Cleveland Clinic Heart Vascular & Thoracic Institute Vascular Medicine Specialists And Surgeons
Choosing a doctor to treat your vascular disease depends on where you are in your diagnosis and treatment. The following Heart, Vascular & Thoracic Institute Sections and Departments treat patients with all types of vascular disease, including blood clotting disorders:
Section of Vascular Medicine: for evaluation, medical management or interventional procedures to treat vascular disease. In addition, the Non-Invasive Laboratory includes state-of-the art computerized imaging equipment to assist in diagnosing vascular disease, without added discomfort to the patient. Call Vascular Medicine Appointments, toll-free 800-223-2273, extension 44420 or request an appointment online.
Department of Vascular Surgery: surgery evaluation for surgical treatment of vascular disease, including aorta, peripheral artery, and venous disease. Call Vascular Surgery Appointments, toll-free 800-223-2273, extension 44508 or request an appointment online.
You may also use our MyConsult second opinion consultation using the Internet.
The Heart, Vascular & Thoracic Institute also has specialized centers and clinics to treat certain populations of patients:
How Can I Address My Diabetic Foot Ulcers
Keep The Blood Flowing To Your Feet
Try the following tips to improve blood flow to your feet:
- Put your feet up when you are sitting.
- Wiggle your toes for a few minutes throughout the day. Move your ankles up and down and in and out to help blood flow in your feet and legs.
- Do not wear tight socks or elastic stockings. Do not try to hold up loose socks with rubber bands.
- Be more physically active. Choose activities that are easy on your feet, such as walking, dancing, yoga or stretching, swimming, or bike riding.
- Stop smoking.
Smoking can lower the amount of blood flow to your feet. If you smoke, ask for help to stop. You can get help by calling the national quitline at 1-800-QUITNOW or 1-800-784-8669. For tips on quitting, go to SmokeFree.gov.
You May Like: Which Pancreatic Cells Release Insulin And Glucagon
Open Sores And Wounds
Having high blood sugar for a long time can lead to poor circulation and nerve damage. You may have developed these if youve had uncontrolled diabetes for a long time.
Poor circulation and nerve damage can make it hard for your body to heal wounds. This is especially true on the feet. These open wounds are called diabetic ulcers.
Diabetes and feet
- Get immediate medical care for an open sore or wound.
- Work with your doctor to better control your diabetes.
What Is A Diabetic Foot Ulcer
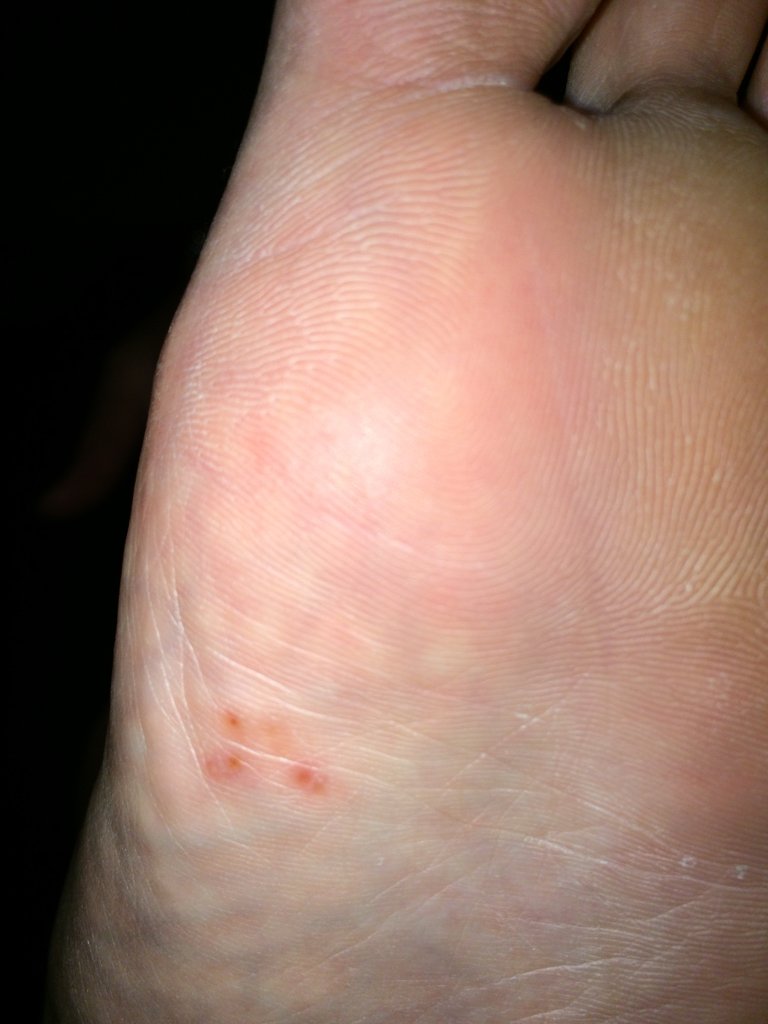
A diabetic foot ulcer can be redness over a bony area or an open sore. The ulcer can develop anywhere on your foot or toes. Ulcers usually develop on the bottom of the foot. You may not know you have an ulcer until you notice drainage on your sock. Drainage is fluid that may be yellow, brown, or red. The fluid may also contain pus or blood.
You May Like: How Many Points Does Metformin Lower Blood Sugar
Diabetes: 12 Warning Signs That Appear On Your Skin
Diabetes can affect many parts of your body, including your skin. When diabetes affects the skin, its often a sign that your blood sugar levels are too high. This could mean that:
-
You have undiagnosed diabetes, or pre-diabetes
-
Your treatment for diabetes needs to be adjusted
If you notice any of the following warning signs on your skin, its time to talk with your doctor.
Could You Have Nerve Damage
Anyone with diabetes can develop nerve damage, but these factors increase your risk:
- Blood sugar levels that are hard to manage
- Having diabetes for a long time, especially if your blood sugar is often higher than your target levels
- Being overweight
- Having high cholesterol
Nerve damage, along with poor blood flowanother diabetes complicationputs you at risk for developing a foot ulcer that could get infected and not heal well. If an infection doesnt get better with treatment, your toe, foot, or part of your leg may need to be amputated to prevent the infection from spreading and to save your life.
When you check your feet every day, you can catch problems early and get them treated right away. Early treatment greatly reduces your risk of amputation.
Read Also: Can Diabetics Eat Macaroni And Cheese
When To See Your Doctor
If you begin to see blackened flesh around an area of numbness, see your doctor right away to seek treatment for an infected foot ulcer. If untreated, ulcers can cause abscesses and spread to other areas on your feet and legs.
At this point, ulcers can often only be treated by surgery, amputation, or replacement of lost skin by synthetic skin substitutes.
What Are Some Symptoms Of Foot Ulcers
Diabetic foot ulcers are painful, but because many patients have extreme nerve damage, they may not feel pain as a symptom.
Upon examination, patients might notice drainage on their socks. They may also notice that their feet are red, swollen, and possibly abnormally smelly.
Its important to check your feet often and be on the lookout for any unusual firmness or numbness. In some cases, patients may not have apparent symptoms, and the ulcer may not be discovered until its already become infected. Due to this risk, its important to talk to your doctor about any changes to your feet if youre at risk for diabetic ulcers.
You May Like: Which Pancreatic Cells Release Insulin And Glucagon
Who Can Get A Diabetic Foot Ulcer
Anyone who has diabetes can develop a foot ulcer. Native Americans, African Americans, Hispanics and older men are more likely to develop ulcers. People who use insulin are at a higher risk of developing a foot ulcer, as are patients with diabetes-related kidney, eye, and heart disease. Being overweight and using alcohol and tobacco also play a role in the development of foot ulcers.
How To Treat Ulcers
If you do get an ulcer or notice a change in your skin that youâre not sure about, tell your doctor right away. Youâll likely get a procedure called debridement, which removes unhealthy tissue from the wound to spur healing.
Your doctor will also work with you to try to keep your sore or ulcer from getting infected and becoming bigger. Some of the steps they may recommend include:
Clean your ulcer daily. Use soap and water, unless your doctor recommends another cleanser. Donât use hydrogen peroxide or soak your wound in a bath or whirlpool, because this could reduce healing and may boost your odds of infection.
Keep your ulcer bandaged or covered with a wound dressing. While you may have heard that itâs important to âair outâ wounds, experts now know that not covering a wound actually increases the odds of infection and slows healing.
Keep pressure off your ulcer, especially if itâs on your foot. This may mean you need to use crutches, special footwear, a brace, or other devices. Reducing pressure and irritation helps ulcers heal faster.
Use the topical medications your doctor recommends. These may be saline, growth factors, and/or skin substitutes.
Keep your blood sugar under control. In addition to reducing your risk of ulcers, tight blood sugar control helps your body heal existing ulcers.
Read Also: Type 2 Diabetes Genes
What Does Diabetic Foot Ulcer Look Like
Diabetic foot ulcer is an external open sore that answers the medical treatment with a significant difficulty. It becomes as a red sore on the skin accompanied with diabetic foot discoloration and located commonly on the big toe or pad but not limited to. It can damage any place lower the ankle and continuously grow in size.
Why does it appear? It starts because of trauma of any nature. A diabetic can struggle in tight shoes or get minor cut, or even have just closed wound any mentioned reason is enough for diabetic ulcer of foot to progress.
What does a foot ulcer look like? This is a crater going deep into the flesh exposing tendons and reaching bones in severe cases. It is usually surrounded by rough skin. The most unpleasant thing with all the above is infection that is ready to develop into osteomyelitis, abscess and in the long run into gangrene.
Among the signs of infection there are unpleasant odor and foul drainage. The liquid is checked for mal cultures. If the nerves are healthy a patient feels pain especially if ulcer of heel happen to be when it is impossible to avoid touching the damaged place. If the nerves do not function properly, a person with this health condition can even be unaware of the problem.
How Do I Know If I Have A Diabetic Foot Ulcer
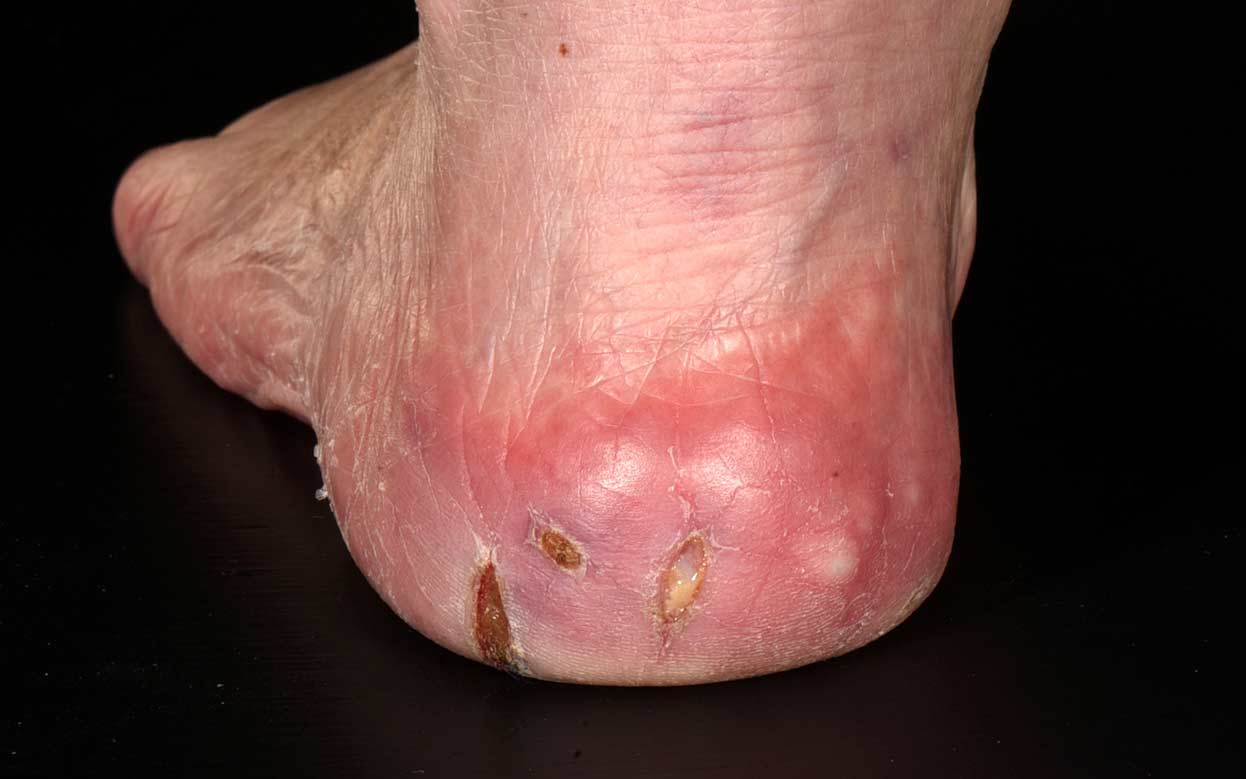
To know if you have a diabetic foot ulcer, its important to understand both the key causes and symptoms of diabetic foot ulcers. A foot ulcer is an open sore on the foot. These often develop under a callus from pressure and rubbing. They may also result from an injury or trauma to the foot. They usually occur on the bottom of the foot, as that is the part of the foot that makes contact with the ground. Foot ulcers are a result of the skin and tissue of the foot breaking down, leading to an open sore that can get infected if not treated promptly. These types of wounds are common among diabetic patients due to nerve damage and loss of sensation, known as neuropathy. Once you lose the feeling of the foot, you can no longer feel the rubbing or injury to the foot. Typically a blister from walking tells us to slow down or stop walking to allow the area to heal. However, with neuropathy, the body can no longer tell us there is a problem. Diabetes and smoking can cause poor circulation, which slows down healing
There are a number of common symptoms of a diabetic foot ulcer:
- Irritated skin from friction while walking
- Pain,
- Bleeding on a sock or floor
- Odor and/or swelling
- Tissue that looks black or discolored
If you believe you have a diabetic foot ulcer, call one of our convenient locations today to book an appointment at 732-838-FEET . We look forward to restoring you to the best quality of life possible.
Recommended Reading: How Many Points Does Metformin Lower Blood Sugar
Foot Ulcer Prevention Tips
The best way to prevent an ulcer on the foot from forming in the first place is to treat the underlying health problem. In diabetes, keeping blood sugar at normal levels will help prevent some of the complications that can lead to foot ulcers.
Heres what else you can do to keep a step ahead of foot ulcers:
Vlahovic says if you have diabetes, its important to develop a good relationship with a podiatrist. This foot specialist can assess whether you are at higher risk for developing a foot ulcer and give you the regular care you need so that a small problem doesnt turn into a major one.
Do You Need The Help Of An Experienced And Caring Podiatrist
If you’re experiencing any type of foot pain, you should speak with an experienced podiatrist as soon as possible. Please contact us online to schedule your appointment or call one of our convenient El Paso offices directly. To reach our Sierra Tower Building podiatrist office please call 915.533.5151. You can find driving directions here. To reach our George Dieter Drive podiatry office please call 915.856.3331. Driving directions are available here.
|
Related Links: |
You May Like: Does Low Blood Sugar Mean You Have Diabetes
How Can I Prevent It
-
Control blood sugar levels to prevent damage to blood vessels and nerves.
-
Check your feet, including between your toes, every day for sores and cuts. Tell your doctor right away if you notice a problem.
-
Have your doctor check your feet at least once a year.
-
Keep your feet clean, dry, and warm.
-
Always wear shoes that fit well to avoid rubbing and pressure. Don’t go barefoot, even at home, because this increases the risk of injury.
-
Trim your toenails along the shape of the toe and file the nails to remove sharp edges.
-
If you have nerve damage, don’t trim toenails yourself. You should see your doctor or a podiatrist for even minor foot procedures.
-
Do not smoke.
Foot Problems That Might Mean You Have Diabetes
Did you know there is a connection between your feet and diabetes? Diabetes is a condition in which the level of glucose in the blood is too high. This is caused by a problem with the hormone insulin and its role in controlling blood glucose levels. Diabetes may lead to higher risk of health complications including developing foot problems.
Every five minutes an Australian develops diabetes
The number of people with diabetes in Australia is three times higher today than it was 25 years ago. Every day, 280 Australians develop diabetes. Thats around one person every five minutes. Around 1.7 million Australians have diabetes and dont even know it.In the Yarra Ranges, the number of people with diabetes has risen by nearly 180% over the past ten years and each week seven new cases are diagnosed.
Is diabetes affecting you feet?Having diabetes may increase your risk of developing related complications that include nerve damage or poor circulation in your feet. Nerve damage may affect how you feel pressure or pain and may lead to numbness in your toes or feet. Changes to your circulation may delay your ability to heal any cuts or sores, and may also increase your risk of developing ulcers that could even lead to amputations.
Seven signs to look out for
As feet are often the first place to show diabetes-related symptoms, it is important to get your feet checked by a podiatrist. Here are 7 signs and symptoms to look out for include:
What you can do to look after your feet
Don’t Miss: How Many Points Does Metformin Lower Blood Sugar
How Can Diabetes Affect My Feet
Over time, diabetes may cause nerve damage, also called diabetic neuropathy, that can cause tingling and pain, and can make you lose feeling in your feet. When you lose feeling in your feet, you may not feel a pebble inside your sock or a blister on your foot, which can lead to cuts and sores. Cuts and sores can become infected.
Diabetes also can lower the amount of blood flow in your feet. Not having enough blood flowing to your legs and feet can make it hard for a sore or an infection to heal. Sometimes, a bad infection never heals. The infection might lead to gangrene.
Gangrene and foot ulcers that do not get better with treatment can lead to an amputation of your toe, foot, or part of your leg.A surgeon may perform an amputation to prevent a bad infection from spreading to the rest of your body, and to save your life. Good foot care is very important to prevent serious infections and gangrene.
Although rare, nerve damage from diabetes can lead to changes in the shape of your feet, such as Charcots foot. Charcots foot may start with redness, warmth, and swelling. Later, bones in your feet and toes can shift or break, which can cause your feet to have an odd shape, such as a rocker bottom.
Get The Facts On Foot Ulcers
Some people with certain chronic health conditions are at a greater risk of developing an ulcer on the foot. Here’s how to stay one step ahead of foot ulcers.
Foot ulcers are sores on the feet that can involve just the skins surface or can develop into more serious wounds, possibly leading to the loss of a limb. People with chronic conditions, such as diabetes, are particularly susceptible to foot ulcers. In fact, about 15 percent of all people with diabetes will develop a foot ulcer at some point in their lives. Practicing good foot care can put the brakes on foot ulcers before they start.
9 Warning Signs of Type 2 Diabetes
Tracey Vlahovic, DPM, associate professor at the Temple University School of Podiatric Medicine in Philadelphia, says that leg and foot ulcers can be a problem for people with nerve damage due to alcoholism, those with vascular issues, atherosclerosis , and sickle cell anemia, among other conditions. However, diabetes is the No. 1 culprit, she adds.
Those with diabetes are more susceptible to developing an ulcer on the foot because of reasons including:
Peripheral neuropathy. This is a common complication of diabetes, especially in people who have had the disease for years. Peripheral neuropathy is damage to nerves that numbs the extremities to pain, heat, and cold. If your foot gets injured, that nerve damage may prevent you from feeling it. Walking on a wounded or irritated foot day after day causes a foot ulcer to form.
Treatment for Foot Ulcers
You May Like: Does Bananas Affect Blood Sugar
How To Prevent Diabetic Foot Ulcers
The first line of defense in preventing diabetic wounds is to follow the guidelines recommended to keep the disease itself under control:
- Maintain healthy blood sugar levels through a healthy diet and by taking medications as instructed by your doctor.
- Keep your blood pressure within a healthy range.
- Avoid alcohol and tobacco.
You should also take measures to avoid causing sores or wounds on the feet:
- Never walk barefoot.
- Wear shoes that fit properly and dont rub the skin.
- Wash your feet daily with mild soap and lukewarm water to prevent the buildup of bacteria on the skin, which can cause infection even in the tiniest skin breaks.
Because a loss of sensation in the feet may mean theres no pain felt even when an ulcer is present, its also extremely important for those with diabetes to regularly check for any foot sores or skin irritation. This way, the ulcer can be properly treated as early as possible.

