Functions Of Insulin In The Body: Good Guy Or Bad Guy
Insulin is perhaps the most important compound circulating in our bodies. It is involved in more than 60 key biological processes. Impairments in insulin function affect many facets of health and well-being and, if left uncorrected, are ultimately fatal. Despite its paramount importance, the functions of insulin in the body are widely misunderstood.
Insulin is an anabolic hormone, meaning it acts to promote synthesis and building, as opposed to catabolic hormones that break down and deconstruct bodily tissues and compounds. Given its vital importance, it is curious that insulin is sometimes portrayed as the bad guy. Consider, for instance, how we cast insulin as the villain responsible for the development of adverse health conditions: type 1 and type 2 diabetes, metabolic syndrome, polycystic ovary syndrome, and even certain types of cancer.
In this article, we will explore the basic functions of insulin in the body to gain a better appreciation for all it does as well as a clearer understanding of how to keep this hormone functioning in balance and at its optimal capacity.
Maintains Amino Acid Uptake
Another function or role of insulin is that it compels cells the absorb of circulating amino acids. A decrease in insulin levels inhibits this absorption. Individuals with low insulin levels have high blood amino acids. Introducing insulin in their systems brings down amino acid levels in the blood to normal values. In other words, insulin promotes the synthesis or metabolism of protein from circulating amino acids.
How Is Insulin Resistance Diagnosed
Although insulin resistance doesnt usually have symptoms, your doctor may recommend testing your blood sugar if you have risk factors for this condition, such as obesity, a sedentary lifestyle, or high blood pressure.
Test
Read Also: Oatmeal Carbs Diabetes
Favorite Resource For Diabetes Education
If insulin resistance has led you to be diagnosed with diabetes or you want to be educated if that day comes, enroll in a program led by Joslin Diabetes Center experts. The 12-week Why Wait program is designed to help you meet your weight goals, which could improve your bodys sensitivity to insulin.
Insulin Basics: How Insulin Helps Control Blood Glucose Levels
Insulin and glucagon are hormones secreted by islet cells within the pancreas. They are both secreted in response to blood sugar levels, but in opposite fashion!
Insulin is normally secreted by the beta cells of the pancreas. The stimulus for insulin secretion is a HIGH blood glucose…it’s as simple as that! Although there is always a low level of insulin secreted by the pancreas, the amount secreted into the blood increases as the blood glucose rises. Similarly, as blood glucose falls, the amount of insulin secreted by the pancreatic islets goes down.
As can be seen in the picture, insulin has an effect on a number of cells, including muscle, red blood cells, and fat cells. In response to insulin, these cells absorb glucose out of the blood, having the net effect of lowering the high blood glucose levels into the normal range.
Glucagon is secreted by the alpha cells of the pancreatic islets in much the same manner as insulin…except in the opposite direction. If blood glucose is high, then no glucagon is secreted.
When blood glucose goes LOW, however, more and more glucagon is secreted. Like insulin, glucagon has an effect on many cells of the body, but most notably the liver.
Also Check: Insulin Gpcr
Where Does The Insulin Come From
A1) Insulin is a hormone that is made by beta cells in our pancreas. These beta cells manufacture and release the insulin into our blood so that it may circulate and allow glucose to enter and fuel the cell. As such, when insulin enters the cells the remaining supply of glucose in our blood decreases.
Role Of Insulin In The Regulation Of Liver Function
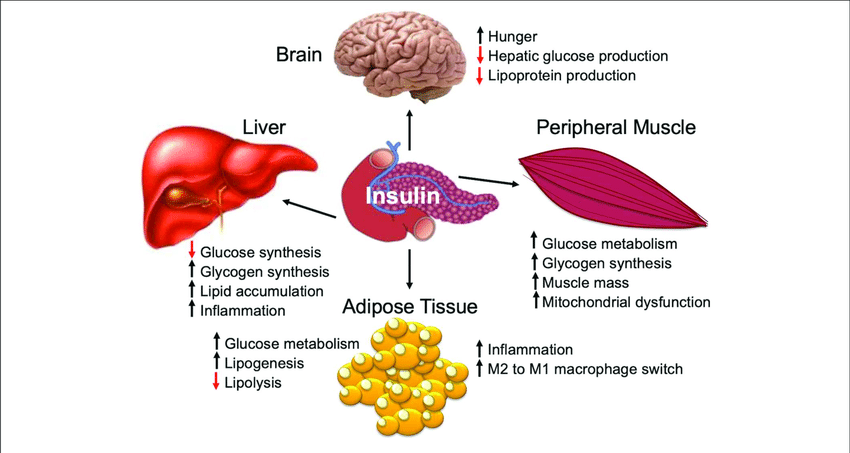
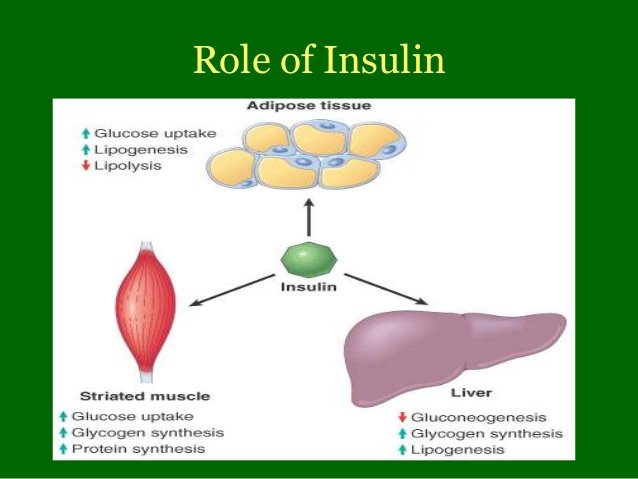
Major physiological roles of insulin in the liver, adipose tissue, and skeletal muscles. After production and release from pancreatic β cells, insulin enters the bloodstream to ultimately reach all other organs. In the liver, insulin helps promote the transport of glucose from the blood into hepatocytes, where it is further converted to glycogen, fatty acids, and triglycerides. In the skeletal muscles, insulin facilitates the uptake of glucose and amino acids from the bloodstream. The amino acids are subsequently used for functional protein synthesis, while glucose is mostly utilized in glycolysis to produce energy in the form of ATP. Glucose may also be converted to the glycogen that is mostly stored as energy for times of deficit. Insulin stimulates adipose tissue uptake of fatty acids, which are later converted into triglycerides and used as long-term energy stores. It is important to note that each of the steps/processes regulated by insulin in the figure are reversible. Whenever insulin stimulates the processes, they are generally irreversible.
Don’t Miss: Which Hormones Are Produced By The Pancreatic Islets That Regulate Blood Glucose Concentrations
Is Insulin Still Made From Pigs
Animal insulin is derived from cows and pigs. Until the 1980s, animal insulin was the only treatment for insulin dependent diabetes. These days the use of animal insulin has largely been replaced by human insulin and human analogue insulin, however, animal insulin is still available on prescription.
What Happens If I Have Too Much Insulin
If a person accidentally injects more insulin than required, e.g. because they expend more energy or eat less food than they anticipated, cells will take in too much glucose from the blood. This leads to abnormally low blood glucose levels . The body reacts to hypoglycaemia by releasing stored glucose from the liver in an attempt to bring the levels back to normal. Low glucose levels in the blood can make a person feel ill.
The body mounts an initial ‘fight back’ response to hypoglycaemia through a specialised set of of nerves called the sympathetic nervous system. This causes palpitations, sweating, hunger, anxiety, tremor and pale complexion that usually warn the person about the low blood glucose level so this can be treated. However, if the initial blood glucose level is too low or if it is not treated promptly and continues to drop, the brain will be affected too because it depends almost entirely on glucose as a source of energy to function properly. This can cause dizziness, confusion, fits and even coma in severe cases.
Some drugs used for people with type 2 diabetes, including sulphonylureas and meglitinides , can also stimulate insulin production within the body and can also cause hypoglycaemia. The body responds in the same way as if excess insulin has been given by injection.
Don’t Miss: Insulin Inhibits Glucagon
Regulation Of Insulin Secretion
The physiology of insulin-producing cells is fundamental to understanding the regulation of insulin secretion. Insulin is a peptide hormone secreted by β cells of the pancreas. The human pancreas contains one to two million pancreatic islets housing different endocrine cells, primarily insulin-secreting β cells, glucagon-producing α cells, and somatostatin-secreting δ cells . Although islets compose only 1â2% of the human pancreas, they receive up to 10% of the total pancreatic blood supplies . Generally, insulin is released after ingesting glucose in a process named glucose-induced insulin stimulation. This process requires both the intracellular uptake and metabolic degradation of ingested glucose . In human β cells, glucose transporter 1 and GLUT3 are the prominent glucose transporters, whereas GLUT2 has been reported as a major glucose transporter in rodent . This difference could be attributed to the differences in Km values of different isoforms of glucose transporters .
The phosphorylation of glucose by the enzyme glucokinase is the first step in glucose metabolism. Glucose phosphorylation by GCK is related to insulin secretion therefore, GCK gene dysfunction or aberration leads to decreased glucose-mediated insulin release and glucose intolerance or diabetes . A major understanding of insulin secretion is derived from the research using rodent models, whereas few studies have been described in humans .
What Happens To The Body Without Insulin
Without insulin, your body will break down its own fat and muscle, resulting in weight loss. This can lead to a serious short-term condition called diabetic ketoacidosis. This is when the bloodstream becomes acidic, you develop dangerous levels of ketones in your blood stream and become severely dehydrated.
Read Also: What Is A Normal Dose Of Metformin
Insulin And Its Structure:
Insulin is a peptide hormone, composed of long chains of proteins and amino acids, that performs numerous crucial functions in the human system, being chiefly involved in glucose metabolism. It was the first peptide hormone to be discovered in the year 1921 by three renowned medical researchers Canadian physician Sir Frederick Grant Banting, American-Canadian scientist Charles Herbert Best and Scottish biochemist J.J.R. Macleod.
Later on, in the year 1951, famed British biochemist Frederick Sanger determined the precise amino acid arrangement of insulin, with another prominent British chemist Dorothy Hodgkin decoding its elaborate chemical crystal structure. The human insulin protein is made up of 51 amino acids, with a molecular mass of 5808 Da . It occurs in the form of a heterodimer i.e. a protein composed of two chains A-chain and B-chain joined by disulfide bonds.
Insulins Action On The Digestive System
When a person eats a meal, food is allowed to travel to the stomach and the small intestines. There the food undergoes a breakdown into small nutrient particles that are then absorbed into the blood. In response to this absorption of carbohydrate nutrients, the pancreas secretes insulin in order to make use of the glucose for cellular metabolism. The pancreas is considered part of the digestive system as well as the endocrine system.
Insulin allows the fat cells, muscle cells, and liver cells to keep glucose in storage until it is later needed for cellular fuel. At the same time, the liver makes less glucose and instead stores it as glycogen. This allows the blood sugars to remain stable. Between meals, the liver breaks down its glycogen stores so that there will always be enough glucose in the bloodstream.
Also Check: What Happens If You Stop Taking Diabetes Medication
How To Enhance Insulin Function
Aside from the nutritional strategy of minimizing large spikes in blood glucose, the most effective way to enhance insulin function is to stay physically active.
It makes sense that insulin is an important factor in making sure the body is properly fueled for physical activity. Insulin helps deliver glucose from the blood into the muscle cell. Once in the muscle, glucose is metabolized to produce energy to support physical exertion. Insulin also stores excess glucose as glycogen so that it can be used for energy at a later time.
Dietary protein and amino acids can also stimulate insulin release. Consuming a balance of carbohydrate and protein, such as supplemental amino acids, during exercise has been proven to stimulate more insulin than carbohydrate alone, resulting in faster delivery of glucose to working muscles.
Insulin is also needed to optimize recovery of muscles from a hard workout. Immediately after exercise, the muscle is primed to replenish fuel stores like glycogen and to rebuild and repair muscle proteins. During this period, insulin accelerates the rate at which glycogen and protein synthesis proceeds, up to 2 to 3 times the normal rate as long as carbohydrate and protein are ingested and made available.
Evolution And Species Distribution
Insulin may have originated more than a billion years ago. The molecular origins of insulin go at least as far back as the simplest unicellular eukaryotes. Apart from animals, insulin-like proteins are also known to exist in the Fungi and Protista kingdoms.
Insulin is produced by beta cells of the pancreatic islets in most vertebrates and by the Brockmann body in some teleost fish.Cone snailsConus geographus and Conus tulipa, venomous sea snails that hunt small fish, use modified forms of insulin in their venom cocktails. The insulin toxin, closer in structure to fishes’ than to snails’ native insulin, slows down the prey fishes by lowering their blood glucose levels.
Don’t Miss: Can Diabetic Eat Cheese
What Else Can I Do To Control My Blood Glucose Levels
Food, sleep, and exercise are all of vital importance for regulating your blood sugar when you have diabetes.
What Severe Complications Can Occur Because Of Rationing Or Running Out Of Insulin
Diabetic ketoacidosis is an emergency condition that results if you dont have enough insulin to regulate your blood sugar. DKA causes your body to break down fat for energy in the absence of insulin. This leads to a dangerous accumulation of acids known as ketones in your blood that can cause your brain to swell and your body to go into shock.
Signs of diabetic ketoacidosis include:
- Thirst or a very dry mouth
- Frequent urination
- High levels of ketones in your urine
- Fatigue
- Nausea, vomiting, or stomach pain
- Difficulty breathing
- A fruity or acetone odor on your breath
- Confusion or acting drunk while sober
DKA is so common and can come on so quickly that it is the first sign of Type 1 diabetes in 20% of cases, and the way many type 1 diabetics are first diagnosed with the condition. If you go into diabetic ketoacidosis, dont try to hide it or make light of it. Treat it as the emergency it is and get to a hospital as soon as possible to recover. Ive had people tell me theyre tired of taking insulin, or that theyre rationing it due to cost. In type 1 diabetes, thats all it takes to end up in a life-threatening situation, says Dr. Zilbermint.
Another complication facing diabetics who use insulin is the potential for hyperglycemia, also known as insulin shock, which involves using too much insulin and causing your blood sugar to drop extremely low. This can cause coma, seizures, and heart attacks, says Dr. Powers.
Also Check: Which Pancreatic Cells Release Insulin And Glucagon
What Will Insulin Be Like In The Future
Pharmaceutical companies are working on very long-acting versions of insulin that could last for a week. There is also an ultra-fast version of insulin under development that will act in less than 15 minutes.
Another group of researchers is looking at glucose responsive insulin , which would react to the needs of your body in real time. It would have nanosensors bound to the insulin so that when insulin is needed, it releases, and when it isnt, it stops, according to Dr. Hirsch.
How Should I Store My Insulin
- Keep current insulin at room temperature to help alleviate injection discomfort.
- Insulin can usually be stored at room temperature for about a month. Once in use, insulin pens should be stored at room temperature. Expiration dates of insulin pens can vary depending upon the type of insulin. For disposable pens, you should discard the entire device when empty or when you reach the expiration date.
- Store extra insulin in the refrigerator.
- Dont expose insulin to excessive cold or heat.
You May Like: How Many Points Does Metformin Lower Blood Sugar
Insulin Function In Human Body
Insulin is a hormonal agent produced by the pancreas that has a number of important functions in the body, particularly in the control of blood sugar levels and avoiding hyperglycemia. It also has a result on several other areas of the body, consisting of the synthesis of lipids and regulation of enzymatic activity.
Factors Influencing Insulin Biosynthesis And Release
Insulin secretion may be influenced by alterations in synthesis at the level of gene transcription, translation, and post-translational modification in the Golgi as well as by factors influencing insulin release from secretory granules. Longer-term modification may occur via influences on cell mass and differentiation. Given insulins pivotal role in glucose utilisation and metabolism, it is not surprising that glucose has multiple influences on insulin biosynthesis and secretion. However, other factors such as amino acids, fatty acids, acetylcholine, pituitary adenylate cyclase-activating polypeptide , glucose-dependent insulinotropic polypeptide , glucagon-like peptide-1 , and several other agonists, together in combination, also influence these processes.
Also Check: Can You Be Born With Type 2 Diabetes
Recommended Reading: What Is A Normal A1c For A Non Diabetic
Regulation Of Brain Functions
Another role of insulin is that it regulates brain function. Insulin in the brain contributes to the regulation of cognition and memory while providing neurotropic, neuromodulatory, and neuroprotective effects. Irregular levels and activities of insulin may result not only in type 1 diabetes, as well as insulin resistance and type 2 diabetes but also in the development of memory and cognitive problems. Take note that there is a close association between type 2 diabetes and Alzheimerâs disease. It is also important to note that because the brain is strictly dependent on glucose while other organs can use fats and proteins as their energy source, the glucose-regulating effects of insulin is essential in maintaining healthy brain functions.
FURTHER READINGS AND REFERENCES
Insulin Resistance In The Bipoc Community
according to a March 2019 study in Diabetes and Vascular Disease Research.according to a systematic review and meta-analysis in Diabetes Care.
- 5 percent of non-Hispanic whites
- 2 percent of Asian Americans
- 7 percent of non-Hispanic blacks
- 5 percent of Hispanics
- 7 percent of American Indians/Alaskan Natives
More on Health Disparities Affecting BIPOC Individuals
Also Check: How Many Carbs Should A Diabetic Have In One Day

