Efficacy Of Treatment With A Basalprandial Insulin Regimen In Patients With Type 2 Diabetes Mellitus Previously Treated With Premixed Insulin
Premixed insulins are a common treatment for type 2 diabetes mellitus . However, their limitations and the lack of achieving glycaemic control in some patients reinforce the need to find therapeutic alternatives. To assess whether basal–prandial therapy improves glycaemic control in patients with type 2 DM and glycosylated haemoglobin >53mmol/mol treated with premixed insulin in the primary care setting. A retrospective observational study in which 116 patients with type 2 DM switched from premixed insulin to basal–prandial therapy. Data on demographics, anthropometrics, laboratory results, and antidiabetic treatment were collected from the medical charts of the patients, prior to switching the treatment and 4 months thereafter. HbA1c significantly decreased from baseline to month 4 , and 70 patients had an HbA1c ?53mmol/mol . Additionally, fasting blood glucose significantly decreased , and the number of patients with FBG<5.6mmol/l , and with post-prandial blood glucose ?10mmol/l significantly increased. There were also significant decreases in body weight and waist circumference . Only 4 patients had hypoglycaemia. Basal–prandial therapy improved glycaemic control in patients with type 2 DM, with a low incidence of hypoglycaemia, and decreased body weightContinue reading >>
What Is Basal Insulin Benefits Side Effects Types And Everything Else You Need To Know
Your body needs insulin to function properly, and the right dose of basal insulin may be the answer to stabilizing your blood sugar and avoiding diabetes complications.
Valencia HigueraKacy Church, MDThinkstock
Insulin is a hormone that everyone needs. It allows the body to use sugar properly. But if you have type 1 diabetes or type 2 diabetes, your body doesn’t make or use insulin properly, which means you may have to give yourself insulin injections on a daily basis.
Insulin isn’t one-size-fits-all. There are different insulins you can use to control your blood sugar levels, and they’re classified by how quickly they work. Basal insulin is one type of therapy. And if you require this insulin, it’s important to understand how it works and how it differs from other types of the drug.
Example #4: Formulas Commonly Used To Create Insulin Dose Recommendations
This example illustrates a method for calculating of your background/basal and bolus doses and estimated daily insulin dose when you need full insulin replacement. Bear in mind, this may be too much insulin if you are newly diagnosed or still making a lot of insulin on your own. And it may be too little if you are very resistant to the action of insulin. Talk to your provider about the best insulin dose for you as this is a general formula and may not meet your individual needs.
The initial calculation of the basal/background and bolus doses requires estimating your total daily insulin dose:
The Takeaway: The Right Dose And Type Of Insulin For A Healthy Life
Insulin is instrumental in energizing your body. If your body doesn’t make insulin or use insulin properly because of type 1 or type 2 diabetes, basal injections can help stabilize your blood sugar and reduce the likelihood of diabetes complications like kidney damage, eye damage, nerve damage, and heart problems.
Make sure you follow your doctor’s instructions and take your insulin as prescribed. If you feel your insulin isn’t working effectively, speak to your doctor about fine-tuning your dosage.
Does Living With Type 2 Diabetes Mean You Need To Take Insulin
Not always. Many people living with type 2 diabetes may not need basal insulin, or at least not right away. Because your body is still able to produce insulin, dietary changes, physical activity, and oral medication may help your body overcome insulin resistance and use this hormone properly.
Losing weight and adding 30 minutes of regular physical activity five days a week can help your body respond to its own insulin so your cells can naturally absorb glucose.
You can also help improve your body’s response to its own insulin by eating fewer starchy, sugary foods, and eating more low-calorie foods like fruits and vegetables. Your doctor may also prescribe the oral medication Glucophage , which helps control high blood sugar by limiting the amount of sugar produced by the liver.
If diet, lifestyle changes, and medication aren’t enough to control your blood sugar, you may need to consult your doctor about adding basal insulin your treatment regimen.
Signs that you may need insulin therapy include:
- Increased thirst
RELATED: What Is Insulin?
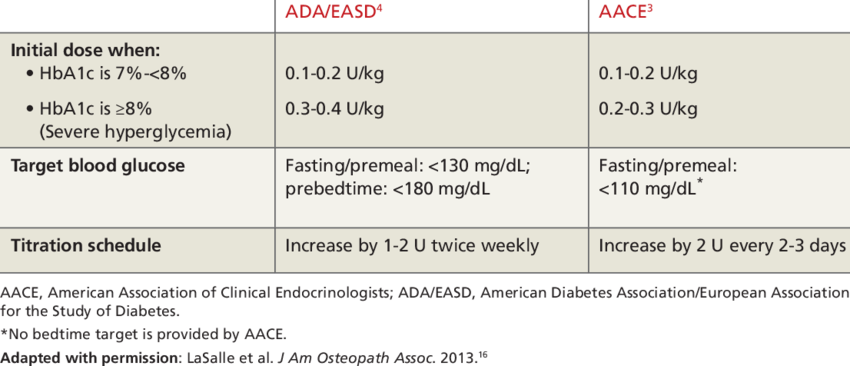
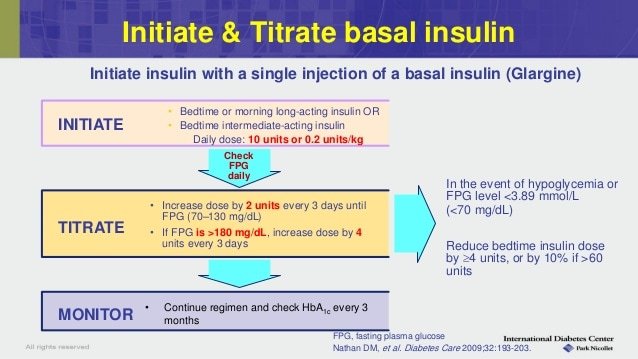
How To Decide Upon The Insulin Dose When Starting The Basal
Patients who were already on a basal-bolus insulin regimen prior to admission and have good blood glucose control can be continued on the same doses of insulin. Further adjustments can be made based on capillary blood glucose monitoring as detailed in the following sections of this review. For patients who are insulin naïve, insulin therapy can be initiated at an empirical total daily dose of 0.4 units/kg/day . The TDD should be reduced to 0.2 units/kg/day in elderly patients and in those with renal dysfunction, liver disease, cardiac disease, autonomic neuropathy or hypoglycaemia unawareness due to the heightened risk of hypoglycaemia and its associated complications in this patient subgroup.
In the scenario in which regular insulin is used for prandial coverage, the calculated TDD is divided equally into four portions, with the implication of one portion for the basal insulin injection and one portion each for the three prandial insulin injections . However, when an insulin analogue is used for prandial coverage, the TDD should be divided into 50% for basal insulin and 50% for prandial insulin .
What Is Basal Insulin And How Can It Help Control Diabetes
Basal insulin is an important component in diabetes management because it acts as a background insulin. It’s designed to stabilize your blood sugar during periods of fasting, such as in between meals and while you’re asleep.
Insulin also plays a role in how you metabolize carbohydrates. After eating, your body breaks down carbs from food into sugar or glucose to energize your body and enable you to walk, eat, perform tasks at work, and more. This breakdown increases your blood sugar level, and in response to this higher level, your pancreas releases insulin into your bloodstream.
RELATED: How to Stabilize Your Blood Sugar
Insulin helps your body’s cells absorb the glucose in your bloodstream, providing you with that essential energy. Some glucose remaining in your blood gets stored in your liver, and then slowly forms and releases into your bloodstream when there’s a demand for fuel.
Because people with type 1 diabetes don’t make their own insulin, they need to take injections of basal insulin to manage their blood sugar. But if you have type 2 diabetes, your body still produces insulin. The issue is your pancreas may not produce enough insulin to maintain a healthy glucose level. That’s why your doctor may recommend using basal insulin at some point in your treatment. Between 75 percent and 90 percent of people with type 2 diabetes require injections.
What Are The Risks And Advantages Of Taking Basal Insulin
The main risk when using insulin is a higher risk of hypoglycemia or low blood sugar, especially if you change the physical activities you are used to, such as walking a little more or doing more intense exercises, or taking more insulin than recommended. However, this can be avoided by using a glucose monitoring device to know how glucose behaves throughout the day. Learn more about hypoglycemia and how to prevent it if it happens. Another risk is skipping or using less insulin than prescribed, which leads to high blood glucose.
The advantage of taking insulin is the several ways in which it can help us achieve better glucose management with higher a time in range delaying or preventing the risk of diabetes complications. The downside is that taking it requires injections.
Type 2 Diabetes Mellitus: Outpatient Insulin Management
AMANDA HOWARD-THOMPSON, PharmD, Veterans Affairs Medical Center, Memphis, Tennessee
MUNEEZA KHAN, MD, University of Tennessee Health Science Center, Memphis, Tennessee
MORGAN JONES, PharmD, MS, Cleveland Clinic Independence Family Health Center, Independence, Ohio
CHRISTA M. GEORGE, PharmD, University of Tennessee Health Science Center, Memphis, Tennessee
Am Fam Physician. 2018 Jan 1;97:29-37.
Type 2 diabetes mellitus is a chronic, progressive disease characterized by multiple defects in glucose metabolism, the core of which is insulin resistance in muscle, liver, and adipocytes and progressive beta cell failure.1 Beta cell failure progresses at a rate of approximately 4% per year, requiring the use of multiple medications, often including insulin, to attain and maintain glycemic control.2
Data from the National Health and Nutrition Examination Survey show that the percentage of U.S. adults with diabetes and an A1C level of more than 9% decreased slightly between 2003 to 2006 and 2007 to 2010, from 13% to 12.6% .3 According to the Centers for Disease Control and Prevention, from 2010 to 2012, 57% of patients with type 2 diabetes used only oral diabetes medications.4 Thus, it is likely that many patients who should be receiving insulin therapy are not. American Family Physician recently published a review of noninsulin therapies for type 2 diabetes.5 Our article reviews insulin management in the outpatient setting.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
A Practical Guide To Basal And Prandial Insulin Therapy
A practical guide to basal and prandial insulin therapy. Separating basal and meal-related insulin requirements allows a systematic approach to subcutaneous insulin therapy. Simple guidelines for both the doctor and patient can cater for the spectrum of severity of diabetes. A non-insulin-dependent diabetic who, despite dieting, continues to have moderate fasting hyperglycaemia may need only a basal insulin supplement, whereas a totally insulin-dependent diabetic usually needs similar amounts of basal and meal-related insulin. The likely insulin requirements of individual diabetics can be predicted, including the increased amounts required by obese patients. The algorithms have been developed using ultralente to provide the basal insulin requirement, but the principles and doses probably apply to other similarly long-acting insulins or an insulin pump. The insulin doses can be easily altered for varying lifestyles, including night work, religious fasts or long distance aeroplane travel, and for temporary disturbances such as operations or intercurrent infections.Continue reading >>
Understanding The Segment Of The Day When Insulin Works
Each insulin dose in the basal-bolus regimen works during a particular segment of the day. Prandial insulin administered before breakfast predominantly acts from breakfast to lunch ; prandial insulin given before lunch predominant acts from lunch to dinner ; prandial insulin given before dinner predominantly acts from dinner to midnight ; and basal insulin given at bedtime predominantly acts from midnight to breakfast . Although there may be some overlap in action, this broad concept helps the clinician to determine the appropriate dose adjustment based upon the demarcation of the segment during which blood glucose targets are not achieved.
Maternal Complications Associated With Insulin Therapy
3.8.1 Maternal hypoglycemia
Hypoglycemia threshold is specific for every individual. In pregnancy, there is a reduction of this threshold by 20% . Patients with GDM that are treated with insulin must maintain a glycemia above 3.7 mmol/l according to CDA, or above 3.9 mmol/l according to ADA .
Insulin analogs are superior to human insulin because the hypoglycemic events are less frequent in type 1 diabetic pregnancies . The use of multiple daily injections is as effective as continuous subcutaneous insulin infusion .
Maternal hypoglycemia affects the fetus just in severe cases when is associated with loss of consciousness or secondary to trauma. Also, it was observed that repeated episodes could lead to growth over the 90th percentile . These episodes are more likely to be present in the first trimester in women who had pregestational diabetes than in GDM .
3.8.2 Hypertension
There is moderate quality evidence that indicates higher hypertension associated hypertension without giving details in insulin-treated GDM. This fact should be further researched because it is in contradiction with a non-modified risk for pre-eclampsia .
Whats The Difference Between Basal And Bolus Insulin

Along with basal insulin, bolus insulin is a treatment option for type 2 diabetes.
While basal insulin works as a background insulin to supply your body with insulin during periods of fasting, bolus insulin is a rapid or fast-acting insulin that works quickly, but there’s a catch: Its blood-sugar-lowering effect doesn’t last as long.
Important Factors To Consider In Patients With Covid
Pre-analytical factors, such as blood pH, hypoxia, hypotension and extreme hematocrit concentrations, can affect the performance of capillary blood glucose monitoring and should be given due consideration in the current scenario . While most blood glucose meter test strips use the glucose oxidase method, which is specific for glucose, it is worth mentioning that the glucose dehydrogenase-pyrroloquinolinequinone method is not glucose specific. Consequently, GDH-PQQ can react with other sugars, such as maltose, galactose and xylose, resulting in false high blood glucose readings in the presence of these molecules . Maltose is product of icodextrin metabolism and also a constituent of intravenous immunoglobulin, which is an experimental therapy for patients with severe COVID-19 pneumonia . Erroneously high blood glucose readings leading to fatal insulin dose calculation errors may occur in such scenarios when using a GDH-PQQ-based glucometer . For this reason, GDH-PQQ-based blood glucose meters are not recommended for use in the hospital setting by the US Food and Drug Administration .
You’ll Need To Calculate Some Of Your Insulin Doses
You’ll also need to know some basic things about insulin. For example, 40-50% of the total daily insulin dose is to replace insulin overnight.
Your provider will prescribe an insulin dose regimen for you; however, you still need to calculate some of your insulin doses. Your insulin dose regimen provides formulas that allow you to calculate how much bolus insulin to take at meals and snacks, or to correct high blood sugars.
In A Person With Type 1 Diabetes Or Type 2 Diabetes
In a person with type 1 diabetes: the pancreas constantly tries to produce beta cells in order to make insulin, but the immune system continues to attack and destroy most or all of those beta cells.
For those with type 1 diabetes, the evolution of the disease and the attack on the beta cells occurs very quickly, which means people get sick very quickly. Often mistaken at first for the lingering flu, a simple blood test and urine test can determine and diagnose type 1 diabetes.
Immediately upon diagnosis, patients should begin taking pharmaceutical insulin via pump, pen, or syringe.
In a person with type 2 diabetes:the body is either struggling to produce a normal amount of insulin , or the body is struggling with severe insulin resistance which makes it difficult to manage healthy blood sugar levels with the available amount of insulin.
For those with type 2, the struggle to properly produce or make use of their own insulin is usually a slower process, sometimes taking years before you show strong enough symptoms to warrant an HbA1c test,a diagnosis, and eventual treatment.
Fetal Complications Associated With Insulin Therapy
3.6.1 Neonatal hypoglycemia
Glucose is a nutrient that freely crosses the placenta from maternal to fetal circulation, to assure the energy required for growth. Immediately after birth, the glucose source disappears with a physiologic “hypoglycemia” in the blood of the newborn that triggers the secretion of counterregulatory hormones . In GDM pregnancies, the glycemia is continuously raised and determines a consecutive higher secretion of insulin that makes hypoglycemia more severe and prolonged than in normal newborns .
Neonatal transient hypoglycemia could have implications in the neurocognitive development as was shown by magnetic resonance imaging . Also, it has psychological implications on the mother-child relationship because they are separated after birth for treatment. Hence, based on their study results, Voormolen et al. recommend screening all newborns from GDM women in the first 12 hours after birth because the majority of the events occur in this interval, with a higher incidence being in the insulin-treated group .
A series of studies demonstrated that newborns of GDM patients that were treated with metformin had fewer hypoglycemic events than those of women treated with insulin . Insulin analogs have a lower rise in postprandial glycemic values without elevating hypoglycemic risk and should be preferred to human insulins .
3.6.2 Congenital anomalies
Birth Complications Associated With Insulin Therapy
3.7.1 Cesarean section
A Cochrane analysis of 1481 women with GDM showed that in the treatment group there was a higher number of induced labors versus the group with standard antenatal care, but with no difference regarding the number of births by CS . Another meta-analysis did not demonstrate a correlation between the use of different types of insulin-like aspart, lispro and the birth by CS . Although the risk is not influenced by insulin treatment, it can be reduced by induction of labor in 38th–39th week of gestation with better outcomes for the fetus .
3.7.2 Vacuum-assisted birth
Although pre-gestational diabetes raises the risk for vacuum assisted birth , in GDM the risk was similar to that in the general population and could not be related to insulin therapy . A particular situation is with GDM that appeared in pregnancies obtained by assisted reproductive technology where the risk for perinatal and obstetrical complications is probably increased by the adverse effect of hyperglycemia, not by insulin treatment .
3.7.3 Fetal morbidity
Insulin Delivery Options For People With Diabetes
Once you are diagnosed with type 1 diabetes, and for some diagnosed with type 2 diabetes, it’s critical that you begin taking insulin to bring your blood sugar levels back to a healthier, safer range.
Only a few decades ago, there was only one option: sharpening and boiling the same syringe over and over and over to then take injections with insulin that dictated exactly when and how much you could eat. These insulins were first derived from pigs and cows.
Today, thankfully, we have a slew of options for both the type of insulin we want to take and how we want to take it.
Other Factors To Consider When Adjusting Insulin
Self-adjusting can be frustrating sometimes.
You think you’ve factored everything in and then you find yourself caught out by a rogue high or low blood sugar level, seemingly from nowhere.
These things happen and everyone who self-adjusts insulin finds it difficult to factor in everything that could affect blood glucose levels
When Will A Doctor Prescribe The Use Of Insulin
According to the American Diabetes Association Standards of Care, physicians are advised to consider prescribing basal insulin for people with Type 2 diabetes when:
- There is ongoing weight loss
- Symptoms of hyperglycemia are present
- When A1c levels are greater than 10%
- When Blood glucose levels are very high )
However, if the A1c level remains above the target despite taking basal insulin, a doctor may prescribe bolus insulin to supplement when eating.
Taking Detemir Glargine Or Degludec At Bedtime
The continuous flow of these long-acting insulins is one of their main advantages. But, some people find that the detemir and glargine insulin wears off sooner than 24 hours after injection. This can mean higher blood glucose levels at your next scheduled injection. Degludec should last until your next scheduled injection.
First Some Basic Things To Know About Insulin:
- Approximately 40-50% of the total daily insulin dose is to replace insulin overnight, when you are fasting and between meals. This is called background or basal insulin replacement. The basal or background insulin dose usually is constant from day to day.
- The other 50-60% of the total daily insulin dose is for carbohydrate coverage and high blood sugar correction. This is called the bolus insulin replacement.
Bolus – Carbohydrate coverage
The bolus dose for food coverage is prescribed as an insulin to carbohydrate ratio.The insulin to carbohydrate ratio represents how many grams of carbohydrate are covered or disposed of by 1 unit of insulin.
Generally, one unit of rapid-acting insulin will dispose of 12-15 grams of carbohydrate. This range can vary from 4-30 grams or more of carbohydrate depending on an individual’s sensitivity to insulin. Insulin sensitivity can vary according to the time of day, from person to person, and is affected by physical activity and stress.
Bolus – High blood sugar correction
The bolus dose for high blood sugar correction is defined as how much one unit of rapid-acting insulin will drop the blood sugar.
Generally, to correct a high blood sugar, one unit of insulin is needed to drop the blood glucose by 50 mg/dl. This drop in blood sugar can range from 15-100 mg/dl or more, depending on individual insulin sensitivities, and other circumstances.
Insulin Management Of Type 2 Diabetes Mellitus
ALLISON PETZNICK, DO, Northern Ohio Medical Specialists, Sandusky, Ohio
Am Fam Physician. 2011 Jul 15;84:183-190.
Insulin therapy is recommended for patients with type 2 diabetes mellitus and an initial A1C level greater than 9 percent, or if diabetes is uncontrolled despite optimal oral glycemic therapy. Insulin therapy may be initiated as augmentation, starting at 0.3 unit per kg, or as replacement, starting at 0.6 to 1.0 unit per kg. When using replacement therapy, 50 percent of the total daily insulin dose is given as basal, and 50 percent as bolus, divided up before breakfast, lunch, and dinner. Augmentation therapy can include basal or bolus insulin. Replacement therapy includes basal-bolus insulin and correction or premixed insulin. Glucose control, adverse effects, cost, adherence, and quality of life need to be considered when choosing therapy. Metformin should be continued if possible because it is proven to reduce all-cause mortality and cardiovascular events in overweight patients with diabetes. In a study comparing premixed, bolus, and basal insulin, hypoglycemia was more common with premixed and bolus insulin, and weight gain was more common with bolus insulin. Titration of insulin over time is critical to improving glycemic control and preventing diabetes-related complications.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Analogue insulin is as effective as human insulin but is associated with less postprandial hyperglycemia and delayed hypoglycemia.
A Quick Guide To Help You Inject Basal Insulin
Basal insulin requires a daily injection. Options include an insulin pen with a prefilled cartridge containing your insulin dose, or a syringe that you fill with your prescribed dose from an insulin bottle.
Insulin doses vary, and your doctor will determine how much insulin you need to manage your diabetes.
Insulin is not injected into muscles or veins, but rather into the tissue underneath your skin. Your doctor will show you how and where to administer your doses. Most likely, you’ll inject insulin in your abdomen so that it can quickly absorb into your bloodstream. Insulin injected into your arm or thigh takes longer to reach the bloodstream.
Wash your hands and clean the injection site with alcohol before injecting. Grab or pinch a fold of your skin, and then inject the needle at a 90 degree angle. If you’re thin, you may have to inject the needle at a 45 degree angle instead.
Be sure to rotate your injection site. If you inject insulin into the same spot every day, fatty deposits could develop in this area and reduce insulin absorption.
It’s also important that you don’t reuse or share your needles with anyone, and you must make sure your insulin is stored properly and not expired.
An insulin pump may be an option if you take basal insulin along with a rapid-acting insulin before meals. This is a small device that delivers insulin 24 hours per day, depending on your body’s needs. Insulin enters your body through a catheter attached underneath your skin.
Can Subcutaneous Insulin Be Used To Treat Dka
There are controlled studies that have shown subcutaneous regular insulin to be effective in the treatment of DKA. The concern with using subcutaneous insulin is the variable uptake and onset of action. Studies that have compared the use of regular insulin—given intravenously, subcutaneously, and intramuscularly—have shown a more rapid and predictable decrease in hyperglycemia and ketonemia with the IV administration. There are newer studies evaluating the use of lispro insulin subcutaneously with equivalent effect to IV regular insulin. Although it is not yet a standard of care, there may be a future trend of treating DKA in a non–intensive care unit setting with subcutaneous lispro insulin.
Trachtenbarg DE: Diabetic ketoacidosis. Am Fam Physician 71:1705–1714, 2005.
Umpierrez GE, Latif K, Stoever J, et al: Efficacy of subcutaneous lispro insulin versus continuous intravenous regular insulin for the treatment of patients with diabetic ketoacidosis. Am J Med 117:291–296, 2004.

