Why Are Diabetics Prone To Foot Ulcers And Other Chronic Wounds
Diabetic patients are more prone to developing chronic wounds for a few reasons. Two of the most influencing factors are nerve damage and blood circulation issues that are common among diabetic patients.
Nerve damage, or neuropathy, tends to occur in patients who have a longer history with diabetes because elevated blood glucose levels damage nerves over time. Neuropathy causes patients to experience reduced, or lack of, sensation in the areas affected.
Many patients can sustain trauma or develop an infection without realizing it because theyre unable to feel pain in the area. Further, neuropathy commonly affects the feet, so a wound on the bottom of the foot can escalate quickly because the patient cannot feel or see the wound easily.
Blood circulation issues also can increase the risk for developing chronic wounds, as well as making the wounds more prone to infection. High blood glucose levels cause the narrowing of blood vessels, which constricts blood supply, Estocado said. Adequate blood supply is essential to normal wound healing. The secondary effect of impaired blood supply is a decrease in white blood cells, which are responsible for fighting infection and maintaining a strong immune system.
You May Like: Normal A1c For Non Diabetics
Flaxseed Repairs The Skin Tissues
These seeds are an excellent home remedy for diabetic foot ulcers. Flax seeds work on one of the root causes of diabetic foot ulcers, vascular damage. These seeds are a rich source of omega-2 fatty acids which is necessary for repairing damaged blood vessels and for keeping the blood vessels flexible and functional. Therefore, by improving vascular health, flax seeds bring about a considerable improvement in diabetic foot wounds.
How Do You Treat A Cut On A Diabetic Foot
As we mentioned before, broken skin on the foot is more likely to become infected because of diabetes. This means that treatment for diabetic cuts or wounds should be almost immediate. So what are some treatments for a cut on a diabetic foot?
The most common treatment for open wounds or ulcers in people with diabetes is using a cleanliness regimen and dressings to promote rapid wound healing and prevent infection. Cleaning the wound/ulcer meticulously with soap and water removes all dead tissue such as slough from the surface making it a less perfect environment for bacterial growth and improves the healing process. A wet dressing can use material from previous incisions which have healed as well as dry non-adherent dressings available over-the-counter at pharmacies, grocery stores, to help maintain a moist environment around the wound/ulcer which can speed up the healing process and prevent infections around the affected area.
Here are some basic steps on how to treat a wound on a diabetic foot:
Don’t Miss: High Glucose Dmem
Treatment Management & Guidelines
Treatment: People with diabetes have more risk of foot ulcers. Foot ulcers are the main reason for leg amputations worldwide. Immediately treating foot ulcers is therefore necessary. Treatment varies from person to person condition and this includes:
Medication: Medicine treatment includes:
- Antibiotics to control infection of sore or wound
- Anticlotting medicines to reduce blood clots and improve blood circulation
- Diabetic control medicines to control diabetes.
- Painkillers to relieve pain due to foot ulcers.
Surgical options: Surgery may include:
Summary:
Foot ulcer treatment includes antibiotics and anti-clotting medicines, and it may require surgeries for increasing blood flow.
Management: Management of foot ulcers consists of providing relief from the ulcer pain or itching and to stop its growth. This includes:
Summary:
Diabetic Foot Ulcer Home Treatment
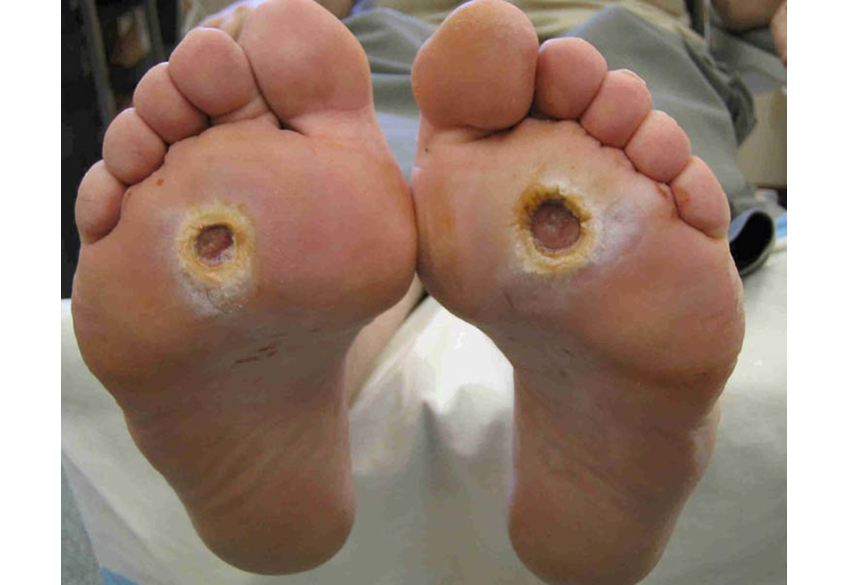
A diabetic foot ulcer is an open wound that happens due to uncontrolled sugar levels in diabetes patients. It is a troublesome condition that hinders a person from carrying on their daily routines. The worst part about diabetic foot ulcers is that person may not even be aware of its growing seriousness due to the damaged sensation of the affected area.
If you suffer from this problem of a diabetic foot ulcer, here is a sigh of relief for you in the name of home treatments or remedies. Yes, there are things that you can try at home to treat diabetic foot ulcers to some extent.
Read Also: Diabetic Medicine Side Effects
What Are A Diabetic Ulcer And Its Symptoms
Diabetic Ulcer is a medical issue mostly occurs in diabetes patients. It is a kind of infection which is dangerous for the individual. Therefore, it needs on time treatment for maintaining good health. It occurs due to the fail in veins for pushing the blood towards the heart, it actually flows back into the legs, eventually causing ulcers. All the arteries in the legs are blocked. In this problem, it shows the following symptoms which help in depicting the ulcer infection.
-
Swelling in wounds
-
Irritation
-
Hard Skin
These symptoms often vary from individual to individual. Although it might get disappear in a few days, some may be non-healing. Therefore, it is important to prevent further complications so better to diagnose it first. Better to visit a doctor and in some cases, your doctor may refer you to a vascular specialist if he is not able to confirm your condition.
What It Means To Have A Diabetic Foot Ulcer
A diabetic foot ulcer is an open sore or wound that forms when skin tissue breaks down and exposes the layers underneath. These ulcers typically occur under the big toes and balls of the feet.
Anyone with diabetes can develop foot ulcers, but some may be at higher risk than others, says Barrett. Those of Native American, African-American or Hispanic descent are at a greater risk for these ulcers. Older men, people who use insulin, and those who have kidney, eye or heart disease related to diabetes are also at a greater risk.
Some common causes of diabetic foot ulcers include:
- Poor circulation
Recommended Reading: What Is A Normal A1c For A Non Diabetic
You May Like: Does Metformin Cause A Rash
Growth Factors For Treating Diabetic Foot Ulcers
What are diabetic foot ulcers?
People who suffer from diabetes mellitus can develop wounds on their feet and ankles. These diabetic foot ulcers can take a long time to heal, and affect quality of life for people with diabetes. In some people, failure of these ulcers to heal can contribute to the need for some level of amputation on the foot. Any treatments that encourage diabetic foot ulcers to heal will be valuable.
What are growth factors?
Growth factors are substances that occur naturally in the body. They promote growth of new cells and healing of wounds. Treatment of diabetic foot ulcers with growth factors may improve the healing of ulcers.
The purpose of this review
This Cochrane review tried to identify the benefits and harms of treating diabetic foot ulcers with growth factors in addition to providing standard care .
Findings of this review
The review authors searched the medical literature up to 3 March 2015, and identified 28 relevant medical trials, with a total of 2365 participants. The trials were performed in ten different countries, generally in out-patient settings. All the trials had low numbers of participants, which makes potential overestimation of benefits and underestimation of harms more likely. Half of the trials were sponsored by the pharmaceutical industry that produces these growth factors.
Shortcomings of the trials included in this review
Ayurvedic Home Remedies For Treating Diabetic Ulcer
Ayurveda is a perfect remedy to treat any kind of health issues. From the ancient time, people are following herbal medicines for having a healthy and happy life. Ayurveda helps in avoiding all health complications and understands the root cause of disease and then manage and treat health problems. We have mentioned the Best Home Remedies to treat Diabetic Ulcer as follows.
Also Check: How Many Carbs Should A Diabetic Have Daily
Wet To Dry Dressing Or Simple Saline
This dressing has a good debriding action and helps in wound bed preparation. Wet-to-dry dressings are described in the literature as a means of mechanical debridement. It is very absorptive as well as adherent and one of the cheapest dressings used throughout the world, but requires frequent dressing change based on wound severity. Dressings should be moistened before removal to minimize any chance of bleeding. A gentle cleanser will minimize wound irritation and discomfort. When treating a granulating or epithelizing wound one should soak the dressing thoroughly with normal saline for five minutes to prevent trauma and heavy bleeding.
What Makes Foot Ulcers So Serious
The soft tissue of the foot isnt like that on other parts of the body, so an infection can get to the muscle and bone very quickly. Infection and poor blood flow can lead to more serious complications, Dr. Scott says.
That infection is what ultimately can lead to amputation. For this reason, you need to see your doctor quickly if you suspect you have a foot ulcer.
Your doctor may order an X-ray, and possibly an MRI, if you have an ulcer that is worsening. This will show whether there is any infection in the bone.
If you do get a foot ulcer, you need to keep your sugars under control and follow up regularly with your doctor.
Its important not to ever let a wound linger without treatment. As time passes, the chances of it healing decrease. Be sure to see your doctor right away. If you dont have a podiatrist, youll need to get one to help you keep tabs on your foot health, Dr. Scott says.
Dont Miss: Can You Live A Long Life With Diabetes
Read Also: Somatostatin And Insulin
Promising Treatments For The Healing Of Diabetic Foot Ulcers
The number of Canadians with #diabetes is rapidly increasing. According to the Canadian Diabetes Association, more than 20 Canadians are diagnosed with the disease every hour of every day.
#Diabetic foot ulcers are the most common chronic complication from diabetes, affecting four to 10 per cent of patients. DFUs can last a year or longer and can happen again in up to 70 per cent of people who have previously been affected. Patients are more likely to develop DFUs if they have had diabetes for a long time, have poorly controlled blood sugar, have foot injuries or infection, are older, or smoke. However, neuropathy, damage to the nerves, which may result in a lack of feeling in the feet, and peripheral artery disease, which reduces the blood flow to the limbs, may be the most significant causes. Because of nerve damage and numbness, an individual with diabetes may not be aware that they have a sore or wound, leading to even minor injuries getting worse or becoming infected. Decreased blood flow caused by peripheral vascular disease may prevent healing once an injury occurs.
When DFUs become infected, the bone or skin can also become infected. This can lead to significant pain and suffering poor quality of life for patients amputation of a leg, foot, or toe increased treatment and hospitalization costs and can even lead to death.
Off-Loading Devices
Compression Therapy
How Diabetic Foot Ulcers Are Treated
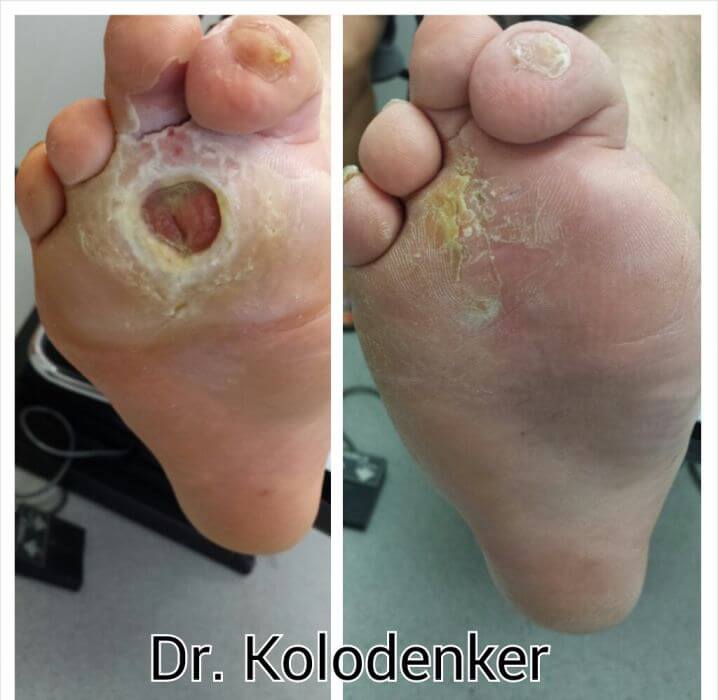
If you do develop a diabetic foot ulcer, your podiatrist will perform debridement of the wound. This means that the doctor will remove the dead skin and tissue from the ulcer to encourage the healing of the tissue. The podiatrist will then apply a dressing to it to prevent an infection. The physician can also perform off-loading to relieve pressure from your foot ulcers, whereby your foot may be placed in a special boot, brace, or cast as your ulcers heal.
Also Check: What Is Your Blood Sugar Supposed To Be
What Are The Clinical Features Of Diabetic Foot Ulcer
A diabetic foot ulcer is a skin sore with full thickness skin loss often preceded by a haemorrhagicsubepidermal blister. The ulcer typically develops within a callosity on a pressure site, with a circular punched out appearance. It is often painless, leading to a delay in presentation to a health professional. Tissue around the ulcer may become black, and gangrene may develop. Pedal pulses may be absent and reduced sensation can be demonstrated.
Diabetic foot ulcer
New Treatment Using Pure Oxygen Therapy That Is Applied At Home Appears Effective In Speeding Up Healing Of Diabetic
with Robert G. Frykberg, DPM, David Armstrong, DPM, MD, PhD, and Mike Griffiths, DProf
If you have diabetes, developing a foot ulcer can be seriousdeadly serious. These open sores occur in about 15 percent of those with diabetes, and most often appear on the bottom of the foot. About half of all people who experience a foot ulcer will land in the hospital due to either an infection or another complication related to the foot ulcer.1
Of course, this open, slow-to-heal wound is likely to restrict your mobility and make life pretty unbearable and depressing, especially if, as is common, an infection sets in, or is worsened by poor circulation. And, the standard treatments, ranging from compression stockings to are not sufficiently effective.
Now, there may be a home-based method of oxygen therapy that is reported to helpboth to heal the ulcers faster than usual care and to help keep them from recurring.2.
“This approach delivers pure oxygen directly to the surface of the wound,” says Robert G. Frykberg, DPM, the study’s lead author and an adjunct professor at Midwestern University in Glendale, Arizona. The best aspect of this new treatment is that it can be done by the patient at home, which is a huge bonus, he tells EndocrineWeb.
Recommended Reading: Bananas For Type 2 Diabetes
What Are The Diabetic Feet Causes
Diabetes negatively affects the healing process of your body. The blood vessels get damaged and oxygen supply becomes insufficient, leading to neuropathy. Neuropathy is basically the loss of sensation in a particular body part. Therefore, diabetic feet lose sensation and the skin around start to break, leading to painful sores. The wounds create constant pressure, forming severe ulcers.
Who Gets Diabetic Foot Ulcer
Diabetic foot ulcer has an annual incidence of 26% and affects up to 34% of diabetic patients during their lifetime. Risk factors for developing a diabetic foot ulcer include:
- Type 2 diabetes being more common than type 1
- A duration of diabetes of at least 10 years
- Poor diabetic control and high haemoglobin A1c
- Being male
- A past history of diabetic foot ulcer.
Also Check: Pasta Bad For Diabetics
Which Ointment Is Best For Diabetic Wound
Hydrogen peroxide is used for very small wounds, but it’s more important to prevent infection when treating diabetic wounds. For a closed incision or wound, you would want to cover the entire surface of the skin with dry non-stick dressing and secure it with adhesive tape.
For an open wound or ulcer, it’s important to cleanse using soap and water as well as to irrigate your wound twice per day in order to maintain a sanitary environment. Wet dressings may be recommended after cleaning which may include sterile gauze/adhesive tapes applied so that the material can absorb any fluids from the surrounding area.
Newer products such as hydrocolloid dressings which are able to create a moist healing environment on surfaces by absorbing wound fluid while protecting the area from infection, dirt, and other external contaminants are available over-the-counter at pharmacies or grocery stores.
If you have a non-healing ulcer after six months of treatment, consult your doctor for further help in promoting wound healing. They may prescribe antibiotics to prevent infections.
Here is a list of supplies required when treating sores on diabetics:
- Hydrogen peroxide
- Non-adherent dressings
- Wet non-adherent dressing
- Cotton balls or cotton swabs
- Gauze pads: regular and compression
- Gauze roll bandages/tubular gauzes
- Tape
- Scissors
Here are some ways you can avoid getting cuts or sores on your feet.
How Are Leg Ulcers Treated
At Cleveland Clinic, patients are treated by a team of world-class experts in the Lower Extremity Wound Clinic in the Department of Vascular Medicine. This Clinic includes doctors, nurses and other medical specialists.
These experts work together to determine the cause of the ulcer and develop an individualized treatment program.
The goals of treatment are to relieve pain, speed recovery and heal the wound. Each patient’s treatment plan is individualized, based on the patient’s health, medical condition and ability to care for the wound.
Treatment options for all ulcers may include:
- Antibiotics, if an infection is present
- Anti-platelet or anti-clotting medications to prevent a blood clot
- Topical wound care therapies
- Prosthetics or orthotics, available to restore or enhance normal lifestyle function
Venous Ulcer Treatment
Venous ulcers are treated with compression of the leg to minimize edema or swelling. Compression treatments include wearing compression stockings, multi-layer compression wraps, or wrapping an ACE bandage or dressing from the toes or foot to the area below the knee. The type of compression treatment prescribed is determined by the physician, based on the characteristics of the ulcer base and amount of drainage from the ulcer.
The type of dressing prescribed for ulcers is determined by the type of ulcer and the appearance at the base of the ulcer. Types of dressings include:
- Moist to moist dressings
- Synthetic skin substitutes
Arterial Ulcer Treatment
Recommended Reading: What Is The Maximum Dose Of Metformin
New Wound Therapytopical Pure Oxygenappears Effective In Healing Food Ulcers
Investigators from Midwestern University invited 73 people who had diabetes, both type 1 and 2, to participate in a study to test this new treatment for diabetic foot ulcers.
They found that nearly 42% of those who were randomly assigned to receive the oxygen therapy experienced significant symptom relief, compared to just 13.5% of those who were treated with regular room air for 12 weeks.2
This new food ulcer therapy is called TWO2 for Topical Wound Oxygen home care therapy. The treatment involves placing an inflatable chamber, similar to a large stocking, over the wound, and then an oxygen generator fills the chamber with pure oxygen administered under pressure.2
As a result of the oxygen therapy, Dr. Frykberg says, “it stimulates production of collagen, growth factor, new blood vessels and increased ability to fight infection.”
Oxygen has long been viewed as crucial in the wound-healing process,3-7 the researchers say. For years, hyperbaric oxygen therapy has been studied intensely to heal foot ulcers and prevent amputation. But results remain inconsistent, the researchers say.
However, Dr. Frykberg and his colleagues say that the use of topically administered oxygen therapy has been hampered by studies that weren’t well designed and complicated by results that were inconsistent.8-10

