glucose provides the fuel or energy tissues and organs need to properly function.
If you have diabetes:
- Your pancreas doesnt make any insulin or enough insulin.
- Your pancreas makes insulin but your bodys cells dont respond to it and cant use it as it normally should.
If glucose cant get into your bodys cells, it stays in your bloodstream and your blood glucose level rises.
How Is Diabetes Diagnosed
Diabetes is diagnosed and managed by checking your glucose level in a blood test. There are three tests that can measure your blood glucose level: fasting glucose test, random glucose test and A1c test.
- Fasting plasma glucose test: This test is best done in the morning after an eight hour fast .
- Random plasma glucose test: This test can be done any time without the need to fast.
- A1c test: This test, also called HbA1C or glycated hemoglobin test, provides your average blood glucose level over the past two to three months. This test measures the amount of glucose attached to hemoglobin, the protein in your red blood cells that carries oxygen. You dont need to fast before this test.
- Oral glucose tolerance test: In this test, blood glucose level is first measured after an overnight fast. Then you drink a sugary drink. Your blood glucose level is then checked at hours one, two and three.
| Type of test |
|---|
You May Like: What Are The Side Effects Of Taking Insulin
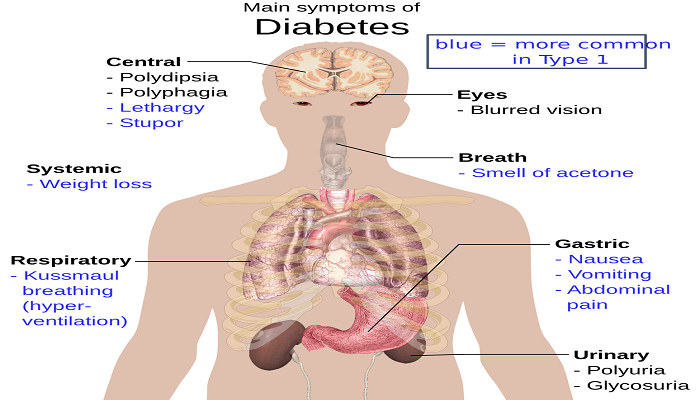
How Are The Signs And Symptoms Similar
There isn’t a difference between the symptoms of either disease. The “classic” symptoms are the same for both diabetes type 1 and type 2:
- Increased urine output
- Unexplained weight loss
For both type 1 and type 2, early symptoms of untreated diabetes arise due to elevated blood sugar levels and the presence of glucose in the urine. High amounts of glucose in the urine can cause increased urine output and dehydration. Dehydration, in turn, causes increased thirst.
A lack of insulin or an inability of insulin to work properly affects protein, fat, and carbohydrate metabolism. Insulin normally encourages the storage of fat and protein, so when there is inadequate insulin or poorly functioning insulin, this eventually leads to weight loss despite an increase in appetite.
Some untreated diabetes patients also experience generalized symptoms like fatigue, nausea, and vomiting. People with diabetes are also at risk for infections of the bladder, skin, and vaginal areas. Changes in blood glucose levels can lead to blurred vision. When blood sugar levels are extremely high, lethargy and coma can result.
Possibility Of Other Health Concerns
Importantly, a correct MODY diagnosis can highlight other health issues that might potentially arise. For example, a MODY 11 mutation to the BLK gene can increase the chances of developing systemic lupus erethematosus .
While being correctly diagnosed as MODY may not change your treatment, it can give you other information, Salsbury said. Many forms of MODY also come along with other health issues that the mutation may have caused. Knowing you have MODY can alert your doctors to watch you or check you for other related health conditions.
Researchers note the same, including Dr. Toni Pollin, a genetic researcher and counselor who in 2016 co-founded the Monogenic Diabetes Research and Advocacy Project at the University of Maryland School of Medicine. The MDRAP effort promotes the correct diagnosis of MODY and also helps raise money for that effort. She co-founded MDRAP with a patient advocate whod been diagnosed with a form of MODY.
While improving MODY diagnosis will certainly improve the clinical care for patients, it will also have broader implications, researchers wrote in this 2015-published
Recommended Reading: Hypoglycemia And Prediabetes
Type 2 Diabetes Is A Serious Pandemic With Serious Complications
Type 2 Diabetes is the most common form of diabetes, accounting for 9095% of all diabetes cases in the world.2 It now affects 415 million people worldwide and is imposing an enormous burden on healthcare systems globally.2 Already a serious global pandemic, it has the potential to get worse. The number of those with diabetes is projected to increase to 642 million people by 2040.2
Every 6 seconds a person dies from diabetes.2
Type 2 Diabetes is a chronic, progressive condition that can severely damage the human body. Each year, 5 million deaths are linked directly to diabetes-related causes.2 Despite the availability of multiple classes of oral glucose-lowering medication, insulin, and other injectables, such as GLP-1 mimetics and insulin analogues, many patients often fail to achieve or maintain control of their diabetes over time, raising their risk of serious complications.3
Long-term complications of diabetes include:1
- An increased incidence of stroke and heart attack
- Diabetic kidney disease leading to renal failure with potential risk for dialysis
- Retinopathy with potential loss of vision
- Peripheral neuropathy with the risk of foot ulcers, and foot and leg amputations
- Autonomic neuropathy causing gastrointestinal, genitourinary and cardiovascular symptoms and sexual dysfunction
The management of Type 2 Diabetes
Which Doctor Treats Type 2 Diabetes
The first points of contact are the family doctor and the diabetologist. If diabetic foot syndrome has already occurred, treatment is carried out in a diabetological foot centre by an interdisciplinary team of diabetologists, angiologists, radiologists, vascular surgeons, orthopaedists and medical chiropodists.
You May Like: Metformin Side Effects Warnings
What Is Gestational Diabetes
Gestational diabetes is a type of diabetes. The condition develops in pregnant women if their blood sugar levels get too high. GD usually appears during the middle of pregnancy, between 24 and 28 weeks.
Developing GD doesnt mean you already had diabetes before you got pregnant. The condition appears because of the pregnancy. Women with Type 1 and Type 2 diabetes have their own, separate challenges when it comes to pregnancy.
Diabetes The Preventable Epidemic
Eat well and exercise. That is the simple message that could help reverse the spread of one of Europes most troubling epidemics Type 2 diabetes.
As a scientist, I want to understand what causes Type-2 diabetes, but sometimes I think my time would be better spent persuading people to eat less and exercise more, said Professor Frances Ashcroft, a British physiologist based at the University of Oxford, UK.
Diabetes occurs in some for no apparent reason, but the most common form, Type-2 diabetes, could often have been prevented. In 90 % of cases, it is linked to eating too much fat, sugar, and salt, and not exercising enough.
The disease now affects about one in 20 Europeans, and this number is said to increase if people keep on eating an unbalanced diet too rich in sugar in particular, and as obesity rates soar.
In fact, the number of European sufferers will increase by over a fifth in the next 20 years, according to the International Diabetes Federation, an umbrella organisation of national diabetes associations in over 160 countries.
The European Union has spent close to EUR 420 million on research to tackle diabetes and related health problems under its 2007 to 2013 funding programme, known as FP7. About EUR 135 million of that is devoted specifically to projects that tackle diabetes and obesity together, a field known as diabesity.
Read Also: Side Effects Of Glucophage
How Does Diabetes Lead To Amputation
Uncontrolled diabetes can lead to poor blood flow . Without oxygen and nutrients , you are more prone to the development of cuts and sores that can lead to infections that cant fully heal. Areas of your body that are farthest away from your heart are more likely to experience the effects of poor blood flow. So areas of your body like your toes, feet, legs and fingers are more likely to be amputated if infection develops and healing is poor.
Getting A Correct Mody Diabetes Diagnosis
Dr. Miriam Udler at Massachusetts General Hospital is one of the more well-known names in MODY clinical research. She believes more cases are being diagnosed in recent years as genetic testing has become more available, particularly after COVID-19 led to a telehealth explosion and more at-home testing kits for bloodwork and diagnostic tests normally done in a lab.
It used to be rare and expensive, and that was a barrier to testing and diagnosing MODY correctly, she told DiabetesMine. But now, more providers have access to this and can order the tests to their clinics or patients at home, and insurance is increasingly covering MODY genetic testing.
While MODY is still less common and infrequently discussed in clinics, Udler says it comes down to that particular doctor or patient recognizing something might be different about their diabetes.
That matters a lot, and a correct diagnosis can change management, Udler said. In most common MODY forms, it could mean coming off medication.
For Salsbury, the particular BLK gene mutation she has causes according to research .
Once MODY is recognized and diagnosed, it can also be difficult to regulate glucose levels in the same ways that T1D and T2Ds often do, because the symptoms and glucose levels can vary significantly.
But she knows everyone is not as fortunate on that front and can have many challenges in getting a correct diagnosis and finding a management routine that works for their particular form of MODY.
Recommended Reading: Type 1 Diabetes Colors
Most Common Types Of Diabetes
There are many misconceptions about diabetes on the internet. The most common is there is only type 1 and type 2. It is important to note that there are actually four types of diabetes. Diabetes is a group of diseases that result in too much sugar in the bloodstream. While glucose is critical to the body for energy, insulin is necessary to break down glucose so it can enter the bodys cells. The most common types of diabetes are type 1, type 2, pre-diabetes, and gestational.
Nephrogenic Diabetes Insipidus Reverses The Issue

Nephrogenic DI occurs when the kidneys are unable to understand what the hormone levels within the body happen to be. The pituitary gland is producing the right levels of ADH that are required, but the kidneys are unable to absorb the water when requested. This defect typically happens within the tubules of the kidney, but may be within the entire functioning mechanism of the organ as well.
The most common reason for nephrogenic diabetes insipidus to occur is because of a long-term medication that is being taken. People who chronically take lithium, for example, have a 40% chance of developing this form of DI. Those who must take a long-term antibiotic such as demeclocycline will also have a higher than average risk of disease development.
Like central diabetes insipidus, the nephrogenic version may also be caused by genetic factors. The symptoms of DI may also be present from birth or may develop slowly over time throughout childhood.
An overabundance of certain minerals may also cause this form of DI. Calcium especially can be problematic for the kidneys and too much of it may cause them to stop responding to the flucuating ADH levels.
Most treatment options are effective for nephrogenic diabetes insipidus, but because of the individualized nature of this disease, finding the right combination can take some time. Making sure enough fluids are consumed will help to prevent dehydration throughout the evaluation and treatment plan creation phases.
Don’t Miss: What Can Happen If Your Blood Sugar Is Too High
Can Diabetes Cause Hearing Loss
Scientists dont have firm answers yet but there appears to be a correlation between hearing loss and diabetes. According to the American Diabetes Association, a recent study found that hearing loss was twice as common in people with diabetes versus those who didnt have diabetes. Also, the rate of hearing loss in people with prediabetes was 30% higher compared with those who had normal blood glucose levels. Scientists think diabetes damages the blood vessels in the inner ear, but more research is needed.
Diabetes In Children And Teens
Until recently, the common type of diabetes in children and teens was type 1. It was called juvenile diabetes. With Type 1 diabetes, the pancreas does not make insulin. Insulin is a hormone that helps glucose,or sugar, get into your cells to give them energy. Without insulin, too much sugar stays in the blood. Now younger people are also getting type 2 diabetes. Type 2 diabetes used to be called adult-onset diabetes. But now it is becoming more common in children and teens, due to more obesity. With Type 2 diabetes, the body does not make or use insulin well. Children have a higher risk of type 2 diabetes if they are overweight or have obesity, have a family history of diabetes, or are not active. Children who are African American, Hispanic, Native American/Alaska Native, Asian American, or Pacific Islander also have a higher risk. To lower the risk of type 2 diabetes in children Have them maintain a healthy weight Be sure they are physically active Have them eat smaller portions of healthy foods Limit time with the TV, computer, and video Children and teens with type 1 diabetes may need to take insulin. Type 2 diabetes may be controlled with diet and exercise. If not, patients will need to take oral diabetes medicines or insulin. A blood test called the A1C can check on how you are managing your diabetes.Continue reading > >
You May Like: Is Metformin Bad For You
Conditions Linked With Type 1 Diabetes
Type 1 diabetes is an autoimmune disease, meaning that the bodys immune system mistakes its own cells for invading pathogens that need to be destroyed.
People with type 1 diabetes tend to have a higher risk of having other autoimmune diseases than the rest of the population.
Other autoimmune diseases include:
- Autoimmune thyroid disease
How Does Diabetes Affect The Body
There are two main types of diabetes: type 1 and type 2.
Both types of diabetes are chronic diseases that affect the way your body regulates blood sugar, or glucose. Glucose is the fuel that feeds your bodys cells, but to enter your cells it needs a key. Insulin is that key.
People with type 1 diabetes dont produce insulin. You can think of it as not having a key.
People with type 2 diabetes dont respond to insulin as well as they should and later in the disease often dont make enough insulin. You can think of it as having a broken key.
People with type 1 and type 2 diabetes may also experience irritability, mood changes, and unintentional weight loss.
People with type 1 and type 2 diabetes may also have numbness and tingling in their hands or feet. Good glucose management significantly reduces the risk of developing numbness and tingling in someone with type 1 diabetes, according to the American Diabetes Association .
Although many of the symptoms of type 1 and type 2 diabetes are similar, they present in very different ways.
Many people with type 2 diabetes wont have symptoms for many years, and their symptoms often develop slowly over the course of time. Some people with type 2 diabetes have no symptoms at all and dont discover they have the condition until complications arise.
Type 1 and type 2 diabetes may have similar names, but theyre different diseases with unique causes.
Recommended Reading: Metformin Prediabetes Dose
The Different Types Of Diabetes
As the years progress, doctors are reimagining the diabetic world. Research is ongoing to try and find a cure, or at least a less intrusive treatment option. With that research there have been a number of accounts of rare forms of diabetes that often result from a specific condition1. Since these types of diabetes only account for a very small amount of cases 1, weve omitted them in this article.
If youre interested in learning more about the rare forms of diabetes, check out this article. For now, well focus on the two most common types of diabetes along with two types of diabetes that should be tested for.

