What Are The Drawbacks Of Using An Insulin Pump
Your doctor might encourage you to get an insulin pump if:
- You have big swings in your blood sugar levels.
- You cannot find an insulin dose that keeps your blood sugar under control without also causing low blood sugar.
- Your lifestyle makes it hard to stop and give yourself insulin injections.
- Your eating and activity schedule changes often, so you need a more flexible insulin schedule.
- You need to inject yourself with insulin often.
Key Points To Remember
- An insulin pump can free you from a strict regimen of meals, sleep, and exercise, because you can program it to match your changing schedule.
- After you learn how to work with a pump, it can make living with diabetes easier. But it takes some time and effort to learn how to use the pump to keep it working properly and to control your diabetes.
- When you use a pump, you will need to check your blood sugar many times a day or use a continuous glucose monitor. You will need to carefully count the grams of carbohydrate that you eat.
- Using an insulin pump can keep your blood sugar at a more constant level so that you don’t have as many big swings in your levels. People who use pumps have fewer problems with very low blood sugar.
- Many insurance companies cover the cost of insulin pumps, but they have strict guidelines that you will have to follow before they will pay.
How Do Diabetes Costs Affect Small And Medium Businesses
1. Revenue Loss Due to Missed Time
With diabetes comes medical appointments, and without a flexible schedule to attend these appointments, employees with diabetes can cost employers on average $1,500 annually due to missed work and decreased productivity. While employers alone aren’t responsible for the changes Canadians need to better manage diabetes, providing the flexibility to make appointments, offering health benefits, and starting wellness programs can help. In turn, this may lowers costs for the employer and reduce turnover.
2. Smaller Hiring Pool
Due to high costs associated with diabetes, job candidates may turn down a job offer if the health benefits are either too restrictive, or non-existent. As a result, small and medium businesses that don’t provide health benefits shrink the pool from which they can hire, putting them at a disadvantage.;
Recommended Reading: How Can Diabetics Improve Circulation?
Why Should I Use An Insulin Pump
The choice to use an insulin pump instead of injections usually comes down to personal preference. However, you may want to consider an insulin pump if:
- You have frequent low blood sugar reactions.
- You have a condition called gastroparesis, which causes a delay in your stomach’s ability to absorb food.
- You are planning to get pregnant.
- You want to use the pump’s bolus calculator functions to set up insulin doses.
About 25% of people with type 1 diabetes use an insulin pump. Some people switch between injections and pump use. For instance, children may use an insulin pump during the school year but not in the summer.
You can use an insulin pump to give your body insulin, but you still need to check your blood sugar level. By checking your blood sugar regularly, you can make sure that the pump and the infusion are working correctly.
Pumps Connected To A Cgm
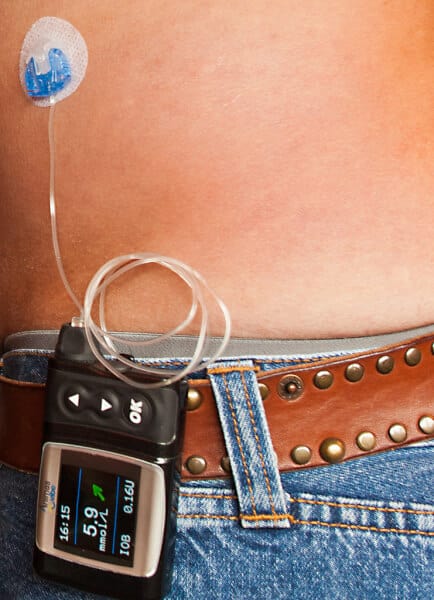
PWDs are increasingly using so-called closed loop systems that connect a CGM with an insulin pump to optimize diabetes control. Medtronic is the only company that actually makes both devices and sells them coupled in one system. The newest commercial closed loop system is from Tandem Diabetes Care, but that connects the Tandem t:slim pump with a Dexcom CGM so two different manufacturers are providing support.
In these connected systems, sometimes a fussy CGM sensor or transmitter can lead to hiccups that make ones insulin pump experience less productive.
How are these companies handling this customer support crossover? Dexcom and Tandem tell DiabetesMine that reps at both companies are well prepared to talk callers through the process of determining whether any problems lie with the pump or CGM, and then directing customers accordingly.
Also Check: Does Diet Soda Raise Blood Sugar
Traveling With A Pump
When traveling , you should always carry several days of extra supplies and all supplies and medications should be kept in your carry on. Make sure all medications, including insulin are in their original container with the prescription label on it. It doesnt hurt to have a letter from your provider stating you are wearing a medical device. Carry syringes and back up long-acting insulin with you when you travel, just in case. Dont forget extra batteries or your charger cable for you pump or CGM.
Your pump is OK to go through screening, but not through the Xray machine. You can also request a pat down rather than having to remove your pump.
If you are going out of the country, many pump companies will offer you a loaner pump to take with you just in case of a malfunction. Its also helpful to change the time on your insulin pump once you arrive at your destination, otherwise you basal rates will not be programmed correctly.
Further reading:
If you are going through a very large time change, talk to your educator about how and when to change the time for your basal. Also, if you are going to be more active on your vacation, you may just plan to set a complete separate basal pattern for while you are away. Just make sure to set an alarm in your phone or leave yourself a note at home to change your time or basal pattern back when you return.
Checklist Before Starting An Insulin Pump
-
Willingness to learn about new pump technology
-
Attend more frequent appointments when starting the insulin pump
-
Learn to carbohydrate count or participate in a DAFNE course
-
See a diabetes educator
-
Be willing to check blood glucose levels multiple times per day
-
Have an understanding of costs of insulin pump
-
Consider taking out private health insurance
Recommended Reading: Normal A1c Levels For Diabetics
What To Do If Your Insulin Pump Malfunctions
Theres nothing quite like the horror of having an insulin pump suddenly go berserk at 11 oclock on a Saturday night. The buttons that dont respond to touch, the shrieking alarms, the critical error notifications signaling you must contact customer service. Its almost enough to induce a panic attack.
Although insulin pumps are the most advanced treatment method of choice for many people with diabetes , they arent perfect. These technical gadgets are just machines, and they sometimes have glitches or malfunction completely.
Of course, according to Murphys Law, an insulin pump will usually die at the most inconvenient moment. That could be just before bedtime or in the middle of the night, while youre on vacation, or during a busy work conference where you just dont have time to deal with device woes.
Whats a PWD to do in these situations? Weve culled the experts and compiled some advice.
Who Should Use A Pump
Insulin pumps have been used successfully across the age spectrum. Whether or not to use a pump is a personal decision. You can manage your diabetes equally well with pumps or multiple injections, so it comes down to your preference.
Choosing one method over the other is not a lifelong commitment. Some people go on and off their pumps . Remember that a pump is just a toolyou can reach blood glucose goals with a pump or injections. But here are some things to consider
You May Like: B12 Dosage For Diabetes
What Are The Advantages Of An Insulin Pump
Insulin Pumps are recommended for the following reasons:
- Eliminates the need for regular injections
-
One needle every 3 days
-
Fewer variations in blood glucose levels
-
Easier & more convenient delivery of insulin bolus
-
Increased flexibility regarding when and what you eat
-
Eliminates the unpredictability of intermediate and long-acting insulin
-
Reduces the need to consume a large amount of carbohydrates in order to exercise
-
Increased accuracy of insulin delivery
-
Ability to give very small doses of insulin
-
Able to set alarms to remind you to check your blood glucose or bolus your insulin
Travelling With An Insulin Pump
While travelling, an accompanying letter on practice letterhead should be provided stating the medical history of the patient, including the diagnosis of type 1 diabetes, and that management is via an insulin pump. A list of current drugs, with generic names and doses, should be included. The letter should stress that it is important that the patients drugs accompany them, and that the insulin pump should not be disconnected. In particular, the pump should not be put through airport X-ray machines.
Prescriptions should be obtained for insulin and other drugs before travel. In case of pump failure both rapid-acting and long-acting insulin should be obtained along with injecting devices and needles. Sufficient equipment for glucose testing should be packed in the hand luggage. In addition to drugs and glucose-testing equipment adequate quantities of consumables should be packed. As a rule, pack twice as many sets as potentially required for the planned period away from home. An adequate supply of consumables should be included in the hand luggage while flying.
Recommended Reading: What Is A High Blood Sugar Reading
What Are The Ongoing Costs
Medtronic infusion sets and reservoirs are available from the NDSS through Diabetes Australia for $25-$30 per month, for patients who meet the criteria. Applications must also be signed and completed by you;before being sent to Diabetes Australia. You should also advise patients of the appropriate infusion set and reservoir for the pump, so that they can order consumables through your state Diabetes Australia office.
Price Of Insulin Pump

If the average insulin pump price is a shocker to take in, what you can do is to weigh some considerations. If you take the diabetes therapy in oral route, a doctors prescribed glipizide may cost you about $32 dollars a month and a maximum dose of metformin is $55. Then add in the pioglitazone for $125 dollars a month. If you add up all the cost, you will realize that its still cost effective to take one dose of the $100 dollar a month, supply of diabetic medicine as compared with all the rest for the pills calculated. Knowing how much does insulin pump costs, can provide you a more informed choice for a cost- effective medication.
How Insulin Pump Works?
Now that you know the average insulin pump price, you will also have to understand how insulin pumps work. What insulin pumps does is that they deliver a rapid acting insulin into your body, using the aid of a catheter placed under the skin. It works for 24 hours a day and is separated into three: the basal rates, the bolus doses and the correction dosses also known as the supplemental doses.
This insulin is being programed on different times of the day, and night. A patient who is eating will have to use the buttons on the insulin pump to give him relief and let the bolus help him cover the carbs in his meal or snack. If a patient is experiencing a high glucose level, all he will need to so is to give himself a correction dose to regulate the insulin level in the body.
You May Like: Is Milk Bad For Diabetics
Components Of Insulin Pump Technology
1. Insulin Pump
An insulin pump is a small, durable electronic device used to program your insulin and display how you are tracking. The device also includes a reservoir compartment.
2. Infusion Set
An infusion set includes a thin cannula that goes from the reservoir to the infusion site on your body. The cannula is inserted into the site, similar to where you would give insulin injections. The infusion set should be changed every two to three days.
3. Reservoir
A reservoir is a plastic cartridge that holds the insulin and is locked into the insulin pump. A reservoir can hold up to 300 units of insulin and should be changed every two to three days.
Looking For An Insulin Pump
The patients doctor is the very best person to figure out if an insulin pump is needed. For patients that do require just smaller, irregular, or infrequent dosages of insulin, the pump is generally not a must.If the doctor recommends a pump, find out what type or brand name of pump they would recommend. You should also ask about what functions or features may be best for the patients requirements.The American Diabetes Association provides a resource guide, consisting of information on specific pumps, insulin choices, and infusion sets.American Diabetes Wholesale and The Diabetes Store offer a range of pumps at competitive rates.Those with insurance coverage will have to talk with an insurance agent prior to acquiring a pump. Ask about the particular pump and devices that will be covered.
Don’t Miss: Why Does Blood Sugar Go Up At Night
Understanding Insulin Pump Settings
Defining pump terms like basal rates, carb ratios, insulin sensitivity, and more
Insulin pumps are devices that deliver insulin without the need for manual injections. Pumps provide fast-acting insulin through a small tube placed under the skin, delivering two types of doses:
-
Basal insulin, delivered continuously in tiny doses throughout the day and night; and
-
Bolus insulin to cover the increase in blood glucose from meals and/or to correct high blood sugars.
Pumps give insulin based on pre-programmed basal and bolus settings read more about these settings below!
Basal
The goal of basal insulin is to hold blood glucose levels steady when you are not eating ideally within a 30 mg/dl range . With the help of a healthcare professional, you can program one or more basal rate settings in your pump.
Basal insulin rate is the rate at which an insulin pump provides small, background doses of fast-acting insulin. The rate is usually programmed as a number of units per hour during a certain time period. For example, someone could program their pump to deliver 1 U/h;from 9am-5pm and 0.7 U/h;from 5pm-9am.
When you first start using an;insulin pump,;your healthcare professional will help you determine your initial basal rate and then carefully adjust;your basal profiles based on frequent blood glucose self-monitoring. The ability to precisely adjust basal rates is one big advantage pumps have over once-daily basal injections. You can read more about basal rate testing here.
Bolus
Pump Therapy In Pregnancy
It is possible to have a healthy pregnancy with diabetes, while on injections. An insulin pump is typically the preferred method of insulin delivery during pregnancy, mainly because insulin needs vary so much throughout the pregnancy, tight control is ideal and the risk of hypoglycemia on a pump is lower than on injections. Not to mention, several pumps have integrated CGMs which are extremely helpful to a pregnant woman aiming for tight control.
Less insulin is needed during the first trimester and 2-3 times the amount of insulin may be necessary by the third trimester. Good blood glucose control before and during pregnancy lead to better outcomes regarding the baby. Starting a pump prior to pregnancy is ideal, but not always the case. A pregnant woman is a great candidate for an insulin pump if she is agreeable to the therapy. Private insurance and government insurance tend to provide good coverage. For more information read our article on Pre-existing Diabetes & Pregnancy.
Possible issues with pump therapy during pregnancy are:
Recommended Reading: What Is A Normal A1c For A Non Diabetic
How Much Time And Effort Commitment Does Pump Therapy Require
Starting pump therapy requires commitment. It is not unusual to check blood sugars 8-12 times per day in the beginning of pump therapy to assess basal and bolus insulin needs. This often means lots of interruptions during the workday and during family time. It also means disturbing your sleep in order to take blood sugar readings in the middle of the night. Think about your schedule and commitments. Talk to your family for support. Plan ahead.
Example #: Carbohydrate Coverage At A Meal
First, you have to calculate the carbohydrate coverage insulin dose using this formula:
CHO insulin dose = ;;;;Total grams of CHO in the meal ÷ grams of CHO disposed by 1 unit of insulin .
For Example #1, assume:
- You are going to eat 60 grams of carbohydrate for lunch
- Your Insulin: CHO ratio is 1:10
To get the CHO insulin dose, plug the numbers into the formula:
CHO insulin dose =
- The carbohydrate coverage dose is 6 units of rapid acting insulin.
- The high blood sugar correction dose is 2 units of rapid acting insulin.
Now, add the two doses together to calculate your total meal dose.
;;;Carbohydrate coverage dose + high sugar correction dose = 8 units total meal dose!
The total lunch insulin dose is 8 units of rapid acting insulin.
Recommended Reading: Difference Between Type 1 And Type 2 Diabetic
How Much Does An Insulin Pump Cost
Most insulin pumps cost thousands of dollars and are purchased through insulin pump companies or durable medical equipment suppliers.;
If you have type 1 diabetes or type 2 diabetes and must use multiple daily injections. Isaacs says most insurance companies cover the cost of insulin pumps. However, you may still need to pay a portion of the price for an insulin pump as part of your insurance deductible.;
There is also the ongoing cost of supplies, such as infusion sets, cartridge syringes, and items to prep the skin where the pump is connected. The costs related to an insulin pump and its supplies can be pricier than traditional insulin injections.;
Quick tip: Check with your insulin or insulin pump manufacturer, as many have programs that help cover the total cost of insulin or insulin pumps.

