Lawmakers Are Taking Action
Several state legislatures have also tried to deal with this problem. Some have enacted laws mandating drug price transparency and provided funds to guarantee emergency access to insulin.
But to date these assorted responses have failed to lower prices for brand-name insulin products, although I think its possible that prices would have risen faster without them.
Congress is also responding.
The House bill would leave out many patients most notably the uninsured. But this measure would also should the Senatefollow suit.
People living with insulin-dependent diabetes have been waiting a long time for someone to do something to make it more affordable. It looks like that time may finally be arriving.
Why Does Insulin Cost So Much
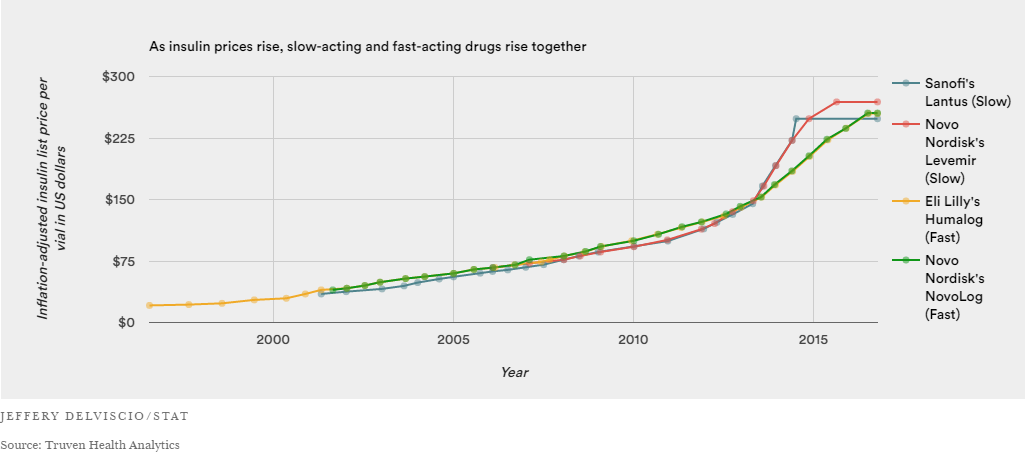
According to one recent study, the cost of insulin tripled in the US between 2002 and 2013. Unfortunately, that kind of inflation isnt unusual for specialty drugs these days. But whats causing insulin prices to keep climbing?
Insulin, a protein that lowers blood sugar, is used to treat diabetes, a group of diseases that causes higher-than-normal blood sugar levels. Until about 30 years ago, insulin was made from pigs and cows.
The era of the biologic genetically engineered proteins that come from human genes brought a more sustainable production process. Today, most insulin is made from the E. coli bacteria. These medicines are much closer to the version produced in the human body, which can mean fewer complications for patients.
Executive Orders On Drug Prices
After the first presidential debate, President Donald Trump claimed of insulin, Im getting it for so cheap its like water. The statement prompted questions about insulin prices following a spate of executive orders that Trump signed over the summer. These orders included language aimed at lowering insulin and other drug prices for Americans.
Recommended Reading: What Is A Normal Dose Of Metformin
What This Means For You
You or a loved one might be paying high prices for insulin. Check with your insulin manufacturer to see if you qualify for a patient assistance program. If you aren’t eligible for these programs, talk to your healthcare provider or certified diabetes care and education specialist about other options.
How To Budget For Diabetes Health Costs
Meanwhile, the idea of offering rebates directly to consumers at the point of sale is picking up steam. In 2018, UnitedHealthcare and Aetna announced that they would begin offering such rebates to some members of commercial plans this year. JDRF called on an additional 23 of largest health insurance companies in the United States to follow suit in November 2018. JDRF advocates prompted Blue Cross Blue Shield of North Carolina to pass on rebates as well, Rice said.
Heilaman says offering consumers rebates seems great in theory, but hes skeptical that anything will cut into the profits of the PBMs and bring real savings to consumers. What we really need is legislation to remove unnecessary middlemen who provide little-to-no service from all aspects of healthcare, he says.
During a Senate Finance Committee hearing on February 26, 2019, drug manufacturer CEOs, including the head of Sanofi, also blamed rebates to PBMs for rising prices of medications and insulin. Meanwhile, bills aimed at bringing down drug costs are stalled in the U.S. Congress.
You May Like: Instant Oatmeal For Diabetics
High Demand Of A Pricey Drug Equals Higher Insurance Premiums
Greene says the math is simple when it comes to insulin: an increased demand plus high prices of insulin result in larger insurance premiums.
He explains that when the original researchers of insulin sold their $3 patent to the University of Toronto, they learned that the demand was too great for them so they went to US drug companies with an offer which entailed that they could have the patent rights on any insulin manufacturing improvements.
Drug companies ran with this opportunity and dramatically changed the quality of insulin available to people with diabetes, improving millions of lives in the process. However, with each new and different insulin version they created came a new patent, which comes with rights against competition for a limited period of time and this kept generic insulin competition out over the years, allowing insulin prices to keep rising.
Eli Lilly is coming out with Basaglar, a follow-on product to Lantus whose patent expired recently and depending on how it works, it may be a suitable Lantus replacement for some people with diabetes. However, we dont know until consumers start using it and the concern is that it wont be much cheaper than Lantus and that it will be the preferred choice among pharmacy benefit managers and insurance but not the preferred choice among consumers.
Is My Test Item Or Service Covered
How often is it covered? Medicare Part B doesnt cover insulin , insulin pens, syringes, needles, alcohol swabs, or gauze. Medicare prescription drug coverage may cover insulin and certain medical supplies used to inject insulin, like syringes, gauze, and alcohol swabs. If you use an external insulin pump, insulin and the pump may be covered as durable medical equipment . However, suppliers of insulin pumps may not necessarily provide insulin. For more information, see durable medical equipment. Your costs in Original Medicare You pay 100% for insulin . You pay 100% for syringes and needles, unless you have Part D. To find out how much your specific test, item, or service will cost, talk to your doctor or other health care provider. The specific amount youll owe may depend on several things, like: Other insurance you may have How much your doctor charges Whether your doctor accepts assignment The type of facility The location where you get your test, item, or serviceContinue reading > >
Don’t Miss: Sugarmd Advanced Glucose Support
Has Competition Been A Negative Factor
Greene writes that In the 95 years since insulin was developed, a number of drug companies have been making and selling it. But even with all those companies making insulin, competition hasnt resulted in lower prices its had the opposite effect. In fact, some brands of insulin have seen prices increase by more than 150 percent in the last five years alone.
He explained that these price increases can spread like wildfire with any competitors raising their prices in step with one another.
Senator Bernie Sanders along with Representative Elijah Cummings have sent a letter to the Department of Justice and the Federal Trade Commission to look into Eli Lilly, Sanofi, and Novo Nordisk for possible price collusion, where companies sync their price hikes with one another in order to raise profits.
So far the three big insulin makers are defending themselves explaining that modern insulin is extremely expensive to create , that the pharmacy benefit managers like Express Scripts, Inc and UnitedHealth Group are raising prices in their negotiations, and that insurance companies are giving people such complicated reimbursement programs that end up causing them to pay higher amounts.
Greene points out that Blue Cross and Blue Shield of North Carolina has been spending more on insulin alongside the consumer. Each year, BCBSNC spends about $250 million on all medications, with insulin making up 13 percent of the total.
Generic Insulin Competition Is Limited
Americans rely on robust competition from low-cost generic drugs to make pharmaceutical products more affordable. This system has historically been more successful with blockbuster drugs like atorvastatin a cholesterol-controlling drug better known by the brand name Lipitor and azithromycin an antibiotic sold under the brand name Zithromax.
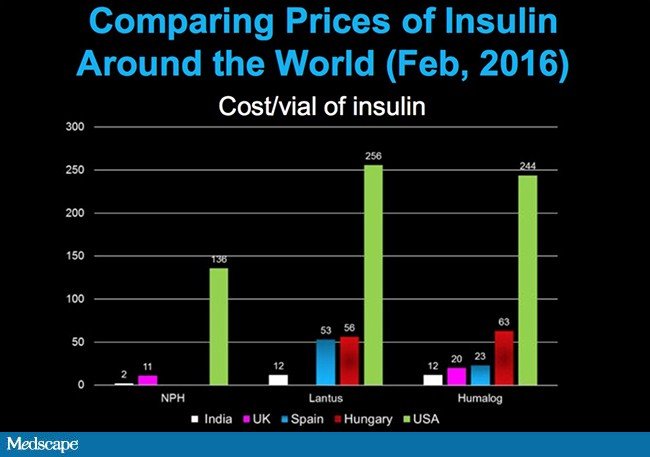
Unfortunately, this system has failed to restrain increases in insulin prices, which are far higher in the United States than other countries.
One reason this has been the case has to do with the fact that insulin is a biologic drug, meaning that its produced using DNA technology by living organisms. Biologic drugs are harder to manufacture and are regulated by the Food and Drug Administration in a different manner than more conventional drugs.
Don’t Miss: Type 1 Diabetes Awareness Ribbon Color
Insulin Has Been Around For 100 Years So Why Is It Still So Expensive
The high cost of insulin in the U.S., where some people with diabetes pay hundreds or even thousands of dollars for a month’s supply, has long been a symbol of our broken healthcare system. Too many people with diabetes have been forced to ration their insulintaking dangerously low doses to make the drug last, while driving themselves into poorer health, and in some cases, poverty.
Though there have been incremental changes recentlya handful of states have placed caps on the cost of insulin, the Affordable Insulin Now act includes a proposed nationwide cap, and some manufacturers and payers have created rebate programs, coupons or caps of their own. But this is not enough for the uninsured and underinsured.
The complexities of the U.S. insulin market are baffling. Manufacturers, pharmacy benefit managers, wholesalers, retailers, payers and employers have created a convoluted, opaque, rebate-driven rat’s nest of a market that sticks patients with the bill. It’s confusing. It’s expensive. And it’s wrong. Over the last 20 years, the average list price of insulin has increased by 11% each year, with annual per capita insulin costs nearing $6,000. Though this structure is not exclusive to the insulin market, it forces too many patients with diabetes who depend on insulin to live to choose between paying for their medicine, their household bills or their food.
It is time to try something different. Something new.
Civica will end this form of highway robbery.
Why Is Insulin So Expensive Right Now
Scientists discovered insulin therapy in 1922 as a derivative of animal insulin, according to an article published in July 2012 in the Journal of Community Hospital Internal Medicine Perspectives. Because the insulin of that era required several injections per day to manage blood sugar, researchers worked on ways to make the drug last longer. In the 1930s insulin makers began adding protamine and zinc to their formulas, extending insulins efficacy to the 24- to 36-hour range. In 1946, isophane insulin, also known as NPH, came onto the market as an intermediate-acting insulin that lasts up to 24 hours.
In 1978 human insulin was synthesized with recombinant DNA technology, and was marketed beginning in 1982. Human insulins currently on the market include rapid-acting regular , which is taken with meals and human NPH .
In the 1990s scientists engineered insulin analogs to have a more reliable duration of action through the modification of amino acid chains, according to the article. Popular analogs currently on the market include fast-acting , Apidra , Humalog as well as intermediate and long-acting Levemir Tresiba and Lantus, Toujeo, and Basaglar .
As the working group explains, the insulin supply chain leading from manufacturer to consumer is complex, with numerous parties including wholesalers, pharmacy benefit managers , employers, insurance health plans, and pharmacies in between that stand to gain or lose based on insulin sales.
Don’t Miss: Bad Carbs For Diabetics
Insulin In America: A Right Or A Privilege
Even as a medical student, I was interested in the history of insulin. As an endocrine fellow, I read The Discovery of Insulin by Michael Bliss . It is a book anyone interested in diabetes should read, as life before insulin is difficult to appreciate by todays standard of care, at least in the United States. Amazing stories of what people did to obtain insulin are plentiful, perhaps none more dramatic than Eva Saxls story, with her husband making insulin in Shanghai, China, for the more than 200 Jews who escaped Nazi persecution during World War II .
But in the United States, access to insulin had never been a problem. As a medication required for survival by 10% of those with diabetes, it was always available, although for decades quite crude by todays standards. The insulin patent from the University of Toronto was sold for $1 with the understanding that cheap insulin would become available . Through the years, insulin remained affordable. Even with the introduction of human insulin in 1982 and then insulin analogs in 1996 , the increases in insulin pricing did not seem to be a concern. At least in the United States, the vast majority of patients requiring insulin had access to all of the insulin analogs as they were developed.
The Role Of Insurance
The ADAs Insulin Access and Affordability Working Group report found that nearly half of Americans have employer-sponsored health insurance. About 20% are insured through Medicaid, and 14% are insured through Medicare. Approximately 7% of Americans purchase health insurance on their owneither directly from an insurer or through a health insurance exchange. About 9% of Americans remain uninsured.
Diabetes is considered a pre-existing condition. According to research published in Diabetes Care, an estimated 1.9 million uninsured people with diabetes gained insurance coverage after the Affordable Care Act went into effect. More than half of those who gained insurance were low-income.
Still, having insurance doesn’t mean insulin is affordable. Insured patients will often pay a copay or a percentage, rather than the list price, for their insulin. Redmond says that cost could range from $30 to $50.
In cases of high-deductible health plans, patients have to pay the list price for their insulin until their deductible is met, which often translates to thousands of dollars out of pocket. Many patients just have a problem paying that much, says Redmond.
Read Also: What Happens When You Stop Taking Metformin
How Much Is A Bottle Of Insulin
The cost of a single vial of insulin varies depending on the type of insulin and whether or not it is covered by insurance. Each insurance plan can cover insulin products differently.
In 2012, the average cost of insulin per diabetes patient was $2,864 per year. By 2016, just four years later, it had risen to $5,705.
Today, one vial of insulin can cost $250 and a pack of pens ranges from $375 to $500. Most patients require two vials of insulin per month or 1-2 packs of insulin pens, but some people need up to six vials per month.
Besides insulin, diabetic patients need other types of medication, which also tend to be high priced. According to a 2016 study, the total average out-of-pocket pharmacy and medical costs for patients with diabetes reached $18,500 in 2016 a surge of $6,000 from 2012 costs, half of which are accounted for by spending on insulin.
As a result of these exorbitant prices, one in four patients say that they ration their insulin because they cant afford full proper doses. In some cases, this practice can cost lives. For patients with type 1 diabetes, just a single day without insulin is enough to send them to the emergency room.
Its Time Everyone Knows About Price Inequities In Insulin
As someone living in the United Kingdom whose daughter has had type 1 diabetes for over 40 years, I find it heartbreaking to know that globally, a lack of insulin is the main cause of death in children living with this condition. Even with this critical fact, there is still an apparent lack of awareness amongst the public, many health professionals and politicians that the issue of access to insulin even exists.
Insulin, which is the only effective medicine used to treat type 1 diabetes, is up to 74 percent higher-priced than other treatments for non-communicable diseases. Little is known as to why the price of insulin is so high, but it is thought to be a result of the global market domination by three multi-national pharmaceutical companies that control 99 percent of the global insulin market.
As a result of this, over the years, we have witnessed the withdrawals of various insulin formulations for commercial reasons. We have also seen a dramatic increase in the more expensive analogue insulins, which even the pharmaceutical companies have described as non-inferior to their predecessors.
Examining shifts in the global market, as well as their trickle-down effect on national health systems, is the key to unlocking some of the answers as to why the price of insulin has remained so high and out of reach to so many in need. Through our work on the ACCISS Study, I am looking forward to discovering some of these answers and ensuring insulin access for all.
Don’t Miss: Is Overnight Oats Good For Diabetics
Generics And Biosimilars Are Driving Down The Overall Price Of Insulins
Since 2019, the overall retail price of insulins has declined by about 5%. Most of this decline can be seen as a result of recent approvals of generics and biosimilars.
In 2019, Eli Lilly released the first generic insulin, insulin lispro, the counterpart to the popular rapid-acting insulin Humalog. Since then, the FDA has approved generic versions of Humalog 75/25 , , , and most recently, Lantus .
Retail prices for generic insulin lispro and insulin aspart are currently about half that of Humalog and Novolog, respectively. The same goes for the generic mixed insulins, insulin lispro 75/25 and insulin aspart 70/30, compared to Humalog 75/25 and Novolog 70/30, respectively.
Generics have been instrumental in bringing down costs for some patients. Instead of paying a retail price of over $700 for a package of 5 Humalog KwikPens, for example, patients can now pay closer to $300 for a package of 5 generic insulin lispro KwikPens. However, weve seen that limited insurance coverage can prevent some patients from accessing these savings.
Like generics, follow-on products have also helped to bring down insulin prices overall. Generics contain the exact replicas of the active ingredients in a brand-name medication. But biologic drugs like insulin are nearly impossible to recreate. So sometimes, manufacturers make close copies of them instead, known as follow-ons or biosimilars. Biosimilars tend to be more expensive than generics but less expensive than brands.

