Does The Time Of Day Of The Exercise Matter
This change in insulin sensitivity throughout the day is important to understand, because if you exercise when you are more insulin sensitive, you may be at greater risk for a low blood sugar. To prevent low blood sugars, you may need to lower the dose of insulin, eat more carbohydrate or both. Check with your medical provider for specific recommendations. The converse also is true. Exercising during periods of insulin resistance may have less blood glucose-lowering effects, so fewer adjustments to insulin dose and carbohydrate intake may be needed.
The History Of A Wonderful Thing We Call Insulin
Since the dawn of time, we have searched for ways to make life easier for us. The modern age has given us some amazing technological advanceswhat we would do without the internet, our iPhones or high-speed travel?
For many people, surviving life without these things sounds rough. However, if you have diabetes, no doubt youre also a big fan of one particular 20th-century discovery: insulin.
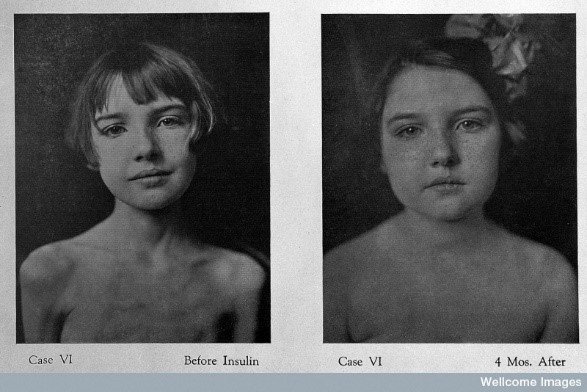
Before insulin was discovered in 1921, people with diabetes didnt live for long there wasnt much doctors could do for them. The most effective treatment was to put patients with diabetes on very strict diets with minimal carbohydrate intake. This could buy patients a few extra years but couldnt save them. Harsh diets sometimes even caused patients to die of starvation.
So how did this wonderful breakthrough blossom? Lets travel back a little more than 100 years ago.
In 1889, two German researchers, Oskar Minkowski and Joseph von Mering, found that when the pancreas gland was removed from dogs, the animals developed symptoms of diabetes and died soon afterward. This led to the idea that the pancreas was the site where pancreatic substances were produced.
Later experimenters narrowed this search to the islets of Langerhans . In 1910, Sir Edward Albert Sharpey-Shafer suggested only one chemical was missing from the pancreas in people with diabetes. He decided to call this chemical insulin, which comes for the Latin word insula, meaning island.
Last edited: August 31, 2020
Choice Of Insulin Regimen: The Combined Oral Drug And Insulin Approach
Many patients and practitioners procrastinate as insulin treatment is erroneously considered to be risky and difficult. However, the regimen used routinely in our clinic is safe and easy to start.2 In our opinion this regimen can be started in general practice. The regimen consists of a combination of intermediate-acting insulin before bed, while continuing maximum oral drug therapy during the day.
Also Check: Does Metformin Increase Insulin Secretion
The History Of Diabetes
People have been aware of diabetes for thousands of years. Learn how discoveries over the ages have led to today’s understanding of diabetes.
Scientists and physicians have been documenting the condition now known as diabetes for thousands of years. From the origins of its discovery to the dramatic breakthroughs in its treatment, many brilliant minds have played a part in the fascinating history of diabetes.
Diabetes: Its Beginnings
The first known mention of diabetes symptoms was in 1552 B.C., when Hesy-Ra, an Egyptian physician, documented frequent urination as a symptom of a mysterious disease that also caused emaciation. Also around this time, ancient healers noted that ants seemed to be attracted to the urine of people who had this disease.
In 150 AD, the Greek physician Arateus described what we now call diabetes as “the melting down of flesh and limbs into urine.” From then on, physicians began to gain a better understanding about diabetes.
Centuries later, people known as “water tasters” diagnosed diabetes by tasting the urine of people suspected to have it. If urine tasted sweet, diabetes was diagnosed. To acknowledge this feature, in 1675 the word “mellitus,” meaning honey, was added to the name “diabetes,” meaning siphon. It wasn’t until the 1800s that scientists developed chemical tests to detect the presence of sugar in the urine.
Diabetes: Early Treatments
Diabetes: How Insulin Came About
Diabetes: Where We Are Today
Other Ways To Lower Blood Sugar Levels
In addition to following a low-carbohydrate diet, physical activity can also help control diabetes by improving insulin sensitivity. A combination of resistance training and aerobic exercise is especially beneficial. Quality sleep is also crucial. Research has consistently shown that people who sleep little are at increased risk of developing diabetes.
A recent observational study found that diabetics who slept 6.5 to 7.5 hours per night had better blood glucose control, compared to those who slept less or longer. Another key to good blood sugar control is stress management. Yoga, Qigong, and meditation have been shown to lower blood sugar and insulin levels.
Bottom Line: In addition to following a low-carbohydrate diet, physical activity, quality of sleep, and stress management can further improve diabetes control.
Read Also: Can I Take Metformin Without Food
Combination Medications For Type 2 Diabetes
Glyburide/metformin , rosiglitazone/metformin , glipizide/metformin , pioglitazone/metformin , and metformin/sitagliptin are five examples of combination pills on the market to treat type 2 diabetes. There are many, many more combination pills available.
These combination drugs carry the benefit of taking fewer pills, which hopefully improves compliance. While they work well, most health-care professionals initiate individual medications to optimize dosing, before switching to a combination pill once the patient has been stable on individual medications for a while.
Starvation Diet Or Restricted Calorie Diet
Frederick M. Allen was the first person to realize that diabetes was more than a problem with high blood glucose levels, but it was a metabolic disorder. Allen helped to provide the best therapy for those with diabetes before insulin, this was known as a restricted-calorie or starvation diet.
The diet provided mainly protein and fat nutrients and restricted carbohydrates. Between the years of 1914 and 1918, 100 patients were treated at Rockefeller Hospital with this method. Other doctors also began prescribing patients with this diet including Elliott Joslin, known as one of the most prominent figures in America for Diabetes. With the starvation diet, patients were given an extra 1 to 2 years of life, but what kind of life did they really have?
You May Like: Can Diabetic Eat Pasta
Ask Google For A Frederick Banting Doodle
There are more than a 366 million people with diabetes in the world. Of those, almost 100 million depend on insulin to live. November 14 is the birthday of Sir Frederick Banting , one of the main discoverers of insulin. His discovery was so significant that this date has been designated as World Diabetes Day by the United Nations. Help us request that Google create a doodle to honor the birthday of this great man, to whom people who inject insulin owe so much, by completing and sharing the petition below. I petition Google to create a doodle to honor November 14, 2012 as the 121st birthday of one of medical historys true heroes: Sir Frederick Banting. He and Charles Best discovered insulin and gave the gift of life to millions of people who had previously been condemned to death. 5,055 people have signed this petition so far.Continue reading > >
November 1920 Great Minds Come Together
In October 1920, Frederick Banting a Canadian surgeon read an article that suggested insulin-producing cells in the pancreas are slower to deteriorate than other pancreas tissue. Banting realised that this might allow for the removal of insulin by breaking down the pancreas in a way that would leave just the cells that produce insulin intact.
But Banting wasnt a scientist and knew he couldnt test his theory alone. On 7 November 1920 he paid a visit to a top professor at the University of Toronto, John Macleod. They put their minds together and began to work on a plan.
Don’t Miss: 168 Blood Sugar After Meal
Putting It All Together
Treating and managing diabetes can seem complicated at times. But your diabetes health care team is there for you. Your diabetes management plan should be easy to understand, detailed, and written down for you so that you can refer to it whenever you need to.
You also might hear about alternative treatments for diabetes, such as herbal remedies and vitamin or mineral supplements. These practices can be risky, especially when people stop following the treatment plan their doctor has given them. So get the facts by talking to your diabetes health care team.
The Discovery Of Insulin And Glycemic Control
Insulin, discovered in 1921 by the legendary Banting, Best and MacLeod collaboration, is nothing short of a miracle. Worldwide, it has saved thousands of patients from certain death.
Before the discovery of insulin, diabetics were doomed. Even on a strict diet, they could last no more than three or four years.
However, despite the many types of insulin and the first oral hypoglycemic agents that came to market around 1957 in Canada, glycemia control the control of blood glucose levels still remains an imprecise science.
In the 1950s, the method a person used to control his blood glucose levels was to drop a reagent tablet into a small test tube containing a few drops of urine mixed with water. The resulting colour from dark blue to orange indicated the amount of sugar in the urine.
Even when they monitored their patients closely, doctors realized that blood glucose levels had to be much better controlled in order to delay the major complications significantly affecting their patients lives: blindness, kidney disease, gangrene, heart attack and stroke.
Don’t Miss: Side Effects Of Stopping Glipizide
Before Banting: Treatments For Diabetes In The Pre
Frederick Banting came up with the idea which led to the discovery of insulin right here at Banting House in 1920. Although the idea of insulin was new, the effects of diabetes were not for many thousands of years, people had been suffering and dying from the disease. So how did doctors help them before insulin had been discovered?
Diabetes was first described in Ancient Egypt around 3500 BCE. Ever since then, physicians around the world tried to test and treat the sugar sickness, as it was called however, with insulin still unknown, diabetics were doomed to waste away. Doctors in Egypt, India, and Greece all watched as the patients they desperately tried to save inevitably fell into comas and died.
During the 18th century, doctors began to understand that diet played a role in diabetes, and that with modification of the diet, its effects could be slowed. They aimed to limit carbohydrates, and increase fat and protein levels in the food that diabetics ate. Fad diets for the desperate in this time included the oat cure, potato therapy, the rice cure, and opium few of which did anything to help.
Today, diabetic diets are still a contentious issue generally, they focus on a balanced diet which is low in saturated fats and processed sugars, and high in soluble fiber. The main concern when discussing diabetic diet is not death, but rather kidney failure and macrovascular disease.
Treating Diabetes: 1921 To The Present Day

Before the discovery of insulin, a diagnosis of diabetes meant certain death.
The lives of people with diabetes has changed considerably in 50 years. They now have specific tools and easier access to information than ever before. The healthcare professionals who treat them also know more about the complexity of the disease, and which treatments work best.
Pending the next medical revolution, Diabetes Québec is demanding the implementation of a national strategy to fight diabetes a strategy founded on education, prevention, support and treatment. The last 60 years have clearly demonstrated that people with diabetes who are well informed, properly supported and treated appropriately live longer lives in better health.
Don’t Miss: What Are The Side Effects From Taking Metformin And Glipizide
May 1921 Experiments Started
Macleod provided Banting with the labs needed to conduct their experiments and brought in a research student, called Charles Best, to help out. Best specialised in testing blood to check glucose levels. This would be the way they would know whether their insulin extracts were having any benefit.
On 17 May 1921 Banting, Best and Macleod first got together to begin their research and set about figuring out how to remove insulin from a dogs pancreas. Their method involved tying off the pancreatic duct to kill off other substances in the pancreas that would destroy insulin, but leave the islets intact. The remaining extract would then be given to other dogs who didnt produce any of their own insulin because their pancreases had been removed to work out its effects on their blood sugar levels.
Different Methods Of Delivering Insulin
Not only is the variety of insulin preparations growing, so are the methods for administering insulin.
Pre-filled insulin pens
In the twentieth century, insulin was available only in an injectable form that required carrying syringes, needles, vials of insulin, and alcohol swabs. Clearly, patients found it difficult to take multiple shots each day as a result, good blood sugar control was often difficult. Many pharmaceutical companies now offer discreet and convenient methods for delivering insulin.
Many manufacturers offer pen delivery systems. Such systems resemble the ink cartridge in a fountain pen. A small, pen-sized device holds an insulin cartridge . Cartridges are available for the most widely used insulin formulations. The amount of insulin to be injected is dialed in, by turning the bottom of the pen until the required number of units is seen in the dose-viewing window. The tip of the pen consists of a needle that is replaced with each injection. A release mechanism allows the needle to penetrate just under the skin and deliver the required amount of insulin.
Insulin pumps
The most exciting innovation in pump technology has been the ability to combine the pump in tandem with newer glucose sensing technology. This is called sensor-augmented insulin pump therapy.
Read Also: Side Effects From Insulin
Throwing Away Your Needles And Lancets
Sharps bins and needle clippers are the safest way of disposing of your insulin needles and your lancets. A needle clipper removes the needle from your insulin pen, and is useful when youre out and about. How you get rid of your sharps bin depends on where you live. Your healthcare team should have information to help you get rid of your bin.
January 1922 Insulin Was First Used In A Human To Treat Diabetes
In January 1922, Leonard Thompson, a 14-year-old boy dying from type 1 diabetes, became the first person to receive an injection of insulin. Within 24 hours, Leonards dangerously high blood sugar levels dropped, but he developed an abscess at the site of the injection and still had high levels of ketones.
Collip worked day and night on purifying the extract even further, and Leonard was given a second injection on 23 January 1922. This time it was a complete success and Leonards blood sugar levels become near-normal, with no obvious side effects. For the first time in history, type 1 diabetes was not a death sentence.
Also Check: Glucose Over 400
What To Tell Patients On The Day They Start Insulin
Although everyone has different information needs, comprehensive information given when starting insulin may confuse many patients. They may not remember the more important messages and some may even be scared away from insulin treatment altogether. Our practice is to concentrate on teaching patients how to inject the insulin subcutaneously into the abdomen, using devices such as the FlexPen or InnoLet which are extremely user-friendly and can be taught in a matter of minutes.
The day patients start insulin is also not an ideal time for detailed dietary advice. We only emphasise the need to have regular meals and snacks containing carbohydrates.
At this stage of diabetes, most patients would be familiar with glucose monitoring and should be asked to perform this. As adjustment of insulin dosage in this regimen is primarily dependent on the morning fasting blood glucose concentrations, testing at this time point is the first priority and should be included every day. For some patients who cannot test their blood glucose for various reasons, it may be necessary to commence insulin without such monitoring and rely on blood glucose monitoring at the doctor’s office and HbA1c concentration to make dose adjustments.
Check Blood Sugar Levels
Checking your blood sugar levels is another part of your diabetes treatment plan. It lets you know how well the other parts of your treatment like your insulin injections and meal plan are working.
Your diabetes care team may recommend that you use a continuous glucose monitor . A CGM is a wearable device that can measure blood sugar every few minutes around the clock. It’s measured by a thread-like sensor inserted under the skin and secured in place. Sensors can stay in place for about a week before they have to be replaced and are accurate enough to replace frequent finger-stick testing. The more frequent CGM blood sugar readings can help you and the care team do an even better job of troubleshooting and adjusting your insulin doses and diabetes management plan to improve blood sugar control.
A blood glucose meter or CGM tells you what your blood sugar level is at the moment. Your doctor may also send you for another type of blood sugar test that tells you how your blood sugar levels have been for the 3 months before the test.
You May Like: Metformin Pioglitazone Side Effects
Diabetes Pills Vs Insulin
Its usually not a case of either pills or insulin. Your doctor will make a recommendation based on the type of diabetes you have, how long youve had it, and how much insulin youre making naturally.
Pills may be easier to take than insulin, but each kind comes with potential side effects. It may take a little trial and error to find the one that works best for you. Pills can stop working even if theyve been effective for some time.
If you start out with only pills and your type 2 diabetes worsens, you may need to use insulin as well.
Insulin also has risks. Too much or too little can cause serious problems. Youll have to learn how to monitor your diabetes and make adjustments as necessary.

