What Happens When You Run Out Of Insulin
First, lets talk about the physical process that sets in when a person with diabetes does not get enough insulin into their body.
Very quickly, severe hyperglycemia sets in. That is high blood sugar that leads to a state called DKA, short for diabetic ketoacidosis, which untreated leads to death.
Basically whats doing on is this: insulin helps sugar enter the cells, which use it for fuel. Without insulin, the body cannot access enough sugar to function properly, so your liver begins to turns some of the body fat into acids called ketones. These build up in the bloodstream and spill over into the urine. When these excess ketones get into the blood, the blood becomes acidic, causing DKA: a combination of very high blood sugar, dehydration and shock, and exhaustion.
Symptoms are vomiting and hyperventilation, and eventually passing out and going into a coma. Without treatment, this leads to death.
Generally, the first signs of DKA show up once the blood glucose level has been north of 300 mg/dL for about four hours, but how quickly things get out of hand at that point is highly variable. Some people with diabetes feel ill immediately, while others can wander around in a daze for days.
If you have any residual insulin at all in your system, it can help hold off DKA even when your blood sugar level is high, according to Dr. Silvio Inzucchi, clinical director of the Yale Diabetes Center.
Hospitalizations for DKA are unfortunately on the rise in the United States.
What Causes Diabetic Ketoacidosis
DKA occurs when insulin levels are low. Our bodies need insulin to use the available glucose in the blood. In DKA, glucose cant get into the cells, so it builds up, resulting in high blood sugar levels.
In response, the body starts breaking down fat into a useable fuel that doesnt require insulin. Turning fat into energy produces ketones. When too many ketones build up, your blood becomes acidic. This is diabetic ketoacidosis.
The most common causes of DKA are:
- missing an insulin injection or not injecting enough insulin
- illness or infection
- Black , Asian , and Hispanic people
- people who have overweight or obesity
- people who are middle-aged
- males
Its best to talk with your doctor about your risk factors to make sure you have the right treatment plan in place.
Testing for ketones is one of the first steps for diagnosing DKA. If you have type 1 diabetes, you should have a supply of home ketone tests. These test either your urine or your blood for the presence of ketones.
You can buy these in drug stores or online.
Signs And Symptoms Of Diabetic Ketoacidosis
The most common early symptoms of DKA are the insidious increase in polydipsia and polyuria. The following are other signs and symptoms of DKA:
-
Malaise, generalized weakness, and fatigability
-
Nausea and vomiting may be associated with diffuse abdominal pain, decreased appetite, and anorexia
-
Rapid weight loss in patients newly diagnosed with type 1 diabetes
-
History of failure to comply with insulin therapy or missed insulin injections due to vomiting or psychological reasons or history of mechanical failure of insulin infusion pump
-
Altered consciousness frank coma is uncommon but may occur when the condition is neglected or with severe dehydration/acidosis
Signs and symptoms of DKA associated with possible intercurrent infection are as follows:
-
Fever
References
Glaser NS, Marcin JP, Wootton-Gorges SL, et al. Correlation of clinical and biochemical findings with diabetic ketoacidosis-related cerebral edema in children using magnetic resonance diffusion-weighted imaging. J Pediatr. 2008 Jun 25. .
Umpierrez GE, Jones S, Smiley D, et al. Insulin analogs versus human insulin in the treatment of patients with diabetic ketoacidosis: a randomized controlled trial. Diabetes Care. 2009 Jul. 32:1164-9. . .
Herrington WG, Nye HJ, Hammersley MS, Watkinson PJ. Are arterial and venous samples clinically equivalent for the estimation of pH, serum bicarbonate and potassium concentration in critically ill patients?. Diabet Med. 2012 Jan. 29:32-5. .
Read Also: Does Metformin Cause Liver Damage
What Can You Do To Prevent Or Slow Dka
First of all, be aware of the symptoms, if any. Our own DiabetesMine correspondent Wil Dubois, who landed in the hospital with DKA last year, writes:
The main symptoms of DKA that were told to watch for other than those associated with high blood sugar in the first place, like crazy thirst and peeing like a race horse are nausea or vomiting, abdominal pain, fruity-smelling breath, rapid breathing, and confusion.
Of course, you cant smell your own breath. If you are confused you probably dont know it. And most people arent aware of their respiration rate. So the main warning sign of impending DKA that all type 1s are taught to be alert for is the union of nausea and abdominal pain in the presence of high blood sugar. And I never had any. Nausea or pain, but clearly as my doctor noted, I was experiencing DKA.
If you know that you have missed a shot or are running low / rationing insulin, its a good idea to keep very close tabs on your blood sugar readings and keep ketone test strips handy.
For someone with established type 1 diabetes, if they really face a limitation of their insulin supply, dont let it run out completely! Stretch it out, encourages Inzucchi.
How Is Dka Diagnosed And Treated
If youre suffering from acute DKA, youll be admitted to the ICU for frequent glucose and vital-sign monitoring, and to begin the process of restoring electrolytes via fluid IV. Youll also have constant insulin infusions until the levels of ketones are reduced and your blood-sugar levels return to normal. Once this treatment is underway, recovery is rapid. A typical hospital stay for DKA is only a few days.
Recommended Reading: Does Metformin Cause High Cholesterol
Can Type 2 Diabetes Get Dka
The answer to this question is usually no. And the reason is because when the body can still make insulin, the beta cells prevent ketones from forming. A condition that is more common with type 2 diabetes is called Hyperglycemic Hyperosmolar State or HHS.
HHS is a rare complication of type 2 diabetes which happens when blood sugar levels are very high. Usually blood sugars are twice as high as DKA in the 600-1200 mg/dl range. HHS commonly presents as dehydration, mental impairment, frequent urination, seizures may be present, some insulin is on board which prevents ketone bodies from forming. HHS has a greater than 50% mortality rate.
HHS is often times started by a serious illness such as stroke, infection, or heart attack.
For both of these conditions, the treatment is rehydration, insulin administration, electrolyte replacemnt and treating the underlying cause.
Case Study: Diabetic Ketoacidosis In Type 2 Diabetes: Look Under The Sheets
Brian J. Welch, Ivana Zib Case Study: Diabetic Ketoacidosis in Type 2 Diabetes: Look Under the Sheets. Clin Diabetes 1 October 2004 22 : 198200.
Diabetic ketoacidosis is a cardinal feature of type 1 diabetes. However, there is a strong, almost dogmatic, errant perception by physicians that DKA is a complication that only occurs in patients with type 1 diabetes. This is not true. DKA does occur in type 2 diabetes however, it rarely occurs in the absence of a precipitating event.
Don’t Miss: What Medications Can Raise Blood Sugar Levels
How Long Can Your Body Survive Without Insulin
Naturally, people whose lives depend on taking insulin get very nervous at the thought of not having access to it. We cant help but wonder: in the worst-case scenario, just how long would we be able to hang on without it?
Conventional wisdom says the answer is roughly 3-4 days. But is that really true?
We set out to do some fact-checking.
What Are The Risk Factors For Diabetic Ketoacidosis
Risk factors for developing DKA include:
- Family history of diabetes: If you have a family history of diabetes, you could be at risk for developing Type 1 diabetes. If you have undiagnosed Type 1 diabetes and miss the early signs and symptoms of the disease, you could develop DKA.
- Family history of autoimmune diseases: If you have a family history of autoimmune diseases, you could be at risk for developing Type 1 diabetes. Undiagnosed Type 1 diabetes could result in DKA.
- Poorly managed Type 1 diabetes: If you have Type 1 diabetes and have frequent high blood sugar, don’t take your insulin regularly and dont check your blood sugar often, you’re at a higher risk of developing DKA.
- Poorly managed Type 2 diabetes: DKA is not as common in people with Type 2 diabetes, but those who have ketosis-prone Type 2 diabetes can develop DKA. This is more likely to happen if you have frequent high blood sugar, don’t take your medication regularly and don’t check your blood sugar often.
You May Like: What Does Diabetes Do To Your Body
Check Your Blood Sugar And Ketone Levels
Check your blood sugar level if you have symptoms of DKA.
If your blood sugar level is 11mmol/L or above, and you have a blood or urine ketone testing kit, check your ketone level.
If you do a blood ketone test:
- lower than 0.6mmol/L is a normal reading
- 0.6 to 1.5mmol/L means you’re at a slightly increased risk of DKA and you should test again in 2 hours
- 1.6 to 2.9mmol/L means you’re at an increased risk of DKA and should contact your diabetes team or GP as soon as possible
- 3mmol/L or above means you have a very high risk of DKA and should get medical help immediately
If you do a urine ketone test, a result of more than 2+ means there’s a high chance you have DKA and you should get medical help immediately.
What Is Diabetic Ketoacidosis
Diabetic ketoacidosis, also known as DKA, is a buildup of acids in your blood. It can happen when your blood sugar is too high for too long. DKA is a serious complication of diabetes and could be life-threatening, but it usually takes many hours to become that serious. You can treat it and prevent it, too.
You May Like: What Happens If You Stop Taking Insulin
Diabetic Ketoacidosis Diagnosis And Tests
Test your ketones when your blood sugar is over 250 mg/dL or you have any of the above symptoms of high blood sugar, such as dry mouth, feeling really thirsty, or peeing a lot.
You can check your sugar levels with a urine test strip. Some glucose meters measure ketones, too. Try to bring your blood sugar down, and check your ketones again in 30 minutes.
Your doctor can give you a physical exam, ask about your symptoms, and discuss your medical history. They can order these tests to diagnose DKA too:
- Bloodwork, including metabolic panel and electrolytes
- Urinalysis
- Electrocardiogram
Correction Of Hyperglycemia And Acidosis

Hyperglycemia is corrected by giving regular insulin 0.1 unit/kg IV bolus initially, followed by continuous IV infusion of 0.1 unit/kg/hour in 0.9% saline solution. Insulin should be withheld until serum potassium is 3.3 mEq/L . Insulin adsorption onto IV tubing can lead to inconsistent effects, which can be minimized by preflushing the IV tubing with insulin solution. If plasma glucose does not fall by 50 to 75 mg/dL in the first hour, insulin doses should be doubled. Children should be given a continuous IV insulin infusion of 0.1 unit/kg/hour or higher with or without a bolus.
Ketones should begin to clear within hours if insulin is given in sufficient doses. However, clearance of ketones may appear to lag because of conversion of beta-hydroxybutyrate to acetoacetate as acidosis resolves. Serum pH and bicarbonate levels should also quickly improve, but restoration of a normal serum bicarbonate level may take 24 hours. Rapid correction of pH by bicarbonate administration may be considered if pH remains < 7 after about an hour of initial fluid resuscitation, but bicarbonate can lead to development of acute cerebral edema and should not be used routinely. If used, only modest pH elevation should be attempted , with doses of 50 to 100 mEq over 30 to 60 minutes, followed by repeat measurement of arterial pH and serum potassium.
Also Check: Are Graham Crackers Ok For Diabetics
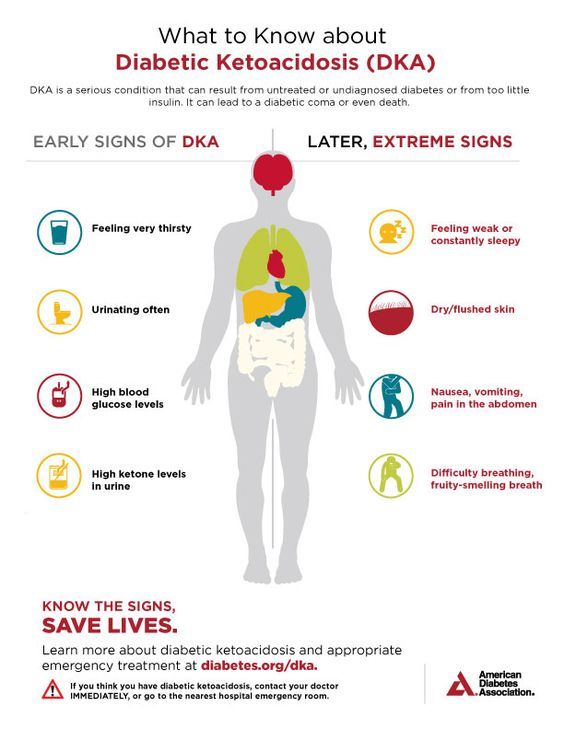
What Are The Warning Signs Of Dka
DKA usually develops slowly. But when vomiting occurs, this life-threatening condition can develop in a few hours. Early symptoms include the following:
- Thirst or a very dry mouth
- Frequent urination
- High blood glucose levels
- High levels of ketones in the urine
Then, other symptoms appear:
- Constantly feeling tired
- Dry or flushed skin
- Nausea, vomiting, or abdominal pain. Vomiting can be caused by many illnesses, not just ketoacidosis. If vomiting continues for more than two hours, contact your health care provider.
- Difficulty breathing
Dka In Type 2 Diabetes
Although DKA is less common in type 2 diabetes, it still happens. Over the last 15 years, I have treated hundreds of type 2 diabetics hospitalized with DKA. People with type 2 diabetes are less familiar with DKA, and many fail to recognize it. I have written this article to help people with type 2 diabetes better understand DKA. It is based on my personal experience as a doctor as well as a thorough review of relevant medical journals.
In this article, you will learn:
Don’t Miss: Metformin And Diuretics
What Can You Do To Avoid Dka
You can help avoid DKA by monitoring your blood sugar levels regularly and altering your insulin dose in response to your blood sugar levels and what you eat.
Your blood sugar levels could be higher than normal when you are unwell. So, its a good idea to work with your healthcare team to come up with some sick day rules for when you are ill. You may need to drink more fluids, take more insulin and check your blood sugars more than you would usually. The amount of extra insulin needed will vary from person to person. Your diabetes team will help you to work out the correct dose for you .
It is still a good idea to contact your GP or diabetes team if:
- You feel fine but are getting higher than usual readings for blood glucose and ketones.
- You feel unwell but your blood glucose and ketones are only slightly higher than normal.
“The experience has taught me that its so important to listen to your body. No matter how many HCPs you visit, whether theyre a GP or a diabetes specialist or a family friend who works in the field, you know your body and you know what feels right and what doesnt feel right. When it comes to diabetes, its so important to trust your instincts.” Amber, 21, had DKA
Who Does Diabetic Ketoacidosis Affect
Diabetic ketoacidosis can develop in people of any age who have diabetes or undiagnosed diabetes.
- Individuals who have undiagnosed Type 1 diabetes: For some people, diabetic ketoacidosis is how they find out that they have Type 1 diabetes. Type 1 diabetes is a chronic autoimmune disease in which your immune system attacks the insulin-producing beta cells in your pancreas. Oftentimes people are in DKA when they’re first diagnosed with Type 1 diabetes because they no longer have enough insulin in their body to use glucose for energy. Type 1 diabetes typically develops during childhood or adolescence but can also develop in adulthood. You can develop Type 1 diabetes even if you dont have a family history of diabetes. Approximately 20% to 40% of DKA cases are from people who are newly diagnosed with Type 1 diabetes.
- Individuals who have Type 1 diabetes: People who have been diagnosed with Type 1 diabetes can develop DKA at any point throughout their life if their body does not get as much insulin as it needs.
- Individuals who have Type 2 diabetes: Although its not as common, people with Type 2 diabetes who have ketosis-prone diabetes can develop diabetic ketoacidosis .
Recommended Reading: Does Metformin Cause Anxiety
How Serious Is Diabetic Ketoacidosis
DKA is a serious medical emergency. Without urgent treatment, this diabetes complication can lead to death. With adequate and rapid intervention and treatment, mortality rates are lowered to around 5%.
If someone with diabetes displays the signs of ketoacidosis, the situation should be treated as an emergency
Key Points About Diabetic Ketoacidosis
|
Contact your doctor or diabetes nurse or go to the nearest emergency department straight away if: |
|
Recommended Reading: How Long Does Nph Insulin Take To Work

