Pharma: Biden Freezes Trumps Lower Cost Insulin And Epinephrine Rule
Posted on 01/22/2021
Big pharma is smiling big right now. The big three insulin producers are Eli Lilly and Company, Novo Nordisk A/S, and Sanofi S.A., in which they dominate more than 90% of the world insulin market by value. After swearing-in, U.S. President Joe Bidens HHS froze the Trump administrations December 2020 drug policy that mandates community health centers to pass on all their insulin and epinephrine discount savings to patients.
The rule was finalized in late December 2020. The drug rule was put in place to benefit patients who have a hard time paying for expensive insulin and allergy medication. Former President Trump campaigned on lowering the price of important pharmaceutical drugs like insulin, which is used to treat diabetes, and epinephrine. Diabetes afflicts over a quarter of Medicare beneficiaries and drives billions in Medicare spending every year. More than 20 million Americans have diabetes, in which the body fails to properly use sugar from food due to insufficient insulin, a hormone produced in the pancreas.
Insulin Makers Middlemen Stonewall Strike Back
“This industry is anything but a free market when PBMs spur drug makers to hike list prices in order to secure prime formulary placement and greater rebates and fees,” Grassley said in a statement.
“Our investigation worked to get to the bottom of this. We found that the business practices of and the competitive relationships between manufacturers and middlemen have created a vicious cycle of price increases that have sent costs for patients and taxpayers through the roof.”
Wyden said, “Insulin manufacturers lit the fuse on skyrocketing prices by matching each other’s price increases step for step rather than competing to lower them, while PBMs, acting as middlemen for insurers, fanned the flames to take a bigger cut of the secret rebates and hidden fees they negotiate.”
The American Diabetes Association notes that determining actual costs to consumers is difficult: “out-of-pocket costs vary depending upon the type of health insurance each individual has and the type of insulin prescribed.”
A study by Ohio-based 3 Axis Advisors of 41,000 prescriptions from more than 1,500 independent pharmacies for a three-pack of Lantus Solostar insulin pens shows an average co-pay of about $34, and a median of about $9, for January through October 2020. About 1 in 12 co-pays topped $110.
J.C. Scott, president and CEO of the Pharmaceutical Care Management Association, the trade group representing pharmacy benefit managers, said in a statement:
Inside The Senate Report On Rising Insulin Prices
Editors Note: People who take insulin require consistently affordable and predictable sources of insulin at all times. If you or a loved one are struggling to afford or access insulin, you can build custom plans based on your personal circumstances through our tool, GetInsulin.org.
In January 2021, the United States Senate Finance Committee issued their findings from a two-year investigation into the price of insulin in the US. Their findings are unsurprising to anyone impacted by the cost of insulin. Too many entities manufacturers, pharmacy benefit managers , and insurance companies are driving up the cost of insulin, a life-sustaining drug that insulin-dependent people cannot go without.
The diabetes community has never gotten this level of insight before all of the contracts and deals the Senate Finance Committee were able to investigate were confidential. Below, we break down whats in the Senate Finance Committees 90-page report.
To best understand the findings, here are four definitions you need to know:
Editors Note: See Beyond Type 1s full glossary for the US Healthcare System HERE
Over almost two years, the Senate Finance Committee poured over 100,000 pages of internal documents provided by insulin manufacturers, the three major PBMs, and reports from The Centers for Medicare & Medicaid Services , trying to determine the financial and contractual relationships between the companies.
Some of the top line findings from the report include::
You May Like: Which Pancreatic Cells Release Insulin And Glucagon
The Role Of Insurance Companies
When negotiating with PBMs to create their insurance formularies, i.e. the products that they will provide insurance coverage for, insurance companies also receive portions of the drug rebates. Those rebates often go back to those enrolled under the insurance plans in the form of lower premiums. However, people who require maintenance medications like those for diabetes, asthma, etc. are the bulk of those paying for hefty rebates, while the rebates received by insurance companies themselves get spread amongst the entire population of those enrolled on a health insurance plan.
Over the last several years, further complicating privatized US healthcare, PBMs have merged with health insurance companies, further increasing their leverage, buying power, and ability to control the healthcare market. Express Scripts merged with Cigna, CVS Health with Caremark and Aetna, and Optum Rx became a subsidiary of UnitedHealth Group. These large mergers and acquisitions further complicate an already clunky system built more upon profit than patient care.
From the report, The Internal Revenue Service sought to address this issue in July 2019 when it released guidance that expanded the list of preventive services that an HDHP can cover below the deductible, to include insulin. However, this is a voluntary offering for HDHP plans it is up to the employer to decide if they want to offer this first dollar coverage , which creates an additional cost to the employer.
How Rebates Most Of The Cost Of Your Insulin Work
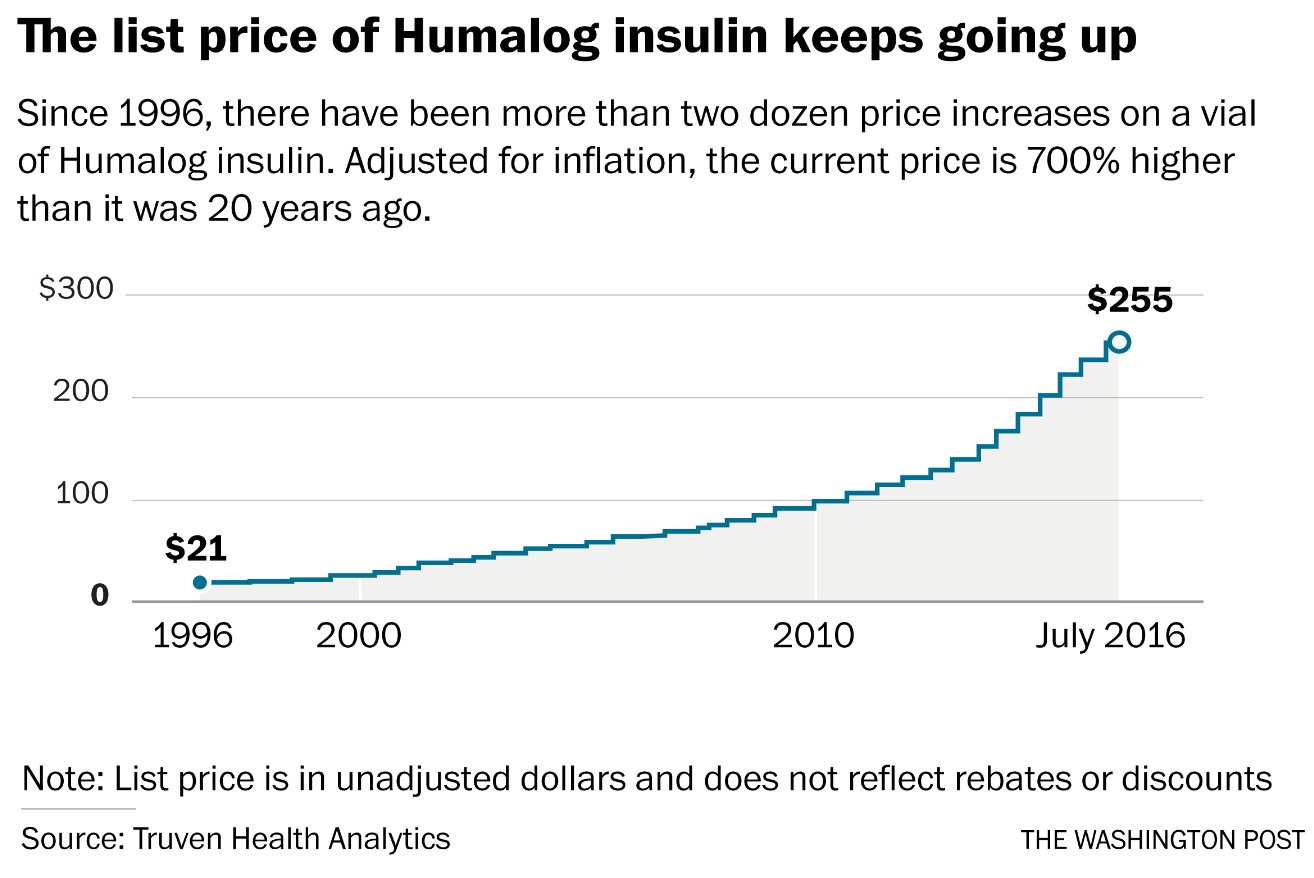
The math is infuriating, but heres the heavily-simplified basics of how rebates work if you made a product for $5 and wanted to sell it, you may set the price at $10, to create a $5 profit. With that $5 profit, you can invest back in your company to create better products, pay yourself whatever you want to do with your $5.
But lets say you want your product to be in more places and available to more people. You might hire a middle person to place your product in new stores across the country, and theyll charge a fee, which is reasonable.
When you begin, their fee is $1. So that you can keep your $5 profit, you raise your price to $11. Still reasonable. But over time, your middle person makes themselves indispensable and knows it. Youre making way more money because of how many products youre able to sell, so youre not about to drop your middle person.
And oh oops you also signed a contract with your middle person to ensure youll always get your product placed in these nation-wide stores, so youre locked in. And part of that contract was an understanding that you wont lower your price, since that would impact your middle-persons profit.
So now, your product costs $50. Its the same product youve never improved it. Your customers are receiving no more value than when the product cost just $10. Over time, you wanted to make more money from it, so your profit is now $10.
Its still $5 to make your product.
Don’t Miss: What Kind Of Candy Can A Diabetic Eat
Overall Insulin Epipen Pricing Isn’t Affected
Nationally, 30 million Americans suffer from diabetes, according to the American Diabetes Association. And nearly one in 50 Americans are at risk for anaphylaxis brought on by certain foods, insect bites, medications and latex, according to a 2013 study by the Asthma and Allergy Foundation of America.
But not all of those patients require insulin or epinephrine. And most who live in extreme poverty, or less than 200% of the federal poverty level an equation that works out to $34,840 for a family of two already receive free or discounted prescription drugs, a national health policy expert said.
Karyn Schwartz, a senior fellow at the Kaiser Family Foundation, a nonpartisan nonprofit that analyzes health policy, said some patients served by the 1,400 federally backed health centers nationally, such as those with high deductibles or those who are uninsured and paying list prices for the drugs, would have benefitted from the new pricing rule.
But it’s hard to say how many, she said. It’s also difficult to speculate about how many new patients would switch care to a community health center to take advantage of the discounted insulin and EpiPen prices, she said.
Reasons Why Insulin Is So Outrageously Expensive
20 Jan 2019, 6:08 p.m. in #insulin4all USA by T1International
Why does insulin cost so much to patients in the USA and around the world? Why is insulin, a widely sold drug of which most forms are now off-patent, so incredibly expensive? These are simple questions, but ones with a number of complicated answers. This post will break some of those answers down and point you in the direction further reading if you want to dive deeper.
1. Only 3 Companies Control 90% of the Global Insulin Market
The big three insulin producers Eli Lilly, Novo Nordisk and Sanofi dominate more than 90% of the world insulin market by value. Often only one of these companies supplies insulin in a country, which means they more or less hold a monopoly there and can set prices as they wish. In some countries, notably China and India, there are domestic insulin companies that can help drive down the price. This means we need more companies in markets like the USA to help bring prices down. Well touch on that a bit further down the list.
2. No Generic Insulin
3.Pay-for-Delay Schemes & Lawsuits
4. Patents
5. Politics
6. Price Fixing
These Business Insider graphs pretty much say it all.
Several lawsuits alleging some form price-fixing are currently in the works. You can read more here and here.
7. Pharma Marketing Schemes
8. Payment for Influence
What Can be Done?
Also Check: What Diabetic Supplies Are Covered By Medicaid
The Claim: President Joe Biden Is ‘reversing’ An Executive Order Put Into Place By Donald Trump To Reduce Patient Costs For Insulin And Epinephrine
For years, members of Congress have pressured drug companies and pharmacy benefit managers to bring under control the rising costs of insulin and epinephrine for millions of Americans with diabetes or allergies.
In July 2020, President Donald Trump signed four executive orders aimed at reining in prescription drug costs. One required that federally qualified health centers, which purchase insulin and epinephrine through what’s called the 340B drug program, pass along any savings they receive from discounted drug prices to medically underserved patients.
The rule blocks health centers from receiving future federal grants unless they charge patients no more than their acquisition price for insulin and EpiPens epinephrine auto-injectors plus a small administration fee.
At the time, the U.S. Department of Health and Human Services said the move would increase access to insulin and EpiPens for the 28 million patients who visit community health centers annually, over 6 million of whom are uninsured.
On the campaign trail last year, Trump made repeated claims that, because of the executive orders, he was succeeding in his promise to lower drug prices.
HHS approved the rule affecting community health centers in December, and it was to go into effect Jan. 22.
A user on Facebook claims President Joe Biden is now “reversing” Trump’s executive order. This is NOT a partisan issue and will harm Americans, reads the Jan. 22 post, which has almost 1,000 shares.
The Cost Of Insulin: What Determines The Cost And How To Save
Government regulation on drug prices has been heavily debated across the healthcare atmosphere. Drug prices seem to be reaching new heights every year. And, insulin prices are no exception. Before rebates or discounts, insulin costs make up approximately $48 billion, or 20 percent, of the direct costs for treating diabetes. Based on current trends, gross insulin costs are projected to reach $121 billion by 2024.
Diabetes is one of the most expensive chronic conditions to treat in the U.S. over a lifetime. With around 30 million Americans living with diabetes and almost 90 million Americans living with prediabetes, insulin may be a household necessity for many people. But what exactly is driving up the cost of insulin and are there ways to save on insulin? Read on to learn more about the cost of insulin.
What determines the cost of insulin?
The cost of insulin depends on the type of insulin and who itâs manufactured by. Three major pharmaceutical companies control the majority of the pricing of insulin in the U.S. These companies include Sanofi, Eli Lilly, and Novo Nordisk. Many people might ask why manufacturers make insulin prices what they are, and the answer is because they can, quite simply.
Insulin savings programs
Don’t Miss: Does Type 2 Diabetes Need Insulin
Sanofi Patient Assistance Connection
The Sanofi Patient Assistance Connection provides free Sanofi insulin products to people with an income at or below 400 percent of the federal poverty level.
The program is open to Medicare Part D enrollees and people without insurance. Youll need to reapply for this program every year.
Manufacturers also offer copay savings cards. These cards can help reduce the amount you pay out of pocket for your insulin. Unlike patient assistance programs, copay savings cards are available regardless of your income.
Its worth noting that Medicare enrollees cant use copay coupons or drug cards.
- Novo Nordisk offers a savings card that reduces the copayments for its products. Your exact savings will depend on the insulin your doctor prescribed, but copayments when using the card range between $5 and $25.
- Eli Lilly. Eli Lilly offers the insulin value program. With the program, you can get most Eli Lilly insulin products for $35 per month. You can use the program with or without insurance, and there are no income limits.
- Sanofi. The Sanofi copay savings card is for people with insurance. It reduces copayments for Sanofi insulin to between $0 and $10. Those without insurance can join the Valyou Savings Program, which allows people to purchase Sanofi insulin for $99 per month.
Trump Boasted He Made Insulin So Cheap Its Like Water Americans With Diabetes Beg To Differ
Early in Tuesday nights presidential debate, President Trump claimed he had drastically lowered the price of insulin, a lifesaving drug taken in some form by more than 7 million Americans with diabetes.
Insulin, its going to it was destroying families, destroying people. The cost, the president said. Im getting it for so cheap its like water.
That came as a shock to the Americans who shell out hundreds of dollars a month on insulin, a number of whom posted triple-digit pharmacy bills to social media immediately after the presidents assertion.
I looked at my husband and slapped my leg and said, Can you believe that! said Tiffany Garrioch, 36, a public health nurse and educator in Minnesota with Type 1 diabetes, who watched the debate with her family.
Were already an underserved and highly vulnerable population, she said. To hear the president say it costs as much as water makes us look like were crybabies or liars.
Insulin costs her $36.76 a day, she said. In 2008, it was $9.81.
Insulin prices have ballooned over two decades, including during the Trump administration. A subset of people who will be able to enroll in Medicare drug plans that cap payments at $35 a month would be insulated from those costs. Otherwise a patient with diabetes can spend hundreds of dollars on a monthly insulin supply.
The consequence of the untenable price of insulin can be measured in body counts, Greene said.
Read more:
Read Also: What Happens In Type 1 Diabetes
The Role Of Pharmacy Benefit Managers
A definition you need to know for this section: insulin WAC is the wholesale acquisition cost, an estimate of the manufacturers list price for a drug to wholesalers or direct purchasers, that does not include discounts or rebates.
Speculated about for some time but difficult to prove because of private contracts is the sheer amount of cash being collected by PBMs. Originally created to help get needed drugs to patients more efficiently, PBMs have unfortunately become a key agitator to high out-of-pocket drug costs.
Page 5 of the report outlines the issue drug manufacturers increased insulin WAC, in part to give them room to offer larger rebates to PBM and health insurers, all in the hopes that their product would receive preferred formulary placement. This pricing strategy translated into higher sales volumes and revenue for manufacturers. In some cases, manufacturers appear to have been concerned that decreasing WAC prices would be viewed negatively by PBMs, since PBMs capture a portion of rebate revenue and are also paid administrative fees based on a percentage of WAC.
From the report, PBMs play a major role in the drug supply and payment chain by negotiating drug rebates and discounts with manufacturers and managing drug benefits for health care payers, including private insurers, employers, and entities that provide coverage under Medicare, Medicaid, and the Childrens Health Insurance Program .
Read Also: Insulin-degrading Enzyme
Rep Degette Newly Atop An Oversight Subcommittee Promises To Grill Drug Industry Ceos And Investigate Insulin Makers
While even the American Medical Association acknowledged in a recent policy statement that guidance and educational materials can help younger physicians become more comfortable with prescribing more affordable insulin alternatives, some doctors maintain that they shouldnt be blamed for the current insulin affordability crisis.
When we first starting using Humalog and Lantus, the difference between the two in terms of cost were minimal, but there were modest differences in hypoglycemia, Dr. Irl Hirsch, a professor of medicine at the University of Washington, told STAT. Since cost wasnt a big concern, how can one blame the physicians?
Branded drug makers deserve a share of the blame for the concentrated market, too.
Their strategy for keeping generic competition at bay? Filing patents lots of them. Each of the major manufacturers has hundreds of unexpired patents related to their products, the devices that deliver the drugs, and the methods for manufacturing them.
Sanofi, which manufactures Lantus, has been singled out in particular for allegedly repeatedly making small changes to its product to file for new patents. It has filed 74 patents on some version of that drug alone, according to I-MAK.
Don’t Miss: How Many Points Does Metformin Lower Blood Sugar

