Diabetic Foot Ulcer Treatment
The first step in treatment of diabetic foot ulcers is to remove necrotic wound tissue from the wound. It is essential that the method of debridement utilized does not damage nerves, tendons, and blood vessels. Since many people with diabetes dont feel pain from the wound site, health care practitioners cant rely on the patient to let them know when sensitive areas are being examined. The debridement will:
- Reduce pressure on the ulcer.
- Stimulate wound healing.
- Allow the healthy underlying tissue to be examined.
- Help the wound to drain.
- Optimize the effectiveness of the wound dressing.
Recommended Reading: What Is A Normal A1c For A Non Diabetic
Treatment For Vascular Ulcers
Its important to note that not all skin ulcers are caused by diabetes, and that even people who dont have diabetes can suffer from chronic wounds. Even people without diabetes can be susceptible to vascular ulcers. Vascular ulcers are caused by problems with the vascular system .
These types of ulcers can happen to people who suffer from veins or arteries that dont function properly, causing blood flow in the legs to be limited. This can lead to an increased risk of wounds that may not heal normally and can become infected.
The Wound Care Center at Harrington also provides full service care for these types of wounds, including on-site X-rays, MRI and lab work.
To make an appointment at the Harrington Wound Care Center, call 248-8105. You can also learn more on our website here.
Wet To Dry Dressing Or Simple Saline
This dressing has a good debriding action and helps in wound bed preparation. Wet-to-dry dressings are described in the literature as a means of mechanical debridement. It is very absorptive as well as adherent and one of the cheapest dressings used throughout the world, but requires frequent dressing change based on wound severity. Dressings should be moistened before removal to minimize any chance of bleeding. A gentle cleanser will minimize wound irritation and discomfort. When treating a granulating or epithelizing wound one should soak the dressing thoroughly with normal saline for five minutes to prevent trauma and heavy bleeding.
You May Like: What Is A Normal A1c For A Non Diabetic
How Emuaid Works To Eliminate Your Diabetic Ulcer Symptoms
What Are Diabetic Feet
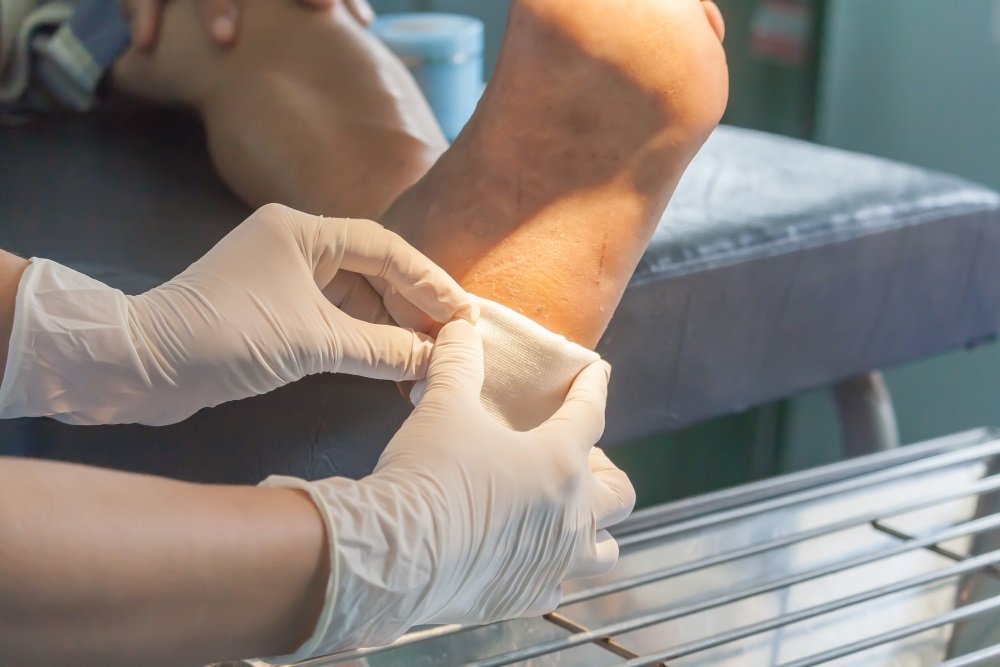
People with diabetes often have problems with their feet. Diabetic feet develop sores, deformities and infections more easily.
If not treated quickly, a diabetic foot ulcer or blister can get infected. Sometimes a surgeon must amputate a toe, foot or part of the leg to prevent the spread of infection.
You May Like: How Many Points Does Metformin Lower Blood Sugar
Treatments Your Physician May Prescribe
In the case of a new ulcer, your doctor may want to take an X-ray of the area to make sure that there is no infection , fracture of the bone, or foreign objects lodged in the ulcer, as you may not feel them. Next, the doctor will likely remove any dead tissue with a scalpel from the area, revealing healthy skin. While this will actually make the ulcer larger in size and cause bleeding, it is important to have healthy tissue exposed for faster and cleaner healing. This will likely be done in the operating room, under anesthesia. After the surgery, be sure to follow proper instructions on wound care, making sure to apply any medications and dressings as directed.Your doctor may send a sample of skin or fluid for bacterial culture and start you on oral antibiotics. It is very important to follow up with your doctor as scheduled: neurogenic ulcers can worsen very quickly and need to be closely monitored. Make sure to call your doctor if you experience any of the following: redness of the area, red streaking up the leg, drainage of the area, pain, foul odor, rising blood glucose, or swelling or redness of the top of the foot.Your doctor may have you wear a special cast that will allow you to continue to be mobile but take pressure off the area. There are also medications that use growth factors to stimulate wound healing that your doctor may prescribe.
How To Prevent Diabetic Ulcers And Promote Healing Of Chronic Wounds
Living with diabetes increases your risk of developing several complications. Due to the relationship between blood sugar and your circulatory system, people with diabetes are at a higher risk for developing diabetic neuropathy and other circulatory issues. Over time, this has a direct impact on wound healing, which subsequently increases your risk for infection. To reduce complications, heres how to prevent diabetic ulcers and promote healing of chronic wounds.
Read Also: Ideal A1c Levels
Q: What Causes Heel Pain
A: Typically, heel pain is not caused by one single incident or injury, and the most common cause is plantar fasciitis, which can lead to long-term pain that may one day require surgical treatment if not corrected.
Repetitive stress/pounding of the heel can cause heel pain.
Other common causes can include inflammation of the plantar fascia, inflammation of the back of the heel, inflammation of the heel pad, progressive degeneration of the Achilles tendon, or a stress fracture caused by repetitive stress to the heel.
Promising Treatments For The Healing Of Diabetic Foot Ulcers
The number of Canadians with #diabetes is rapidly increasing. According to the Canadian Diabetes Association, more than 20 Canadians are diagnosed with the disease every hour of every day.
#Diabetic foot ulcers are the most common chronic complication from diabetes, affecting four to 10 per cent of patients. DFUs can last a year or longer and can happen again in up to 70 per cent of people who have previously been affected. Patients are more likely to develop DFUs if they have had diabetes for a long time, have poorly controlled blood sugar, have foot injuries or infection, are older, or smoke. However, neuropathy, damage to the nerves, which may result in a lack of feeling in the feet, and peripheral artery disease, which reduces the blood flow to the limbs, may be the most significant causes. Because of nerve damage and numbness, an individual with diabetes may not be aware that they have a sore or wound, leading to even minor injuries getting worse or becoming infected. Decreased blood flow caused by peripheral vascular disease may prevent healing once an injury occurs.
When DFUs become infected, the bone or skin can also become infected. This can lead to significant pain and suffering poor quality of life for patients amputation of a leg, foot, or toe increased treatment and hospitalization costs and can even lead to death.
Off-Loading Devices
Compression Therapy
Also Check: Dee Dee Blanchard Diabetes
How Do You Treat Diabetic Foot Ulcers
When a DFU is present, attempts to treat at home should not be made. Patients must seek medical attention to be sure that the ulcer or wound is not a venous ulcer, an arterial ulcer, a malignant melanoma, or another issue. Additionally, the risk of being too submissive in the treatment of a DFU without seeing a physician for care can result in the risk of compromising the extremity.
Once a physician has been consulted and diagnosis is confirmed, treatment will consist of three basic approaches: debriding the wound, keeping weight off the wound, and controlling the risk of infection.
Debridement of the wound involves the removal of necrotic tissue on the foot. Periwound callus must be removed as well. Once these two steps have been taken, the critical step of removing foreign bodies must be carried out. The debridement process needs to be ongoing until viable tissue is present. This will reduce infection risk and ease peri-wound pressure . Once debridement is complete, the ulcerated area should be thoroughly rinsed with an irrigation agent such as saline, followed by the application of a wound dressing. If an abscess is present, the ulcer will be incised and drained before the abscessed tissue is removed via debriding. If treatment is swift and accurate, amputation can be avoided. Antibiotics alone will not prevent morbidity and mortality.
- Staphylococcus aureus
- Bacteroides
- Peptostreptococcus
Praise For Emuaid From Satisfied Customers
We are very thankful for the early arrival of your fine product. My sister, in less than 24 hours, is now completely Pain free. Very, very grateful,*
Dennis L F
I use Emuaid for my skin condition that causes constant itching. Since using Emuaid the itching is completely gone. Its a great product!*
Theresa S.
Emuaid max is a great product that I have bought several times.I am diabetic and it is slow healing but it does help alot*
Anonymous Customer
I am so glad I found this cream to help my husband, in one week I could see a big different. Today we had a Doctor appoinment , she was so surprise how it got better, she took me to the computer to show me the picture from last week and now what a different, I just have to tell her about your cream, she said , she never heard about this cream. I strongly recomend r*
David J
It is the only meds that i have ever found that totally works. the shopping exp, was awesome thanks*
Maggie T.
This stuff is so good. I got the extra strength this time. I am assured that it will work as well or better. Nothing I have tried before worked until I discovered this product. Its a miracle in a jar.*
Paul
Show/Hide all customer reviews +
D. G.
My order came within the promised time and my sore parts were better in 2 days. I cant wait to try it on other skin issues to test its effectiveness. When I talk to my Dr. again I am going to suggest he recommend this to his patients with any skin ailment.*
ElizabethLucyRalphAliceRolandAlbieFred
You May Like: Stopping Glipizide
Trust South Valley Vasculars Expertise
The medical experts at South Valley Vascular in Visalia, Porterville, and Hanford, California, specialize in the diagnosis, treatment, and management of diseases and conditions of the blood vessels. Our vascular surgeons will determine a treatment plan that provides the best benefits for your specific needs.
How To Treat Diabetic Foot Ulcers
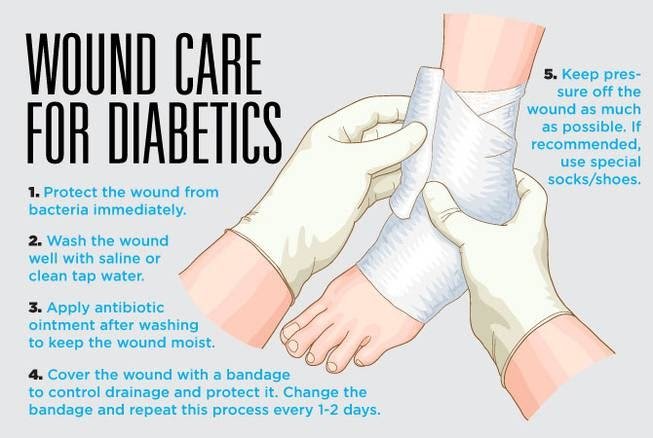
November 4, 2016 by Admin2
Diabetes is a deadly and life-threatening disease that can bring about unbearable pain and discomforts that are enough to affect the way we live. This includes loss of energy, increased hunger with no appetite, lack of interest and focus, loss of vision, and loss of efficiency for the body to heal wounds. One of the major effects of diabetes is the painful and grotesque wounds that form under your heels. This is called Diabetic foot ulcers and they are serious symptoms of diabetes that can lead to even more complications.
Diabetic foot ulcer is an open wound that occurs under or at the side of your foot and toes. These are painful and can sometimes leak out blood and pus. Diabetic ulcers are formed as a result of changes in the bony shapes of the foot. Other causes are peripheral neuropathy and diseases in the artery. Diabetic foot ulcers can also be caused by wearing tight footwear, rigorous exercises, and getting wounded in the foot.
More than 90% of diabetic patients experience diabetic foot ulcers, and 15% of these patients have been hospitalized due to inflammation and infection. While it is hard to heal diabetic foot ulcers, it is best not to leave them alone for flies and germs to gather around to prevent worsening the condition.
Here are ways you can treat your diabetic foot ulcers:
Also Check: Which Pancreatic Cells Release Insulin And Glucagon
Ayurvedic Home Remedies For Treating Diabetic Ulcer
Ayurveda is a perfect remedy to treat any kind of health issues. From the ancient time, people are following herbal medicines for having a healthy and happy life. Ayurveda helps in avoiding all health complications and understands the root cause of disease and then manage and treat health problems. We have mentioned the Best Home Remedies to treat Diabetic Ulcer as follows.
How To Promote The Healing Of Chronic Wounds And Diabetic Ulcers
Diabetes is the leading cause of foot amputation in the United States, which is why immediate treatment is essential with chronic wounds like diabetic ulcers. At the first sign of a chronic wound or diabetic ulcer, see your doctor as soon as possible. Diabetes causes healing impairments and its always better to seek professional help. The sooner your wound is treated, the lower your risk for complications. Wound Care Centers are the best place for chronic wound treatment, so talk to your doctor for recommendations as a proactive measure.
To promote the healing of chronic wounds and diabetic ulcers, your doctor will assess the wounds seriousness and create a treatment plan. Some of the treatment options include the following:
The best way to promote healing in chronic wounds like diabetic ulcers is to properly manage your diabetes. Byram Healthcare has a range of products to help you monitor your blood glucose levels with ease. If youre faced with healing a chronic wound, our wound care product selection guide has everything you need to support your doctors treatment plan.
Read Also: Can Type One Diabetics Donate Blood
What Are A Diabetic Ulcer And Its Symptoms
Diabetic Ulcer is a medical issue mostly occurs in diabetes patients. It is a kind of infection which is dangerous for the individual. Therefore, it needs on time treatment for maintaining good health. It occurs due to the fail in veins for pushing the blood towards the heart, it actually flows back into the legs, eventually causing ulcers. All the arteries in the legs are blocked. In this problem, it shows the following symptoms which help in depicting the ulcer infection.
-
Swelling in wounds
-
Irritation
-
Hard Skin
These symptoms often vary from individual to individual. Although it might get disappear in a few days, some may be non-healing. Therefore, it is important to prevent further complications so better to diagnose it first. Better to visit a doctor and in some cases, your doctor may refer you to a vascular specialist if he is not able to confirm your condition.
How Does Diabetes Increase The Risk Of Leg Ulcers
Neurotrophic ulcers, from nerve damage, affect diabetics who have high blood sugar levels.
These ulcers form most often at pressure points on the bottom of the feet. The ulcer may be discolored, pink, red, brown, or black, and is an open wound. The surrounding skin is often discolored and calloused.
Nerve damage to the legs or feet can cause symptoms such as a loss of feeling, changes to sweat glands, tingling, a burning or stinging feeling, and pain. These are predictive signs of a potential ulcer. Anyone with these symptoms should talk with a doctor and get checked.
People with diabetes should check their legs and feet frequently. Make sure there are no calluses, scrapes, or cuts. Wear good, closed footwear, never walk barefoot, and keep your legs and feet clean.
Also Check: What Happens If You Stop Taking Diabetes Medication
What Is The Outlook For People With Diabetic Foot
Diabetic foot ulcers are fairly common in people who have had diabetes for a long time. Even with foot checks and careful blood glucose monitoring, some people with diabetes develop infections.
The outlook depends on factors such as:
- How early the wound was found.
- Presence of infection and how much it spreads.
- Treatment effectiveness.
If the infection cant be controlled and spreads too far, amputation may be necessary.
What Types Of Physicians Specialize In Treating Diabetic Foot Ulcers
The doctors that are qualified to treat diabetic foot ulcers include wound care specialists, orthopedic surgeons, vascular surgeons, and endocrinologists.
- Wound care specialists are clinicians who have received specialized training in caring for and treating all wounds, both acute and chronic. One of the most treated wounds are diabetic wounds. The percentage of these wounds that become stubborn and refuse to heal is high. This creates an issue with the patients quality of life.
- Podiatrists are foot health specialists who are specially trained in treating all injuries and illnesses pertaining to the feet, including the diagnosis and treatment of diabetic ulcers.
- Orthopedic surgeons can offer prevention measures to patients who have diabetic foot ulcers. Long-term protection of the feet is provided to patients by Orthopedists subscribing footwear that will protect them in the future. The surgeon can also correct bunions, hammertoes, and deformities in the feet to avoid the formation of an ulcer.
- A vascular surgeon does not directly treat diabetic foot ulcers. They are involved in the treatment of peripheral arterial disease, which is a critical catalyst for the impediment of blood flow to the lower legs and feet.
- Endocrinologists are specially trained physicians who address several conditions, including diabetes. An endocrinologist will be the doctor who will make referrals to the other specialists mentioned here.
Recommended Reading: Does Type 2 Diabetes Need Insulin
Diabetic Foot Ulcer: Treatment And Prevention
Estimates are that by 2030 there will be 550 million individuals with diabetes in the world. Because almost a quarter of all people with diabetes will develop a foot ulcer at some point, health care workers need to know the best practices for diabetic foot ulcer prevention and treatment.
Determining which diabetic foot ulcer type is important to determine an effective treatment. Here are the different types of these wounds:
- Neuropathic ulcers arise when the nerve damage from diabetic neuropathy causes the individual with diabetes to not feel pain from an injury, which often leads to the ulcer progressing substantially before the person is even aware of it. Foot and toe deformities, corns, calluses and areas repetitive stress are likely places of injury. Footwear can not only hide these issues, but can exacerbate the injury if the shoe is ill-fitting.
- Ischemic ulcers or arterial ulcers as they are sometimes called may occur due to lack of blood flow to the extremity. When an ulcer occurs as the result of an injury to the extremity, the lack of blood flow makes these ulcers difficult to heal.
- Neuroischemic ulcers occur in individuals with both neuropathy and poor arterial blood flow and are the most difficult to heal.
- Infected wounds occur in about half of patients with a diabetic foot ulcer and require particularly close care.

