Insulin For Cell Culture And Organ Preservation
Cell culture, one of the major techniques in life science research, is a complex process by which cells are grown under controlled conditions, in a favorable artificial environment. Insulin is required for the growth and development of cells and also stimulates the proliferation of certain cells in culture . Numerous hormones including insulin are used as an essential component of synthetic growth media for cell culture . Insulin has been found to be stimulatory in serum-free medium for the growth of virtually every cell type including mammalian cells . It is used for the manufacture of monoclonal antibodies, virus vaccines, gene therapy products, and other biological drugs .
Insulin, by increasing the permeability of cell membranes to glucose and making nutrients available to the cells, promotes the growth of mammalian cells . The action of insulin in mammalian cell culture is primarily through the binding and activation of IGF-1R . Mammary tumor cell lines, like the MCF-7 cell line, respond to low levels of insulin, suggesting that the growth-promoting effect is mediated by the IR , . Insulin through the IR also inhibits apoptosis induced by serum withdrawal in a variety of cell types , .
How Did People With Type 1 Diabetes Survive Historically
We hate to break it to you, but they didnt.
Looking at historical records from pioneering diabetes doctors Joslin and Allen before the advent of medical insulin, we see that they were only able to keep patients alive for months, sometimes more than a year, by them to death. Literally.
Dr. Elliott Joslin proudly wrote that, Whereas formerly the prognosis for children less than 10 years of age was measured in months, today it is rare for a child to live for less than one year. Ultimately, all of Joslins pre-insulin patients died. 100 percent of them. Those who didnt starve succumbed once their insulin production dropped to zero.
But of course we now know that the onset of type 1 is a messy affair. The autoimmune process that drives it doesnt happen overnight. Insulin production lingers for many months in a phenomenon called the diabetes honeymoon.
So, history can only show us how long we can suffer starved in the honeymoon phase of the disease, not how long a full-fledged type 1 will last sans insulin in todays modern world.
DKA is the leading cause of death in people with T1D under age 24. But stats indicate that there are only several-thousand deaths from DKA per year in the whole country. Most cases occur right at disease onset, and most receive some sort of medical intervention in a timely manner. The
Articles On Type 1 Diabetes Complications
Cold sweats, trembling hands, intense anxiety, a general sense of confusion — these are signs of low blood sugar. Your doctor may call it . It often happens when you take too much insulin.
Hypoglycemia happens to many people with . It can be serious. Thankfully, most insulin problems can be avoided if you follow a few simple rules.
Diabetes Is A Balancing Act
It can be a bit troublesome to try to get your diet, exercise, and medications straight. All of this effort is to have your A1C stay under 7 percent, so that you are living healthy with diabetes. However, if your A1C starts creeping up, and you have tried many other diabetes medicines in order to try to get your A1C down to no avail, dont balk at starting insulin.
Throwing Away Your Needles And Lancets
Sharps bins and needle clippers are the safest way of disposing of your insulin needles and your lancets. A needle clipper removes the needle from your insulin pen, and is useful when youre out and about. How you get rid of your sharps bin depends on where you live. Your healthcare team should have information to help you get rid of your bin.
Effects Of Excess Insulin
As a diabetic patient who is dependent on insulin, you must measure your requirements for the same very carefully and consider your food intake and level of activity. If you take insulin but eat insufficient amounts of food, your body will use high levels of glucose from your blood resulting in hypoglycemia.
On the other hand, if you are a non-diabetic who takes insulin then the extra amounts of insulin in your body will eliminate the glucose already present in the blood causing your blood sugar level to fall considerably. In some cases the level falls so much that it can even prove fatal for the person. Hence, it is necessary to avoid taking medicines when not advised and also to follow proper dosage, as advised.
Bodybuilding And Insulin Abuse
Insulin is an anabolic hormone, which means it promotes protein synthesis and muscle growth. According to a September 2016 review published in the , bodybuilders have been known to use insulin to try to “bulk up.” But the review’s authors stressed that this is not a good idea . “Athletes are risking long-term harm by using these drugs … potentially resulting in coma and death,” they wrote.
It should also be noted that exercise lowers blood sugar levels, according to the American Diabetes Association, which increases the risk of bodybuilding-related insulin overdose . According to the review, insulin abuse among athletes is a growing problem. The Olympic Committee Medical Commission has banned non-diabetes insulin use since 1998 .
- Insulin is an anabolic hormone, which means it promotes protein synthesis and muscle growth.
- Athletes are risking long-term harm by using these drugs… potentially resulting in coma and death,” they wrote.
Treating An Overdose Of Rapid
How you treat an overdose will depend on how quickly you realise the error.
If the insulin was administered more than 20 minutes ago, act quickly and take a good source of fast-acting carbohydrate immediately, such as glucose tablets or a very sugary drink. Follow this up with sufficient slower-absorbed carbohydrate, such as bread, to prevent hypoglycemia occurring later.
If you realise an error has been made within 20 minutes of injecting, you may not need to take sugar but you should have carbohydrate that will get absorbed relatively quickly. Avoid having fatty foods, if possible, as fat tends to slow down how quickly the carbohydrate acts.
It is common to need 10g of to counteract each unit of insulin. Its generally safer to have too much than too little carbohydrate when treating an overdose of insulin.
Test your blood glucose levels regularly and be on the lookout for symptoms of a hypo. If you feel hypo symptoms, or think you feel them, perform a blood test.
If the overdose is a large overdose, take carbohydrate first and then call your health team or out- of-hours service for advice.
How Long Can Your Body Survive Without Insulin
Naturally, people whose lives depend on taking insulin get very nervous at the thought of not having access to it. We cant help but wonder: in the worst-case scenario, just how long would we be able to hang on without it?
Conventional wisdom says the answer is roughly 3-4 days. But is that really true?
We set out to do some fact-checking.
What Causes Hypoglycaemia In People Without Diabetes
You may feel mild to moderate symptoms of hypoglycaemia if you havent eaten for a few hours.
This can also happen if as a result from using any medication that lowers blood glucose or as a side-effect of another condition or illness.
You should call 111 or contact a doctor immediately if you regularly experience symptoms of hypoglycaemia. Your doctor will carry out a comprehensive examination including a blood test to find out why your blood sugar levels have dropped.
Some common causes of hypoglycaemia include:
Symptoms Of Insulin Overdose
Excess insulin in the bloodstream causes cells in your body to absorb too much glucose from your blood. It also causes the liver to release less glucose. These two effects together create dangerously low glucose levels in your blood. This condition is called .
Your blood needs the right amount of glucose for your body to operate properly. Glucose is the bodys fuel. Without it, your body is like a car running out of gas. The severity of the situation depends on how low the blood sugar level goes. It also depends on the person, because everyone reacts differently.
Insulin In Parenteral Nutrition Solutions
Parenteral nutrition , also known as intravenous feeding, is feeding a person intravenously, bypassing the normal process of eating and digestion. PN formulations are balanced mixes of essential and non-essential amino acids, glucose, fat emulsions, electrolytes, micronutrients, water, vitamins, insulin, and other required vital medications . PN has become one of the imperative primary and adjuvant therapies over the past few years for the treatment of patients with significant disruption in gastrointestinal function like in diseases such as Crohns disease, cancer, short bowel syndrome, and ischemic bowel disease, etc. PN is administered via a central venous catheter or through a peripheral limb vein. PN therapy in acute care institutions is on an average 1014 days duration . The duration of feeding depends on the degree of malnutrition. PN is expensive and also carries higher risk of complications. The major complication is hyperglycemia, which sets the patient at risk for infection. Therefore, insulin is frequently required in PN solutions to control hyperglycemia .
PN is a valuable and necessary medical treatment for several patients providing both nutritional maintenance and life extension at a time when it is not possible to sustain them any other way. Appropriate use of this complex nutrition therapy maximizes clinical benefits while minimizing the potential risk for adverse events.
What To Do If You Forget An Insulin Shot
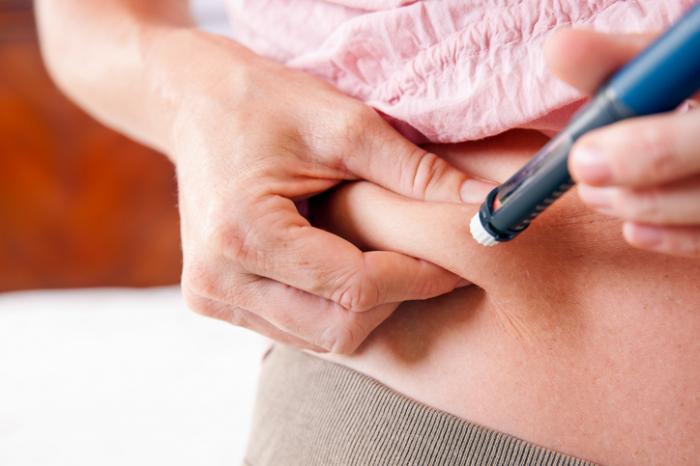
The remedy of missing a dose of insulin is simple; measure your blood sugar. If the amount of mg/dL is in the range don’t act. But if your levels are peaking, take your insulin dose instantly. But do it only when youre 100% sure about you have missed your insulin dose. If you accidentally took insulin twice it can cause complications and severe low blood sugar. If you do forget to take your insulin dose, always test your blood sugar level as soon as possible and take the right dosage according to your sugar levels.
Dont be overwhelmed or panic in such a situation, it happens almost with every diabetic. Sometimes you have the urge to take as much insulin as you can to have a low blood sugar fast. But take in mind that your insulin has a potential working time between 3 and 5 hours and some of them, like Lantus, long-acting insulin, works for 24 hours.
If you missed your long-acting insulin then try to consult your endocrinologist after taking a dose. You may feel a headache but it’s normal. Try to consume more water than your usual routine. Remember, I am not talking about excessive drinking of water, six to eight glasses will be enough.
The worst thing that could happen is that your ketones levels will be disturbed. Ketones are the chemicals that are responsible for fat burning. The best way to check your ketone levels is to check your blood sugar levels via a 2-way blood glucose meter or via ketone sticks.
What Happens When You Run Out Of Insulin
First, lets talk about the physical process that sets in when a person with diabetes does not get enough insulin into their body.
Very quickly, severe sets in. That is high blood sugar that leads to a state called DKA, short for diabetic ketoacidosis, which untreated leads to death.
Basically whats doing on is this: insulin helps sugar enter the cells, which use it for fuel. Without insulin, the body cannot access enough sugar to function properly, so your liver begins to turns some of the body fat into acids called ketones. These build up in the bloodstream and spill over into the urine. When these excess ketones get into the blood, the blood becomes acidic, causing DKA: a combination of very high blood sugar, dehydration and shock, and exhaustion.
Symptoms are vomiting and hyperventilation, and eventually passing out and going into a coma. Without treatment, this leads to death.
Generally, the first signs of DKA show up once the blood glucose level has been north of 300 mg/dL for about four hours, but how quickly things get out of hand at that point is highly variable. Some people with diabetes feel ill immediately, while others can wander around in a daze for days.
If you have any residual insulin at all in your system, it can help hold off DKA even when your blood sugar level is high, according to Dr. Silvio Inzucchi, clinical director of the Yale Diabetes Center.
Hospitalizations for DKA are unfortunately on the rise in the United States.
Treating An Overdose Of Long
If you have given too high a dose of long-acting insulin, this could affect you for up to 24 hours.
How you prevent a hypo will depend on how big the overdose was. If the overdose was large, such as a double dose, take carbohydrate to raise your sugar levels and call your health team or out-of-hours service for advice.
If the overdose was smaller, such as up to 5 units too much, take more carbohydrate than usual and aim to keep your sugar levels higher than normal over the next 24 hours to prevent a hypo occurring.
Test regularly through the day and at any time you think you may feel hypo
Take plenty of carbohydrate before sleeping. It is better to wake up with higher sugar levels than risking a hypo overnight. Dont risk going low. If you cannot be certain that hypos will be avoided, call your health team or out-of-hours service.
How To Reverse Insulin Resistance
If you have insulin resistance, you want to become the oppositemore insulin sensitive .
Physical activity makes you more sensitive to insulin, one reason why its a cornerstone of diabetes management . Dont wait until youre diagnosed with diabetes to start moving more. The earlier you take action , the better off youll be.
Weight loss is important too, as is avoiding high blood sugar, reducing stress, and getting enough sleep .
These lifestyle changes really work. Talk with your health care provider about how to get started.
Insulin For Calcium Channel Blockers And
The overdoses of -blockers and calcium channel blockers may be associated with significant morbidity and mortality . General goals of therapy are aimed at improving inotropy and chronotropy. Important interventions to manage their overdose include intravenous fluids, atropine, glucagon, calcium, and vasopressors. Unfortunately, in severe overdoses, these agents do not consistently improve hemodynamic parameters .
From recent clinical and experimental evidence, HDI therapy has emerged as an effective antidote to calcium channel blocker and -blocker overdose , . In the previous literature reports of calcium channel blocker and combined calcium channel blocker and -blocker ingestions, the majority of patients have received between 0.5 and 2 units/kg/h insulin infusions .
The benefit of insulin in -blocker and calcium channel blocker overdose is anticipated to be related to three primary mechanisms: increased inotropy, increased intracellular glucose transport, and vascular dilatation. Exogenous insulin is believed to improve cardiac function by increasing myocardial carbohydrate metabolism, which in turn expedites myocardial oxygen delivery and cardiac contractility . HDI appears to enhance cardiac contractility without increasing myocardial work, unlike cathecholamines.
What Happens If You Miss A Dose Of Insulin
The human body takes time to adapt to changes. And when we talk about the diabetic lifestyle its a bit difficult to adapt. The most common issue people with diabetes face is to miss an insulin dose.
The major response of the body to insulin deficiency is its antibody reaction. These antibodies start attacking beta cells which resist the movement of glucose from the blood to cells.
Insulin is a hormone that helps your body to maintain blood glucose levels. So, when your body faces its deficiency your blood sugar levels start getting higher. High blood sugar is not less dangerous than low blood sugar. It can cause damage to your organs and cells. When having a long blood sugar for too long your body can reach a diabetic ketoacidosis state.
To control your blood sugar levels you have to consume fewer carbs and take an insulin injection according to your current blood sugar level and acting insulin. In addition to this, your doctor and nutritionist can give you medical advice and help you with your insulin dosage.
What Happens If Type 2 Diabetes Is Untreated
Diabetes is one of the most common diseases in America and the number of people being affected by it is increasing. A recent survey revealed that more than 30 million Americans are currently suffering from diabetes and are adhering to various means of treatment for the same. The main aim of treating diabetes is to prevent the complications. Let us know what happens if type 2 diabetes is untreated for long.
Being a metabolic disease, diabetes cannot be treated completely but can be managed quite well if the patient takes the right medications, consumes a healthy diet and also makes necessary lifestyle changes. For type 1 diabetes and severe type 2 diabetes, insulin injections become a compulsion.
Type 1 Diabetes Disclaimer
This article is not for people with Type 1 diabetes because it is imperative that people with Type 1 diabetes require insulin every day without question. A person with Type 1 diabetes produces very little, or no insulin. Without insulin, you cannot convert food into usable energy. Simply put, without insulin, a person with Type 1 diabetes cannot survive. 2
When Robert contacted TheDiabetesCouncil, he was concerned that one day he would have to take insulin shots for his Type 2 diabetes. He had heard a few of his friends with diabetes at church talking about how they had to take insulin injections. Robert was afraid of needles, and the thought of giving himself a shot scared him.
Is Robert going to need to start taking insulin, or is there any way he can avoid it at this point? If he avoids it, what effects would this have on his health? Will he develop long term complications of diabetes if he doesnt start giving himself shots of insulin?
I suggest also reading these:
At TheDiabetesCouncil, we decided to take a look at this particular question in depth, for Robert and for others with diabetes who might benefit from reading this information.
Factors That Speed Insulin Absorption

Variation in insulin absorption can cause changes in blood glucose levels. Insulin absorption is increased by:
- injecting into an exercised area such as the thighs or arms
- high temperatures due to a hot shower, bath, hot water bottle, spa or sauna
- massaging the area around the injection site
- injecting into muscle this causes the insulin to be absorbed more quickly and could cause blood glucose levels to drop too low.
Can You Lose Weight Using Insulin
You may experience weight loss before you start insulin therapy. The loss of sugar in your urine takes water with it, so some of this weight loss is due to water loss. Also, unmanaged diabetes can make you extra hungry. This can lead to eating an increased amount of food even when you start insulin therapy.
Insulin For Body Building
Athletes use performance-enhancing drugs for muscle-building purposes so as to improve their endurance. Commonly used performance-enhancing drugs in athletes include anabolic androgenic steroids, clenbutarol, erythropoietin, diuretics, growth hormone , and, recently, insulin; all of these have potential health consequences .
Doping is the use of prohibited substances unlawfully to improve their sporting performance and is detrimental to the overall impact of sporting spirit. Doping in sports has been ongoing since the original Olympic Games, with the desire to win at all cost. The International Olympic Committee Medical Commission and sub-commission Doping and Biochemistry in Sport announce annually a list of banned substances and have developed a sophisticated system for detecting drug abuse. Recent evidences suggest that insulin and GH have now become a significant threat in the sports arena .
GH, due to its anabolic and lipolytic properties, which leads to an increase in lean body mass and reduction in fat mass, has been used in sports since the early 1980s . Insulin was used as a doping agent frequently in the Olympic Games, as in Nagano in 1998 , . Insulin with GH is being used by many athletes and body builders for increasing their muscle mass.
Why Is Insulin For Dogs So Important
Since lack of insulin in your dog’s body is the problem, injecting insulin is the only way to manage this condition. Therefore, insulin is the only adequate treatment for a dog with diabetes, and there are different types of it.
While additional exercise and losing weight will improve the quality of your diabetic dog’s life, insulin will be the main medicament for maintaining the condition. Appropriately adjusting diet for a diabetic dog can help a little further with managing the condition.
You can give insulin to dogs as a syringe shot, but recently, insulin pens have become very popular among pet owners. When using a syringe, you’ll need to buy a box of them and a bottle of insulin then inject it the standard way, while with an insulin pen, you’ll be applying a needle tip, choosing a dosage, and then just press a button.
In the past, vets tried to prescribe some other medications, such as oral hyperglycemic, but they proved ineffective as virtually all dogs have the insulin-dependent type of diabetes.
Obligations That Come With Insulin
Insulin needs to be administered twice a day.
After your dog is diagnosed with diabetes, it will take some time until the vet is able to prescribe an adequate dosage of insulin, and there’s going to be some trial and error.
You or your vet will run tests on the dog’s glucose level several times a day or a week in order to see the reaction of your dogs organism to a particular dosage. The positive thing is that once a good dosage is established, the dog wont need the check-ups as often.
Insulin needs to be administered around the same time.
This means creating a schedule around your dogs injections. If you have frequent business trips, irregular working hours, or stay overtime often, you would need to think about the alternatives for keeping up with the schedule. You can ask a friend, family member or a pet sitter to administer it to your dog when you are unable.
Some dog owners feel anxious about giving a shot to their dog, especially because the dog is not thrilled about it either. But giving injections to dogs is fairly simple, and most people get used to it very quickly; it becomes a regular routine for them and their pet.
Exercise Physical Activity And Weight Loss
Its important for people with Type 2 diabetes to be physically active. They should aim to get in at least 30 minutes of physical activity five days per week. If weight loss is desired, a modest goal for weight loss of five to seven percent of body weight will help decrease insulin resistance, and protect remaining beta cells in the pancreas.
Research in the United Kingdom has shown that just a small amount of weight loss around the pancreas will greatly reduce insulin resistance. Overall weight loss can help reduce visceral fat.
What Happens If You Dont Give Your Dog Insulin At All
Not giving your dog insulin will in most cases be like not treating diabetes at all. This can affect the dog’s life expectancy and significantly decrease their life quality.
Apart from less serious effects like excessive urination, thirst and appetite, your dog will experience a significant weight loss. Living with diabetes can impair a dog’s eyesight, and they can develop cataracts and even go blind very quickly.
Your dog can also completely lose appetite, feel weakness and anxiety, and catch other diseases that are not related to diabetes but result from a dog’s organism having to cope with the constant lack of insulin and weakened system.
A diabetic dog’s life expectancy will depend on various factors, such as breed, age, general health, weight and lifestyle. In general, dogs with diabetes can live anywhere from two months to two years if not given insulin.

