Insulin Takes Sugar Out Of Your Blood And Stores It In Muscles Fat Cells And The Liver For Later Use
Even though it’s helpful for your cells to take in blood sugar for energy, they don’t need immediate access to that sugar all the time. In fact, insulin will take any extra blood sugar that your cells can’t use right away and send it to your muscle cells, fat cells, and liver to be stored for later use. When it’s stored, the original form of sugar, glucose, becomes another form of sugar known as glycogen.
Insulin Takes Sugar Out Of Your Blood And Sends It Into Your Cells To Be Used For Energy
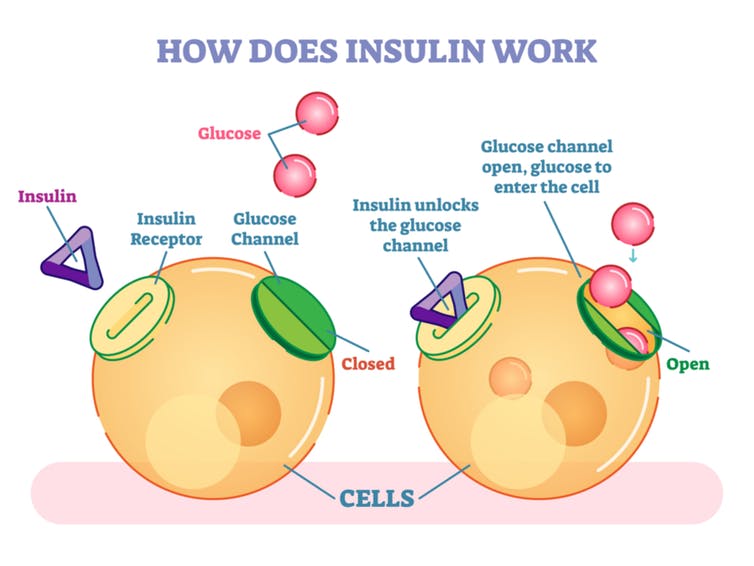
When you eat a meal with carbohydrates , you often get a burst of energy. Well, your cells get energy from sugar too, but how does the sugar get into the cells? That’s where insulin comes in.
Most of the cells in your body contain insulin receptors. Think of an insulin receptor like a lock and the insulin hormone like a key. When the key opens the lock—or when insulin binds to the insulin receptor—the cell opens to let sugar in. By attaching to insulin receptors, insulin helps take sugar out of the blood and sends it into cells to be put to good use. As a result, your blood sugar levels should return to normal.
Types Of Insulin Administration With Needles Pumps Pens And Why Insulin Is So Expensive
Lisa JaffeAmy Hess-Fischl MS, RD, LDN, BC-ADM, CDEJessica Rodriguez CNP
What does insulin do? Help your body turn food into energy, for starters. When you’re diabetic, and you’re either not producing insulin, or your insulin function is off, all sorts of things can go wrong. From needles, to pens, to pumps, to types of insulin, we’re here to empower you with clear answers to all your pressing Qs.
In This Article:
Alvin Powers MD, Mihail Zilbermint MD, and Irl Hirsch MD
What Severe Complications Can Occur Because Of Rationing Or Running Out Of Insulin
Diabetic ketoacidosis is an emergency condition that results if you don’t have enough insulin to regulate your blood sugar. DKA causes your body to break down fat for energy in the absence of insulin. This leads to a dangerous accumulation of acids known as ketones in your blood that can cause your brain to swell and your body to go into shock.
Signs of diabetic ketoacidosis include:
- Thirst or a very dry mouth
- Frequent urination
- High levels of ketones in your urine
- Fatigue
- Nausea, vomiting, or stomach pain
- Difficulty breathing
- A fruity or acetone odor on your breath
- Confusion or acting “drunk” while sober
DKA is so common and can come on so quickly that it is the first sign of Type 1 diabetes in 20% of cases, and the way many type 1 diabetics are first diagnosed with the condition. If you go into diabetic ketoacidosis, don’t try to hide it or make light of it. Treat it as the emergency it is and get to a hospital as soon as possible to recover. “I’ve had people tell me they’re tired of taking insulin, or that they’re rationing it due to cost. In type 1 diabetes, that’s all it takes to end up in a life-threatening situation,” says Dr. Zilbermint.
Another complication facing diabetics who use insulin is the potential for hyperglycemia, also known as “insulin shock,” which involves using too much insulin and causing your blood sugar to drop extremely low. “This can cause coma, seizures, and heart attacks,” says Dr. Powers.
Consume Foods That Have Been Scientifically Proven To Boost Insulin Sensitivity
Scientific research has demonstrated foods like vinegar, lemon, lime, walnuts, almonds, green tea, cinnamon, and turmeric have insulin-sensitizing properties. Including nutrient-dense foods like these in your diet may help improve the body’s sensitivity to insulin and ability to store consumed carbohydrates within muscle glycogen stores instead of as fat. That’s why I included all these kinds of foods inside the Ultra Lean and Muscle Building Cookbooks. If you haven’t checked these cookbooks out already, you’re missing out on over 200+ mouth-watering diabetic friendly recipe ideas that will help you get you in shape without giving up the foods you love.
What Are Alternative Medications For People With Diabetes That Arent Insulin
- Metformin – a pill that stops sugar production in the liver
- Glitazones – pills that remove sugar from the bloodstream
- Sufonylureas and glinides – pills that increase the release of insulin from your pancreas
- Starch blockers – pills that slow starch absorption
- Incretin therapies and amvlin analogs – pills and injections that reduce sugar production in the liver and slow food absorption. Types of the former include DPP4 inhibitors and GLP1 analogs .
- SGLT2 inhibitors – pills that are taken before meals that prevent the reabsorption of glucose
Insulin Sensitivity: What It Is And 4 Ways To Improve It Without Medication
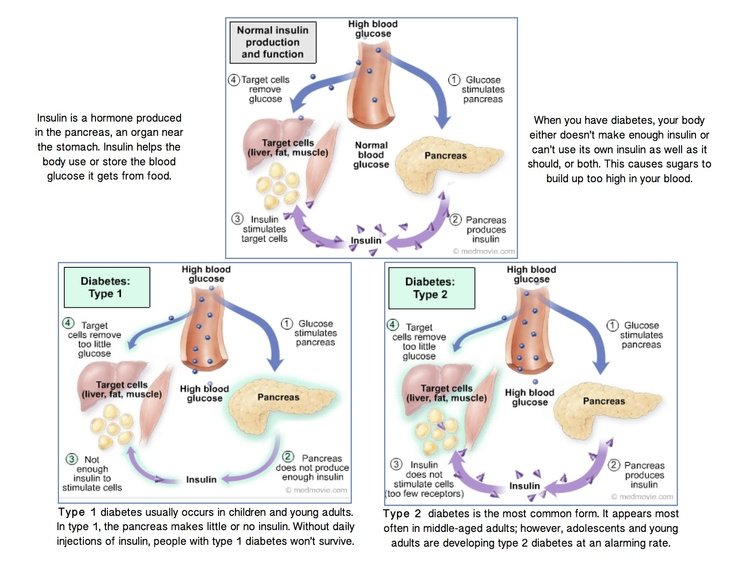
Insulin is an essential hormone produced in the pancreas that regulates blood sugar levels. It effectively helps convert sugar from your blood into your cells as stored glucose . When the body’s cells are insulin resistant, they are unable to use insulin efficiently. This in turn results in elevated blood sugar, above a healthy target range . If the pancreas detects elevated blood sugar, this triggers the production of more insulin to overcome the resistance and lower blood sugar back to an in range level.
Insulin Resistance
Over time, the process of over producing insulin can deplete the pancreas of insulin-producing cells, which is common in people living with type 2 diabetes. Moreover, prolonged and unregulated high blood sugar can damage nerves and organs. Individuals are most at risk of insulin resistance if they already have prediabetes, or a family history of type 2 diabetes, as well as if you are overweight or obese. If you have insulin resistance, you have low insulin sensitivity. Conversely, if you are sensitive to insulin, you have low insulin resistance.
Insulin Sensitivity
Looking to enhance your insulin sensitivity is a smart and healthy decision regardless of whether you are already living with diabetes, or not. Being insulin sensitive ensures that your body properly utilizes food and converts the correct amount of glucose for energy into the bloodstream in the most efficient way possible.
How do I improve insulin sensitivity ?
1. Eat the right foods
Regulation And Mechanisms Of Insulin Secretion At The Cellular Level
Synthesis and secretion of insulin is regulated by both nutrient and non-nutrient secretagogues, in the context of environmental stimuli and the interplay of other hormones. Nutrient secretagogues such as glucose appear to trigger insulin secretion from the ? cell by increasing intracellular ATP and closing of K+-ATP channels as outlined above. Generation of cyclic AMP and other cellular energy intermediates is also augmented, further enhancing insulin release. Glucose does not require insulin action to enter the ? cell . Non-nutrient secretagogues may act via neural stimuli such as cholinergic and adrenergic pathways, or through peptide hormones and cationic amino acids.
Neural Stimuli
1. Cholinergic Transmission
It has been well recognised that vagus nerve stimulation results in pancreatic insulin secretion. This is thought to mediate the so-called “cephalic phase” of insulin secretion, occurring when food is seen, smelled or acutely ingested. Islet cell cholinergic muscarinic receptors activate phospholipase C, with subsequent intracellular events activating protein kinase C, phospholipase A2 and mobilizing intracellular calcium. Insulin secretion by these mechanisms does not occur in the fasting state or if blood glucose levels are low, but may augment the anabolic response to feeding.
2. Adrenergic Pathway
Peptide Hormones
Amino Acids
Schematic presentation of insulin secretory pathways. Adapted from references: &.
Footnotes: Figure Abbreviations
DAG = diacylglycerol
Pharmacological Influences On Insulin Action And Insulin Resistance
A wide range of pharmacological agents have been associated with impaired glucose tolerance. Antihypertensive agents such as diuretics and ?-blockers, corticosteroids, oral contraceptives, nicotinic acid and antipsychotic agents have been reported to impair glucose tolerance, as have the anti-retroviral protease inhibitors used to treat human immunodeficiency virus infection. The mechanisms vary; ?-blockers impair insulin secretion from the pancreas by blockade of ?-adrenoceptors, thiazide diuretics are thought to act by depleting potassium levels, corticosteroids and oral contraceptives have counter-regulatory hormonal activity, and the HIV-1 protease inhibitors result in partial lipodystrophy with loss of peripheral subcutaneous fat and accumulation of truncal adipose tissue leading to insulin resistance.
Foods That Can Produce Insulin Naturally N Body To Fight Diabetes
These days diabetes is a lifestyle disease and once it is dictated in someone, then there is the only chance that it can be controlled. Hardly you have heard that someone actually got cured of diabetes. So, let’s not put anyone in the confusion that, this article is not written for the purpose of curing diabetes, rather it is written to make you aware of the issues and you can have control over your insulin so that everything is in control.
What is Insulin?
Insulin is a hormone made by the pancreas that allows your body to use sugar from carbohydrates in the food that you eat for energy or to store glucose for future use. Insulin helps keeps your blood sugar level from getting too high or too low .
Rose of Pancreas
We hardly think of the pancreas as an important endocrine organ unless it starts to create a problem. The pancreas has two important roles to play; Make insulin for blood sugar control. Create enzymes for the metabolism of fats and proteins.
Malfunction of the pancreas could result in a variety of problems – the most common being diabetes. Fortunately, nature has given us some foods that boost the beta cells of the pancreas to produce insulin and help alleviate diabetes, of course, coupled with the right lifestyle changes.
Foods Help Growing Insulin
1. Red Cabbage
Cabbage, especially red, is a boon for cancer and diabetes patients. The natural red pigments of red cabbage, betalains, helps lower blood sugar levels and boosts insulin production.
4. Fenugreek Seeds
Sites Of Insulin Action And Manifestations Of Insulin Resistance
The effects of insulin, insulin deficiency and insulin resistance vary according to the physiological function of the tissues and organs concerned, and their dependence on insulin for metabolic processes. Those tissues defined as insulin dependent, based on intracellular glucose transport, are principally adipose tissue and muscle. However, insulin’s actions are pleotropic and widespread, as are the manifestations of insulin resistance and the associated compensatory hyperinsulinaemia.
Insulin Resistance: How To Recognize The Symptoms And Reverse It
Megan N. Freeland, PharmD, RPh
Your body naturally produces the hormone, insulin, to help keep your blood sugar at healthy levels, but sometimes your body doesn’t respond to insulin the way it should. When this happens, it’s called insulin resistance. Here, we’ll discuss what insulin resistance is, how it can cause complications like type 2 diabetes, and what you can do to prevent it.
The Primary Hormones That Are Produced By The Pancreas Include:

- Insulin – this hormone works by allowing the body’s cells to absorb glucose from the bloodstream and use it as energy. This in turn helps to reduce high blood sugar levels.
- Gastrin – gastrin hormone stimulates specific cells in the stomach that aids in digestion.
- Glucagon – this hormone helps insulin to maintain a normal blood sugar level by stimulating the cells to release glucose when it is too low.
- Vasoactive intestinal peptide – vasoactive intestinal peptide helps to control absorption and secretion of water from the intestines.
- Somatostatin – in case other hormones such as glucagon and insulin are too high, the hormone somatostatin will be released to help maintain blood sugar.
What New Research Is Being Conducted On Insulin Resistance
Insulin resistance has gained awareness and significance, in its own right, as a contributor to the metabolic syndrome. Timely intervention can delay the onset of overt type 2 diabetes. Future studies must assess longer intervals than existing research to determine the duration for treatment to prevent the development of type 2 diabetes and related complications.
Lifestyle changes are clearly important to delay the development of type 2 diabetes in individuals with insulin resistance. Lifestyle changes are the primary recommendation for prevention of diabetes in high-risk individuals. Metformin is the only drug recommended by guidelines for patients at highest risk. Education about these changes must be directed to all groups at risk for type 2 diabetes. Childhood obesity is epidemic and on the rise in developed countries. Changes must be made in homes and school cafeterias to ensure healthier nutrition.
How Do You Choose The Right Syringe For Injecting Insulin
Just as there are different sizes of syringes for administering insulin, there are also varying sizes of insulin needles. Shorter needles usually mean less sting when injecting. The downside is that the shallower the injection is, the longer it takes for the insulin to work. Your doctor will help you find the balance that’s best for you.
What Are The Drawbacks To Insulin Treatment For Diabetes
The biggest issue with insulin right now is unaffordability. “A box of rapid-acting insulin can cost $400 without insurance. As so many people continue to lose their health coverage, it’s becoming an enormous problem,” Dr. Zilbermint says.
Consistently rising costs have led some patients to ration their insulin, which can be dangerous and even deadly. The cost of testing strips is also an issue, and both have led to a black market in testing strips and insulin. “It’s illegal,” says Dr. Zilbermint, “but it’s happening.”
Add These Wonder Foods Which Can Boost Insulin Secretion
Flax seeds are believed to be good for health as they are rich source of antioxidants, But flaxseeds are proven to be more good for type -1 diabetics , as the clinical trial performed by National Centre for Biotechnology Information – USA reveals that flax seeds are good at increasing production of insulin naturally. apart from flax seeds , curcumin , honey and stevia are also known to repair beta cells of pancreas and help in insulin production naturally.
Consume powder of fenugreek seeds soaked in hot water to reduce your fasting blood sugar levels, tri glycerides and vldl-c cholestrol , results are amazing you may see below
http://www.ncbi.nlm.nih.gov/pubmed/19839001
Drink Plenty of Fluids is a simple tip to boost insulin productionDrinking plenty of fluids is another factor that can enhance the functioning of pancreas. Due to consumption of fatty and sugar rich foods, pancreas gets soaked in acidic secretions and it interferes with usual state of its functions. Pancreas requires a moderately alkaline environment to be healthy. Being hydrated and taking more liquids with wash off the acidic secretions enhancing the production of insulin and digestive juices from pancreas.
Add Apple Cider Vinegar to your Daily Routine
What Else Can I Do To Control My Blood Glucose Levels
Food, sleep, and exercise are all of vital importance for regulating your blood sugar when you have diabetes.
Where Can I Find Help Acquiring Or Paying For Insulin
The ADA has a dedicated page for helping people who need insulin get it, regardless of finances: http://www.insulinhelp.org.
JRDF has a page with a variety of links to organizations who also supply insulin assistance: https://www.jdrf.org/t1d-resources/living-with-t1d/insurance/help-with-prescription-costs/
Prioritize The Essential Fatty Acids Especially Omega
The human body can synthesize most of its fat needs from the diet. However, there are two essential fatty acids, known as Omega 6 and Omega 3 which cannot be produced in the body and must be consumed from food. Both of these fats can be found in plant and animal foods.
Consuming a healthy balance of omega-6s and omega-3s is very important for human health.
However, in today’s modern society many populations at risk of obesity and diabetes have an imbalance in their consumption of omega 3s and 6s, whereby too much omega 6 is consumed at the expense of omega 3.
While both of these fatty acids are essential for good health, the stark imbalance is pro-inflammatory and detrimental to insulin sensitivity. The imbalance is a result of the world’s growing food intake, particularly increased consumption of processed food cooked in processed polyunsaturated fats like sunflower oil.
The first line of defence in rectifying this imbalance involves eating fewer calories and improving energy balance with physical activity. The next step is to increase omega 3 consumption from cold water fatty fish or use of high-quality Omega 3 food supplements.
Ideally, 340-453g of cold-water, fatty fish such as salmon, sardines, and mackerel each week, if personal taste allows for it. Otherwise a good quality fish oil supplement.
Clinical Syndromes Associated With Insulin Resistance
Type 2 diabetes and the Metabolic Syndrome would be the most common clinical syndromes associated with insulin resistance. Others include hypertension, PCOS, non-alcoholic fatty liver disease, certain forms of cancer and OSA, which some authors consider a component of the metabolic syndrome per se. There are also relatively common conditions where insulin resistance is a secondary phenomenon; these include acute illness, hepatic cirrhosis, renal failure, pregnancy, hyperthyroidism, Cushing’s disease and Cushing’s syndrome as well as acromegaly and phaeochromocytoma which are less common. In many of these, the insulin resistance is due to increased production of counter-regulatory hormones.
However there are also a large number of generally rare disorders where insulin resistance is a major clinical feature., Though individually rare, these conditions may provide insight into the mechanisms of insulin resistance in other settings. Typically they are characterised by disturbances in organ systems where insulin action plays a critical role.
How To Increase Insulin Production In Body Naturally
If you are a type 1 / type-2 diabetic whose morning starts with where shall I inject insulin today and you are one amongst many type 1 /type-2 diabetics who struggles to manage insulin levels and are frustrated of the costs and the pain of injecting insulin everyday then you must know there are methods to produce insulin in your body naturally by making great food choices, exercise regularly and taking right vitamin supplements, Lets explore !! Even if you can reduce one shot of insulin it feels great ,,, ?
Insulin is a hormone that is mainly responsible for glucose regulation. It is produced by the beta cells of pancreas, an organ that is located in the abdomen. Insulin allows the glucose uptake by body cells so that it can be utilized as fuel by the body tissues.Our body needs an optimum level of insulin to maintain the normal glucose balance. Either reduction or an increase in insulin will have deleterious effects on body. In cases where insulin starts falling, the body fails to consume sugar as body fuel. Hence, it is crucial to have a recommended insulin level for healthy body functions. A decrease in insulin results in type 1 diabetes.
Production Of Hormones To Control Blood Sugar Levels
A small proportion of the pancreas is made up of other types of cells called islets of Langerhans. These cells sit in tiny groups, like small islands, scattered throughout the tissue of the pancreas. The islets of Langerhans contain alpha cells which secrete glucagon and beta cells which secrete insulin.
Insulin and glucagon are hormones that work to regulate the level of sugar in the body to keep it within a healthy range. Unlike the acinar cells, the islets of Langerhans do not have ducts and secrete insulin and glucagon directly into the bloodstream.
Depending on what you’ve eaten, how much exercise your muscles are doing, and how active your body cells are, the amount of glucose in your bloodstream and cells varies. These 2 hormones have the job of keeping tight control of the amount of glucose in your blood so that it doesn’t rise or fall outside of healthy limits.
Factors Influencing Insulin Biosynthesis And Release
Insulin secretion may be influenced by alterations in synthesis at the level of gene transcription, translation, and post-translational modification in the Golgi as well as by factors influencing insulin release from secretory granules. Longer-term modification may occur via influences on ? cell mass and differentiation. Given insulin’s pivotal role in glucose utilisation and metabolism, it is not surprising that glucose has multiple influences on insulin biosynthesis and secretion. However, other factors such as amino acids, fatty acids, acetylcholine, pituitary adenylate cyclase-activating polypeptide , glucose-dependent insulinotropic polypeptide , glucagon-like peptide-1 , and several other agonists, together in combination, also influence these processes.
Common Conditions Associated With Insulin Resistance
Type 2 Diabetes
Following pioneering work by Bornstein and the Nobel Prize-winning work of Yalow and Berson, the first insulin assays became widely available in the late 1960s; it was subsequently confirmed that diabetic patients with so-called or maturity onset or type 2 diabetes had normal or increased plasma insulin levels. Insulin resistance was reported to be a characteristic feature of T2DM in the early 1970s. A progressive inability of the ? cells to compensate for the prevailing insulin resistance by sufficient hyperinsulinaemia, heralds the clinical onset of this disorder. While twin studies and linkage analyses are consistent with a strong genetic component in the development of type 2 diabetes, several decades of research have failed to identify a predominant genetic abnormality in the majority of cases. The aetiology of T2DM is thought to be polygenic, with environmental factors being superimposed upon this basic predisposition.
Insulin resistance typically predates the development of diabetes and is commonly found in unaffected first-degree relatives. The morbidity of the disorder relates both to the severity of hyperglycaemia and the metabolic consequences of insulin resistance itself. The primary defects in insulin action appear to be in muscle cells and adipocytes, with impaired GLUT 4 translocation resulting in impaired insulin-mediated glucose transport.
Metabolic Syndrome
-
Abdominal obesity
Men <40 mg/dL
Women <50 mg/dL
Dyslipidaemia
Hypertension
PCOS
OSA
Consider Supplementing With Magnesium And Vitamin D
Magnesium and vitamin D have been shown to improve the body’s sensitivity to insulin. Low magnesium levels are common in people with Type 1 and Type 2 diabetes.
Magnesium is an essential dietary mineral and the second most prevalent electrolyte in the body besides sodium. Magnesium has a strong relationship with insulin and thus plays an important role in carbohydrate metabolism 1,2.
Research has shown that subjects who supplemented with oral magnesium improved their fasting blood glucose levels and increased their insulin sensitivity.3
The standard dose for magnesium supplementation is 200-400mg.4
Vitamin D is a fat-soluble nutrient essential for human survival.
Vitamin D is known to aid in improving insulin receptor function, prevent islet cell death, as well as improve beta cell function.
Research in both type 1 and type 2 diabetes have shown positive results in that supplementing with vitamin D has the potential to lower haemoglobin A1c compared to baseline.5,6 Much of this may in part be due to improving insulin resistance.
Individuals with diabetes should get a 25D blood test to assess their current vitamin D status. The Vitamin D Council recommends a blood level between 50–80 ng/mL year round.
If needed, 1,000-2,000 IU of Vitamin D per day is more than adequate. 7
Both magnesium and vitamin D may be consumed via supplements. However, they can also be obtained from food.

