How The Companies Justify Their Price Increases
With Type 1 diabetes, which affects about 5 percent of people with diabetes in the US, the immune system attacks the insulin-producing cells in the pancreas, leaving the body with little or none of the hormone. In Type 2 diabetes, the pancreas still makes insulin, but the body has grown resistant to its effects. In both cases, patients rely on insulin medication to keep energy from food flowing into their bodies.
The US is a global outlier on money spent on the drug, representing only 15 percent of the global insulin market and generating almost half of the pharmaceutical industrys insulin revenue. According to a recent study in JAMA Internal Medicine, in the 1990s Medicaid paid between $2.36 and $4.43 per unit of insulin by 2014, those prices more than tripled, depending on the formulation.
The doctors and researchers who study insulin say it is yet another example along with EpiPens and of companies raising the cost of their products because of the lax regulatory environment around drug pricing. They are doing it because they can, Jing Luo, a researcher at Brigham and Womens Hospital, told Vox in 2017, and its scary because it happens in all kinds of different drugs and drug classes.
In countries with single-payer health systems, governments exert much more influence over the entire health care process.
The US doesnt do that. Instead, America has long taken a free market approach to pharmaceuticals.
Insulin Cost And Pricing Trends
Tara O’Neill Hayes, Josee Farmer
Executive Summary
- Diabetes cost the United States $327 billion in 2017, becoming the most expensive chronic disease in the nation.
- Insulin costs, before accounting for any rebates or discounts, comprise an estimated $48 billion of the direct costs of treating diabetes after rebates, insulin accounts for 6.3 percent of costs.
- The average list price of insulin increased 11 percent annually from 2001 to 2018, with average annual per capita insulin costs now nearing $6,000. Because patients out-of-pocket costs are typically based on list price, their expenses have risen substantially despite the decrease in net price for many of the most commonly used insulin products over the past several years.
- If the trends of the past decade continue, gross insulin costs in the United States could reach $121.2 billion in total spending by 2024, but if more recent trends of much slower price growth prevail, insulin spending could total $60.7 billion in 2024 .
The Rising Cost of Diabetes
Given the rising costs, it is worth understanding what is driving these increases. This analysis first details increases in insulin prices and offers a projection for how much insulin will cost in the coming years. It then examines what is driving these increases.
The Price of Insulin
Past Price Growth
Insulin Spending in Medicaid
Source: American Medical Association
Insulin Spending in Medicare Part D
Typical Insulin Spending per Patient
Estimating Future Costs
Rebates
Pharma: Biden Freezes Trumps Lower Cost Insulin And Epinephrine Rule
Posted on 01/22/2021
Big pharma is smiling big right now. The big three insulin producers are Eli Lilly and Company, Novo Nordisk A/S, and Sanofi S.A., in which they dominate more than 90% of the world insulin market by value. After swearing-in, U.S. President Joe Bidens HHS froze the Trump administrations December 2020 drug policy that mandates community health centers to pass on all their insulin and epinephrine discount savings to patients.
The rule was finalized in late December 2020. The drug rule was put in place to benefit patients who have a hard time paying for expensive insulin and allergy medication. Former President Trump campaigned on lowering the price of important pharmaceutical drugs like insulin, which is used to treat diabetes, and epinephrine. Diabetes afflicts over a quarter of Medicare beneficiaries and drives billions in Medicare spending every year. More than 20 million Americans have diabetes, in which the body fails to properly use sugar from food due to insufficient insulin, a hormone produced in the pancreas.
Also Check: Do Type 2 Diabetics Take Insulin
The Astronomical Price Of Insulin Hurts American Families
essay
A woman from Minnesota holds up her U.S. bottle of NovoLog insulin and a Canadian box of NovoRapid, which she bought at a pharmacy in Ontario, Canada, June 29, 2019
Drug companies charge more for insulin in the United States than in nearly three dozen other countries RAND researchers examinedand it’s not even close. The average list price for a unit of insulin in Canada was $12. Step across the border into America, and it’s $98.70.
Those differences help explain why insulin has become a symbol of the high cost of American health care. Its prices have shot up in recent years, for reasons that are opaque at best, with those who can least afford it often paying the most. Reining in those prices has become the rare political cause embraced by Democrats and Republicans alike.
This isn’t just some academic question: ‘How do our prices compare with those in other countries?’ said Andrew Mulcahy, a senior policy researcher at RAND who specializes in health care economics and led the study. It’s becoming a very practical question, because there are ideas out there to do something about it, and they can benefit from this kind of analysis.
The U.S. Department of Health and Human Services asked RAND to investigate how American insulin prices compare with those in other parts of the world. Researchers obtained list prices for all types of insulin from 33 countries in Europe, Asia, Australia, and the Americas. Plotted on a graph, the U.S. prices stand alone.
The Role Of Insulin Manufacturers
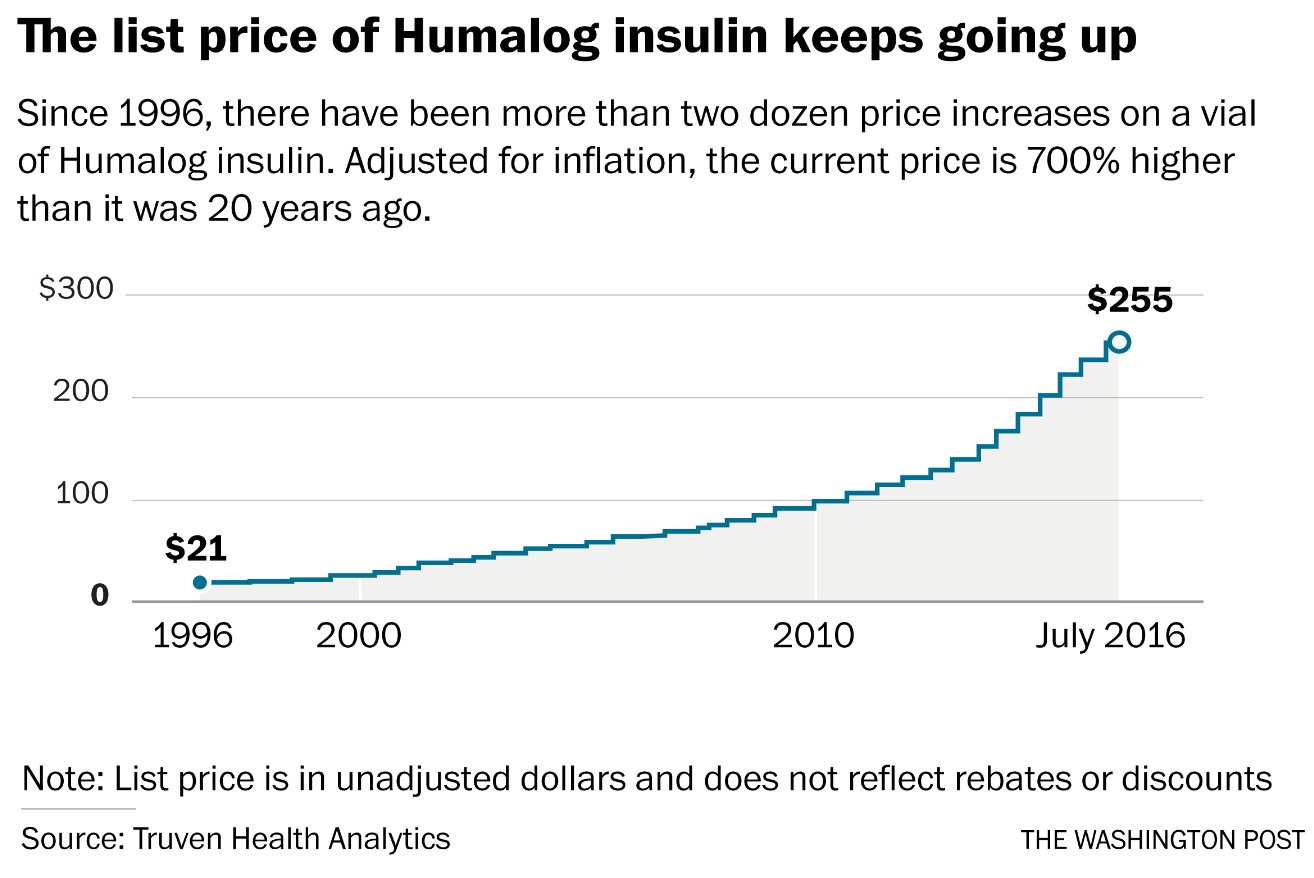
The list price of insulin has risen steeply over time, with the greatest increase over the last fifteen years. For context, one vial of insulin typically lasts an insulin-dependent person anywhere from 5 to 20 days. Most insulin-dependent people require 2-3 vials of insulin per month, while some require 6 or more. Every case of diabetes is unique.
In the late-90s, one vial of analog insulin cost about $25-40 per vial, without insurance. By 2005, this had doubled to about $80, then started sharply increasing about $125 by 2010, $260 in 2015, and depending on the type of insulin up to $275 and sometimes as much as $500 or more for long-acting analog insulins. Experts have stated that, even in a capitalist but competitive market, an insulin-dependent person should be paying $130 or less per year for their insulin needs.
These price hikes are not limited to insulin all drugs, including all glucose regulating medications and most recently, diabetes devices, are subject to the rebates problem. But insulin is certainly where we see one of the clearest examples of how the US healthcare system is broken. Not only do PBMs and insurance companies benefit, but the Senate Finance Committees January 2020 report states that despite the insulin manufacturers saying that they are not making as much off insulin as people say, evidence shows that they are.
The report calls out several clear instances of the pricing increase practices:
Also Check: How To Tell If You Have High Blood Sugar
Advocates Say Senate Report Is Infuriating
When asked to comment on the report, the American Diabetes Association told Medscape Medical News that “the GrassleyWyden report provides important insights into how many business stakeholders have an economic interest in insulin.”
“An array of policy interventions will be needed to create more transparency and to lower costs to patients at the pharmacy counter,” said the ADA’s spokesperson. The ADA is committed to working with Congress and the new administration to ensure these interventions are put in place, the spokesperson said.
On January 12, the Endocrine Society issued a to reduce insulin costs.
Elizabeth Pfiester, executive director of T1International, was much more animated: “For me and T1International’s #insulin4all patient advocate community, the Senate Finance Committee’s report is infuriating because we live the reality of what it means for these companies to put profit over people every hour of our lives,” she said in a statement provided to Medscape Medical News.
Fiona Mason, National Director USA for T1International, told Medscape Medical News that drug makers blaming PBMs for price increases does “not hold up to the scrutiny of the committee’s report.”
T1International is calling on the new Congress to pass and incoming President Joe Biden to sign legislation to immediately lower the list price of insulin.
Mason said, “We will not be managed. We will not stop ‘pushing back.’ We will win #insulin4all.”
Send comments and news tips to .
How The Cost Of Insulin Has Changed
According to research published by the American Diabetes Association, the average price of insulin almost tripled between 2002 and 2013. In the United States, the cost is often passed onto the consumer directly. A study done by RAND Health Care found that the average manufacturer’s price for a unit of insulin in the US was more than 10 times the price in 32 countries.
According to The American Journal of Managed Care, when Eli Lilly first produced its Humalog insulin in 1996, a month-supply cost $21. In 2019, the one-month cost was around $275representing a 1,200% increase. The rate of inflation during that same time period was only 63.67%.
When the cost of insulin became a national talking point, Marissa said she heard a lot of comments about how you can get insulin for $25 a vial at Walmart. In reality, that kind of insulin is an older model that requires patients to follow a strict eating scheduleor experience large blood sugar fluctuations.
“That type of insulin is just not conducive to modern living,” she said.
RELATED: This 25-Year-Old is Living With Type 1 DiabetesHere’s What It’s Like
Within the past two years, eight states passed laws that capped the cost of insulin to $100 or less for a month’s supply. These states include Colorado, Illinois, Maine, New Mexico, New York, Utah, Washington, and West Virginia. That still leaves most of the country without price caps.
You May Like: Does Stress Cause Blood Sugar To Rise
Insulin Makers Middlemen Stonewall Strike Back
“This industry is anything but a free market when PBMs spur drug makers to hike list prices in order to secure prime formulary placement and greater rebates and fees,” Grassley said in a statement.
“Our investigation worked to get to the bottom of this. We found that the business practices of and the competitive relationships between manufacturers and middlemen have created a vicious cycle of price increases that have sent costs for patients and taxpayers through the roof.”
Wyden said, “Insulin manufacturers lit the fuse on skyrocketing prices by matching each other’s price increases step for step rather than competing to lower them, while PBMs, acting as middlemen for insurers, fanned the flames to take a bigger cut of the secret rebates and hidden fees they negotiate.”
The American Diabetes Association notes that determining actual costs to consumers is difficult: “out-of-pocket costs vary depending upon the type of health insurance each individual has and the type of insulin prescribed.”
A study by Ohio-based 3 Axis Advisors of 41,000 prescriptions from more than 1,500 independent pharmacies for a three-pack of Lantus Solostar insulin pens shows an average co-pay of about $34, and a median of about $9, for January through October 2020. About 1 in 12 co-pays topped $110.
J.C. Scott, president and CEO of the Pharmaceutical Care Management Association, the trade group representing pharmacy benefit managers, said in a statement:
‘vicious Cycle’ Sent Insulin Costs Through Roof: Senate Committee
Alicia Ault
US insulin manufacturers and the pharmaceutical benefits management industry are refuting a report by a prominent Senate committee finding that the two sectors acted synergistically to increase the cost of insulin for patients with diabetes.
The Senate Committee on Finance issued findings from a 2-year investigation on January 14, releasing a 90-page report and more than 1700 pages of documents containing internal emails, contracts, and presentations.
“We found that the business practices of and the competitive relationships between manufacturers and middlemen have created a vicious cycle of price increases that have sent costs for patients and taxpayers through the roof,” said Committee Chairman Chuck Grassley in a statement.
“This industry is anything but a free market when PBMs spur drug makers to hike list prices in order to secure prime formulary placement and greater rebates and fees,” Grassley said.
You May Like: How Do You Treat Diabetic Blisters
Vials Are Cheaper Than Newer Dispensers
In 1985, Novo Nordisk introduced the first insulin pen, making it more convenient for patients to store and self-inject insulin but it came at a price. Today, retail prices of rapid-acting insulins can be over $200 more expensive if you opt for pens instead of vials. This trend isnt just relevant to rapid-acting insulins the average retail price of , for example, more than doubles if you choose to use a FlexPen instead of a vial.
New dispensers make insulin more expensive. Were seeing that again with Afrezza, the only insulin to be delivered as an inhalable powder. One unit of Afrezzas insulin can cost as much as 6 times the price of other rapid-acting insulins.
Here are current retail prices of rapid-acting insulins.
New Product Features Can Come With A High Price Tag
and both contain a long-acting insulin and another non-insulin diabetes medication. Xultophy is a mix of insulin degludec plus liraglutide , and Soliqua is a mix of insulin glargine plus lixisenatide . Average retail prices for Soliqua and Xultophy are more than double the price of cheaper alternatives like Basaglar and Tresiba, which have the same exact kind of insulins.
Fiasp contains insulin aspart, the same insulin in Novolog, but it also has vitamin B3. This added ingredient may speed up insulin absorption, but it doesnt necessarily make Fiasp more effective than Novolog at lowering blood sugar. Interestingly, the retail prices for Fiasp and Novolog are about the same on a per insulin unit basis.
Then theres , an ultra-long-acting insulin that stays active for up to 42 hours. For this unique property, its average retail price is about $624.76 for a carton of 5 KwikPens .
Along with these new formulations, insulin manufacturers have also started offering their insulins at higher concentrations to make them more convenient for people who need more insulin than average. Humulin R, Humalog, and Tresiba all come in higher-concentration versions, and is a higher-concentration version of Lantus. At first glance, their prices may seem high, but they actually go for the same per unit retail price as their lower-concentration counterparts.
Don’t Miss: Can You Lose Weight With Diabetes
Insulin In America: A Right Or A Privilege
Even as a medical student, I was interested in the history of insulin. As an endocrine fellow, I read The Discovery of Insulin by Michael Bliss . It is a book anyone interested in diabetes should read, as life before insulin is difficult to appreciate by todays standard of care, at least in the United States. Amazing stories of what people did to obtain insulin are plentiful, perhaps none more dramatic than Eva Saxls story, with her husband making insulin in Shanghai, China, for the more than 200 Jews who escaped Nazi persecution during World War II .
But in the United States, access to insulin had never been a problem. As a medication required for survival by 10% of those with diabetes, it was always available, although for decades quite crude by todays standards. The insulin patent from the University of Toronto was sold for $1 with the understanding that cheap insulin would become available . Through the years, insulin remained affordable. Even with the introduction of human insulin in 1982 and then insulin analogs in 1996 , the increases in insulin pricing did not seem to be a concern. At least in the United States, the vast majority of patients requiring insulin had access to all of the insulin analogs as they were developed.
Fact Check: Is Joe Biden Responsible For The Rising Cost Of Insulin

Out of roughly 330 million people living in the U.S., about 34 million are living with diabetes.
For individuals with type 1 diabetes, access to insulin is the difference between life and death.
Recently, many Americans have been expressing their outrage on social media at the rising cost of insulin and wonder who is to blame.
Read Also: What Type Of Insulin Can Be Given Iv
The Claim: President Joe Biden Is ‘reversing’ An Executive Order Put Into Place By Donald Trump To Reduce Patient Costs For Insulin And Epinephrine
For years, members of Congress have pressured drug companies and pharmacy benefit managers to bring under control the rising costs of insulin and epinephrine for millions of Americans with diabetes or allergies.
In July 2020, President Donald Trump signed four executive orders aimed at reining in prescription drug costs. One required that federally qualified health centers, which purchase insulin and epinephrine through what’s called the 340B drug program, pass along any savings they receive from discounted drug prices to medically underserved patients.
The rule blocks health centers from receiving future federal grants unless they charge patients no more than their acquisition price for insulin and EpiPens epinephrine auto-injectors plus a small administration fee.
At the time, the U.S. Department of Health and Human Services said the move would increase access to insulin and EpiPens for the 28 million patients who visit community health centers annually, over 6 million of whom are uninsured.
On the campaign trail last year, Trump made repeated claims that, because of the executive orders, he was succeeding in his promise to lower drug prices.
HHS approved the rule affecting community health centers in December, and it was to go into effect Jan. 22.
A user on Facebook claims President Joe Biden is now “reversing” Trump’s executive order. This is NOT a partisan issue and will harm Americans, reads the Jan. 22 post, which has almost 1,000 shares.

