If Not Controlled At The Right Time Diabetes Can Lead To Kidney Failure Partial Or Complete Blindness Nerve Problems Loss Of Limbs And Increase The Risk Of A Heart Attack
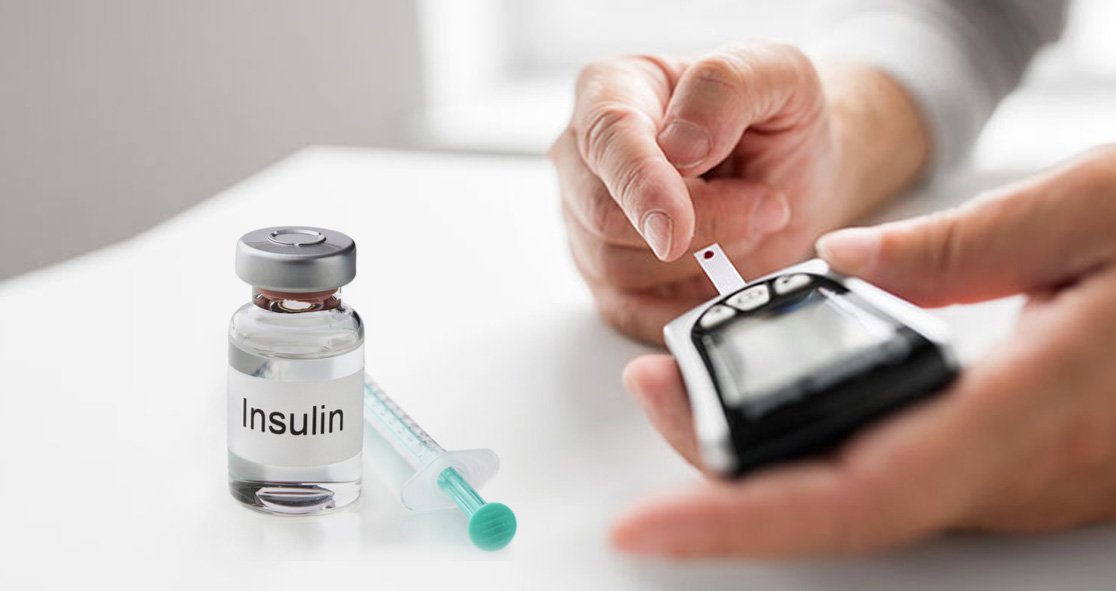
Insulin, which is produced by the pancreas in the body, helps control the body’s blood sugar level. Regular insulin intake along with a proper diet and exercise plan is recommended for type 2 diabetes patients to help maintain their blood sugar level. If not controlled at the right time, diabetes can lead to kidney failure, partial or complete blindness, nerve problems, loss of limbs and even increase the risk of a heart attack. However, there are several myths around injecting insulin due to lack of awareness.
A study, published in the American Medical Association’s biomedical journal JAMA Network Open, also found that the relative risk of death due to diabetes itself was much stronger among individuals who were underweight. The findings suggest that there is an urgent need to “develop diabetes management programs that are tailored to Asian populations and the subsequent strong implementation of these programs in Asia”.
Why do Type 2 diabetics need insulin?
“The pancreas, that produces digestive enzymes, is also responsible for producing insulin, a hormone that helps regulate blood sugar levels. Insulin helps the body use the carbohydrates in food for energy. If a patient develops Type 2 diabetes, their pancreas stop producing sufficient insulin that is required for the body to control blood sugar level”, said Dr Roopak Wadhwa, consultant, department of diabetes endocrinology and metabolism at Fortis Hospital.
Tips while taking insulin injections
Heres The Thing: Your Journey Is Unique And It Starts Fresh Every Day
No matter where you are with type 2 diabetes, there are some things you should know. It’s the most common form of diabetes. Type 2 means that your body doesn’t use insulin properly. And while some people can control their blood sugar levels with healthy eating and exercise, others may need medication or insulin to manage it. Regardless, you have everything you need to fight it. Not sure where to start? Learn how type 2 diabetes is diagnosed.
Why Insulin Can Become Necessary For A Person With Type 2 Diabetes
Starting insulin treatment should not be seen as a setback.
People with type 2 diabetes may require insulin when their meal plan, weight loss, exercise and antidiabetic drugs do not achieve targeted blood glucose levels.
Diabetes is a progressive disease and the body may require insulin injections to compensate for declining insulin production by the pancreas. That is why starting insulin treatment should never be seen as a failure.
Starting insulin treatment should never be seen as a failure.
Treatment with insulin may be added to an antidiabetic medication or completely replace it. Regardless of the treatment, lifestyle habits are essential to managing diabetes.
Many people are reluctant to inject insulin for various reasons:
- Fear of pain or needles
- Guilt
- Impression that this is the “last resort”
- Fear of hypoglycemic attacks
- Fear of weight gain
- Memories of loved one who had to take insulin
If this is the case, do not hesitate to discuss your concerns with a health care professional. Some of your fears may be due to false beliefs. Learning more about today’s insulin treatment will probably allay your fears. For many people, insulin is an effective way to achieve good blood-sugar control, which can prevent or delay certain diabetes complications over the long term.
Why Do Some People With Type 2 Diabetes Need To Take Insulin
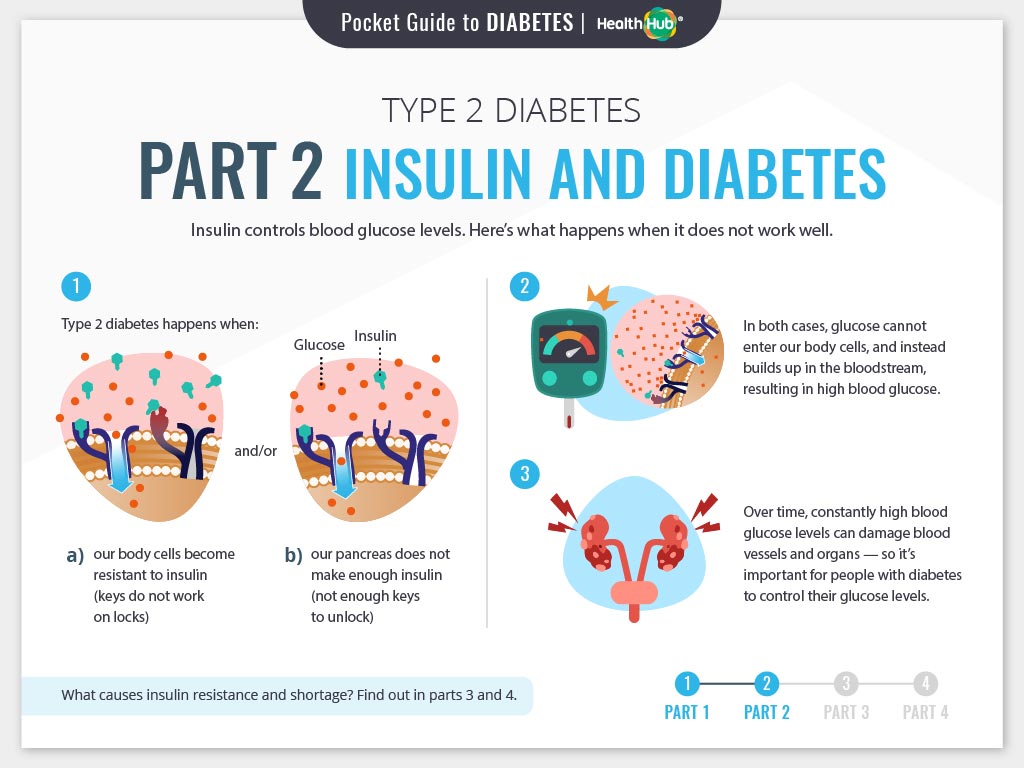
Type 2 diabetes can progress with time, which means that it gets more difficult for a person’s body to regulate glucose levels. The body’s many cells become less responsive to insulin , and the specific cells in the pancreas that produce insulin make less of it . This is not necessarily related to a person’s diabetes management, and it is likely not possible to prevent.
For many people, adjusting lifestyle factors such as a reduced calorie diet and increased physical activity are key to keeping blood glucose levels stable and in a target range. Healthcare professionals may also recommend that people with type 2 diabetes take additional medications like metformin, DPP-4 inhibitors, SGLT-2 inhibitors, or GLP-1 agonists to their treatment plan to improve glucose management, reduce A1C, lose weight, or support heart and kidney health.
Getting Started With Insulin If You Have Type 2 Diabetes
New to insulin? Learn about insulin dosing and timing and how often to test your blood sugar levels if you have type 2 diabetes.
If you have type 2 diabetes, it is likely that your treatment regimen will change over time as your needs change, and at some point, your healthcare professional may suggest that you start taking insulin. While this might feel scary, there are millions of others living with type 2 diabetes and taking insulin, so it’s definitely manageable.
When Dietary Changes Exercise And Medications Don’t Work
type 1 diabetesrole of insulin
- It can quickly bring your blood glucose level down to a healthier range. If your blood glucose level is excessively high when you are diagnosed with type 2 diabetes, the doctor may have you use insulin to lower your blood glucose level—in a way that’s much faster than diet and exercise.Insulin will give your body a respite; it has been working overtime to try to bring down your blood glucose level.In this scenario, you’d also watch what you eat and exercise, but having your blood glucose under better control may make it easier to adjust to those lifestyle changes.
- It has fewer side effects than some of the medications: Insulin is a synthetic version of a hormone our bodies produce. Therefore, it interacts with your body in a more natural way than medications do, leading to fewer side effects. The one side effect is hypoglycemia.
- It can be cheaper. Diabetes medications can be expensive, although there is an array of options that try to cater to people of all economic levels. However, insulin is generally cheaper than medications , especially if the doctor wants you to take multiple medications.
Talk to your doctor and diabetes treatment team.Patient Guide to InsulinTypes of InsulinHow Much Insulin Should You Take?Where Should You Inject the Insulin?
- Abdomen
Newer, Easier Ways to Inject Insulininsulin deliveryA Final Note about Insulin
Whats The Difference Between Type 1 And Type 2 Diabetes
Type 1 diabetes is an autoimmune disease that impacts 1.25 million American children and adults. For type 1, the immune system destroys the cells that release insulin, eventually leading to the complete inability to produce insulin in the body. Type 1 generally manifests at a young age and lasts a lifetime.
Type 2 diabetes has multiple contributing factors including genetics and lifestyle factors such as obesity and inactivity. The disease generally arises during adulthood and oftentimes can be reversed or controlled through diet and exercise. 90-95% of those diagnosed with diabetes have type 2.
How To Get Free Prescriptions For Diabetes Medicine
You’re entitled to free prescriptions for your diabetes medicine.
To claim your free prescriptions, you’ll need to apply for an exemption certificate. This is known as a PF57 form. To do this:
- fill in a form at your GP surgery
- you should get the certificate in the post about a week later – it’ll last for 5 years
- take it to your pharmacy with your prescriptions
Save your receipts if you have to pay for diabetes medicine before you receive your exemption certificate. You can claim the money back if you include the receipts along with your completed PF57 form.
When Do People With Type 2 Diabetes Start Insulin
After 10 to 20 years, many people with type 2 diabetes will begin insulin therapy, although every person’s journey with type 2 diabetes is different. This happens when lifestyle changes and medications aren’t keeping your glucose levels in your target range. It is important that you start treatment as early as possible to avoid persistent hyperglycemia , which can lead to long-term health complications affecting your heart, kidneys, eyes, and other organs.
What Else Do I Need To Know About Taking Insulin
Staying in contact with your healthcare team is the best way to make the transition to insulin therapy. Though the first few days or weeks will be challenging, with the right support, you’ll find a diabetes care plan that works for you.
If you were recently diagnosed with type 2 diabetes, check out more resources here.
What Are The Signs & Symptoms Of Type 2 Diabetes
People who have type 2 diabetes may not know it because the symptoms aren’t always obvious and they can take a long time to develop. Some people don’t have any symptoms at all.
But when a person gets type 2 diabetes, he or she may:
- pee a lot because the body tries to get rid of the extra blood sugar by passing it out of the body in the urine
- drink a lot to make up for all that peeing
- feel tired all the time because the body can’t use sugar for energy properly
Also, people whose bodies are having problems using insulin or who are overweight may notice something called acanthosis nigricans. This can cause a dark ring around the neck that doesn’t wash off, as well as thick, dark, velvety skin under the arms, in between fingers and toes, between the legs, or on elbows and knees. This skin darkening can lighten over time with improvement in insulin resistance.
In addition, girls with insulin resistance may have polycystic ovary syndrome . In PCOS, the ovaries get bigger and develop fluid-filled sacs called cysts. Girls with this condition often have irregular periods or may stop having periods, and they might have excess facial and body hair.
Is There An Age Where Im More At Risk Of Type 2
Type 2 diabetes used to be known as adult-onset diabetes as it was primarily seen in middle-aged adults over the age of 40.
However, in recent years, cases of type 2 diabetes have become more common in young adults, teens and children. This increase has been connected to climbing levels of obesity
- See our guide on diabetes risk factors for more information.
Insulin Use Requires Multiple Daily Injections

Not always. If you need insulin, you have options. You can try a long-acting once-a-day insulin , which mimics the low level of insulin normally found in the body all day long. This may be enough to control blood sugar on its own, or it can be combined with oral medications. If blood sugar is still too high after meals, however, you may need to take insulin several times a day, just before eating.
Insulin Can Cause Dangerously Low Blood Sugar
Okay this one is possible, but not likely. People with type 2 diabetes tend to be at lower risk of hypoglycemia than those with type 1. A prolonged episode of low blood sugar could cause a loss of consciousness or coma. Still, most people with type 2 can easily recognize the symptoms, which include anxiety, shaky hands, sweating, and an urge to eat. Consuming a bit of sugar—a few Life Savers, diluted juice, or glucose tablets—quickly reverses the low blood sugar.
What’s It Like For Teens With Type 2 Diabetes
Sometimes people who have diabetes feel different from their friends because they need to think about how they eat and how to control their blood sugar levels every day.
Some teens with diabetes want to deny that they even have it. They might hope that if they ignore diabetes, it will just go away. They may feel angry, depressed, or helpless, or think that their parents are constantly worrying about their diabetes management.
If you’ve been diagnosed with type 2 diabetes, it’s normal to feel like your world has been turned upside down. Your diabetes care team is there to provide answers and support. Don’t hesitate to ask your doctors, dietitian, and other treatment professionals for advice and tips. It also can help to find support groups where you can talk about your feelings and find out how other teens cope.
Diabetes brings challenges, but teens who have it play sports, travel, date, go to school, and work just like their friends.
What Happens If You Avoid Taking Your Insulin
If you have type 1 diabetes, taking insulin is essential and you cannot live without it. If you avoid taking it, your blood sugar levels can become too high and you risk developing diabetic ketoacidosis . If left untreated, DKA could be life-threatening. That’s why it’s important to make sure you take your insulin.
If you have type 2 diabetes and use insulin to treat your condition, you should continue to take it as prescribed. If you avoid taking it, your blood sugar levels could become too high and you may become ill. Please speak to your healthcare professional if you have any questions or concerns about taking your insulin.
Insulin is a treatment that helps manage blood sugars, so this also reduces the risk of serious long-term complications as well a shorter-term consequences. It’s still important to keep going to your appointments and manage your condition with healthy lifestyle choices. Staying active and eating a healthy diet will reduce the risk of complications from your diabetes, but insulin is also an important part of your treatment.
Risks Of Insulin Therapy For Type 2 Diabetes
Many people with type 2 diabetes can benefit from insulin therapy, but like most medications, it carries some risks.
The most serious risk is low blood sugar, or hypoglycemia. Left untreated, low blood sugar can be a medical emergency.
Low blood sugar can usually be treated quickly and effectively by eating a higher-sugar item, such as glucose tablets, and then monitoring your blood sugar levels.
If your doctor prescribes insulin to treat your diabetes, they’ll talk with you about managing the risk of low blood sugar.
There are other risks with taking insulin. For example, the injections can be uncomfortable. Insulin can also potentially cause weight gain or, rarely, infection at the injection site.
Your doctor can tell you more about the potential benefits and risks of adding insulin to your treatment plan.
If you think you might be experiencing side effects from insulin, contact your doctor right away.
Some people with type 2 diabetes need a single dose of insulin per day. Others need 2 or more doses per day.
Your recommended insulin regimen can vary depending on:
- your medical history
- trends in your blood sugar levels
- the timing and contents of your meals and workouts
- the type of insulin you use
Your healthcare team will instruct you about how often and when you should take your prescribed insulin.
Insulin injections can be administered using:
- a syringe
- an insulin pen
- an insulin pump
Ask your healthcare provider for tips to make injections easier and less uncomfortable.
Producing Less Insulin Naturally Over Time
Research has shown that type 2 diabetes progresses as the ability of the body’s pancreatic beta cells to produce insulin dwindles over time. Your beta cells — the cells in the pancreas that produce insulin — slowly lose function. Experts believe that by the time you’re diagnosed with type 2 diabetes, you’ve already lost 50-80 percent of your beta cell function and perhaps the number of beta cells you had. And the loss continues over the years.
“About six years after being diagnosed, most people have about a quarter of their beta cell function left,” says Anthony McCall, M.D., Ph.D., endocrinologist and James M. Moss Professor in Diabetes at the University of Virginia School of Medicine. “With this minimal function, the need for injected insulin increases.”
Some experts say initiating insulin or other blood glucose-lowering medications early in the course of type 2 diabetes can lower blood glucose and even preserve some beta cell function.
Insulin Needs In The Two Types Of Diabetes
Even though patients with both type 1 and type 2 diabetes need insulin, as that is the main cause behind the condition, their individual need for insulin varies.
While people living with type 1 diabetes need to supplement their body with insulin due to the inability of their body to make enough, the case is a bit different with type 2 diabetes.
Although a type 2 diabetes patient may be prescribed insulin, doctors will most likely recommend you first start out on a healthy diet and a more active life through regular exercise to see if it will help.
Even if at the end, you will need to take medications and/or insulin, exercising and eating right may help you require less than you expected.
A significant factor that determines whether or not a person with type 2 diabetes will need insulin is your individual circumstance.
How Do I Take And Adjust My Insulin Doses
It is important to learn the different methods of taking insulin and what kinds of insulin can be delivered through each method. There are several ways to take insulin – syringe, pen, pump, or inhalation – though injection with a syringe is currently the most common for people with type 2 diabetes. There are many apps that can help you calculate your insulin doses.
Your insulin regimen should be tailored to fit your needs and lifestyle. Adjusting your basal insulin dosage and timing will require conversations and frequent follow-up with your healthcare team. When initiating insulin therapy, you may be advised to start with a low dose and increase the dose in small amounts once or twice a week, based on your fasting glucose levels. People with diabetes should aim to spend as much time as possible with glucose levels between 70-180 mg/dl. Insulin may be used alone or in combination with oral glucose-lowering medications, such as metformin, SGLT-2 inhibitors, or GLP-1 agonists.
One of the most important things to consider is the characteristics of different insulin types. To learn more, read “Introducing the Many Types of Insulin – Is There a Better Option for You?” and discuss with your healthcare team.
In order to dose insulin to cover meals or snacks, you have to take a few factors into consideration. Your healthcare team should help you determine what to consider when calculating an insulin dose. Prandial insulin doses will usually be adjusted based on:
Where Manufactured Human Insulin Comes In
The goal of taking insulin injections is to mimic your body’s normal insulin response. People who take insulin most likely will eventually need a combination of rapid- or short-acting and long-acting insulins to mimic normal insulin function and to control blood glucose.
A normal pancreas releases insulin constantly, not just when you eat, says John Walsh, P.A., CDE, coauthor of Using Insulin: Everything You Need for Success with Insulin . Adults produce about 1 unit of insulin per hour. This is called basal insulin or background insulin.
In response to food, insulin is released from the pancreas in two phases:
1. The first burst occurs within 15 minutes of your first bite in response to rising blood glucose.
2. The second phase happens more slowly, over the next one-and-a-half to three hours, to match the rise in blood glucose from the food you ate, which is called bolus insulin or mealtime insulin.
Oral Medications Are Better Than Insulin
Oral diabetes medications can be great when it comes to lowering blood glucose levels. Many have been used for years and are very safe, such as metformin.Still, they don’t work for everyone. “For some people, insulin is the easiest and best because it always works, but some people respond to pills, and others don’t,” says Dr. Crandall.Not all oral medications have a tried-and-true safety record. For example,
Avandia was restricted by the FDA because of research suggesting that it ups the risk of heart attack.
Myths About Insulin And Type 2 Diabetes
When you hear the word “insulin,” do you picture giant needles or pop culture portrayals of insulin users with low blood sugar ?Either way, most people think of insulin as a difficult, painful, or potentially scary medical treatment.The problem is that if you have type 2 diabetes, you need to know the real deal before you can make an informed choice about whether or not this potentially lifesaving therapy is right for you.Here, we take a look at the facts and fiction about insulin when it comes to treating type 2 diabetes.
What Are The Different Types Of Insulin
The key to transitioning to insulin is knowing your options. Some people taking insulin need to use both a basal and a prandial insulin each day, while others may only need to use basal insulin. Learn about your options here.
-
Basal insulins are designed to be injected once or twice daily to provide a constant background level of insulin throughout the day. Basal insulins help keep blood sugars at a consistent level when you are not eating and through the night but cannot cover carbohydrates eaten for meals or snacks or glucose spikes after meals.
-
Some people use other medications, like GLP-1 agonists, to help cover mealtimes. GLP-1/basal combination treatments for people with type 2 diabetes combine basal insulin with GLP-1 agonist medication in one daily injection. This combination can effectively lower glucose levels while reducing weight gain and risk of hypoglycemia . Learn more here.
Prandial insulins are taken before mealtime and act quickly to cover carbohydrates eaten and bring down high sugar levels following meals. Ultra-rapid-acting prandial insulins can act even more rapidly in the body to bring down glucose levels. Rapid and ultra-rapid insulins are also taken to correct high glucose levels when they occur or are still persistent a few hours after a meal.
Common Questions About Type 2 Diabetes:
- Can type 2 diabetes go away?
- Will I need to take insulin?
- Do I have to take it forever?
How do you treat type 2 diabetes?
When you have type 2 diabetes, you first need to eat a healthy diet, stay physically active and lose any extra weight. If these lifestyle changes cannot control your blood sugar, you also may need to take pills and other injected medication, including insulin.
Eating a healthy diet, being physically active, and losing any extra weight is the first line of therapy. “Diet and exercise“ is the foundation of all diabetes management because it makes your body’s cells respond better to insulin and lowers blood sugar levels.
If you cannot normalize or control the blood sugars with diet, weight loss and exercise, the next treatment phase is taking medicine either orally or by injection.
Diabetes pills work in different ways – some lower insulin resistance, others slow the digestion of food or increase insulin levels in the blood stream. The non-insulin injected medications for type 2 diabetes have a complicated action but basically lower blood glucose after eating. Insulin therapy simply increases insulin in the circulation.
Many people with type 2 diabetes have elevated blood fats and blood pressure, so you may be given medications for these problems as well.
Can type 2 diabetes go away? And if my blood sugar becomes normal, do I still have diabetes?
Will I need to take insulin if I have type 2 diabetes?
Making The Most Out Of Your Own Insulin
To stay healthy with type 2 diabetes over the years, the key is controlling your blood sugar, blood pressure, and blood lipids . These are the so-called ABCs of diabetes care — A is for A1C , B for blood pressure, and C for cholesterol . To control blood sugar, you need to continually and progressively be adjusting your diabetes care to compensate for your body’s waning supply of insulin and growing level of insulin resistance.
At diagnosis, some people still produce enough insulin to hit their blood sugar targets by eating healthfully, getting physical activity, and losing weight. In fact, losing 10-20 pounds can make a dramatic impact early on. But research shows that most people need to start diabetes medications and/or insulin right away.
As the body gradually produces less insulin, nearly everyone with type 2 diabetes needs one or more oral or injectable blood glucose-lowering medications, which might include insulin. Additionally, there is now a category of blood glucose-lowering medicines called incretin mimetics or GLP-1 analogs that are injectable: Byetta, Victoza, and Bydureon are the three approved brands.
When you start insulin or any blood glucose-lowering medication, you still need to eat healthfully and be physically active.

