Diagnosis And Tests For Insulin Resistance
Your doctor will use these things to diagnose insulin resistance:
- Questions. Theyâll want to know about your family’s medical history.
- Physical exam. Theyâll weigh you and check your blood pressure.
- Blood tests. You might get:
- Fasting plasma glucose test. This test measures your blood sugar after you havenât eaten for at least 8 hours.
- Oral glucose tolerance test. First, you’ll take the fasting glucose test. Then you’ll drink a sugary solution. Two hours after that, you’ll take another blood test.
- Hemoglobin A1c test. This blood test shows your average blood sugar level for the past 2 to 3 months. Doctors use it to diagnose prediabetes or diabetes. If you have diabetes, it helps show whether it’s under control. You may need to take the test again to confirm the results.
Successful Therapeutic Strategies Help Elucidate Mechanisms Of Insulin Resistance
Dietary changes are common approaches to weight loss, and although most attempts are unsuccessful due to patient noncompliance, there still remains significant controversy surrounding the best dietary approach. A recent review of several dietary interventions suggests that insulin-resistant individuals derive the most short-term benefit from a low-carbohydrate diet compared with a low-fat diet, likely due to the adverse effect that high levels of carbohydrates have on postprandial insulin and triglyceride levels . Although caloric restriction has been shown to decrease the amounts of adipose cells in skeletal muscle and visceral adipose tissue itself, these effects are almost doubled when weight loss is due to exercise in sedentary overweight patients . Rodent studies provide mechanistic insight into the improvements of insulin resistance associated with exercise. Both acute and chronic exercise in a diet-induced obesity rat model lead to suppression of inflammatory signaling in liver, muscle, and adipose tissue that subsequently improved insulin signaling .
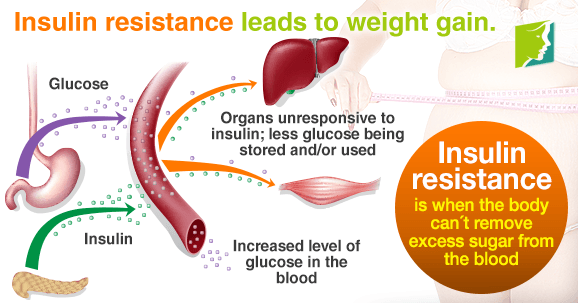
Weight Gain Due To Insulin Resistance
Another thing about insulin is that it plays a primary role in breaking down proteins and fats, other than regulating glucose levels. When indigestion, insulin triggers the fat cells, muscles and liver cells to take up glucose for energy. When your body finds out that there is more glucose than is needed, it will turn the excess sugars into fats to be used in the future. Thus, eating more calories than your body requires can result in weight gain and storage of extra fat, mainly in the abdominal region.
Individuals with diabetes are more likely to suffer from weight gain than other people. The World Health Organization proclaims that about ninety per cent of type 2 diabetic patients suffer from obesity and weight gain. A diabetic patient should go along with a diabetic-friendly diet or use insulin therapy to help lose weight and reduce insulin levels in the body.
Don’t Miss: Eating Too Many Carbs On Metformin
How Can Diet Affect Insulin Resistance
Your diet has a big impact on your blood sugar and insulin levels. Highly processed, high-carbohydrate and high-fat foods require more insulin.
In general, eating foods that have a low to medium glycemic index and limiting foods that have a high glycemic index can help you reverse and/or manage insulin resistance. Eating foods with fiber also helps regulate blood sugar levels because it takes your body longer to digest fiber, meaning your blood sugar levels dont spike as much.
The glycemic index is a measurement that ranks foods containing carbohydrates according to how much they affect your blood sugar levels. The Glycemic Index Foundation classifies the GI of foods as either low, medium or high, with pure glucose generally as a reference at 100:
- Low GI: 55 or less.
- Medium GI: 5669.
- High GI: 70 or greater
High-GI foods generally have a lot of carbohydrates and/or sugar and low to no fiber content. Low-GI foods generally have low amounts of carbohydrates and higher amounts of fiber.
Examples of foods with a high GI include:
- White bread.
- Indigenous people from the continental United States.
- Indigenous people from the Pacific Islands.
Although you cant change certain risk factors for insulin resistance, such as family history or age, you can try lowering your chances of developing it by maintaining a healthy weight, eating a healthy diet and exercising regularly.
Modern Eating Habits Cause Weight Problems
According to Stephens, the modern habit of eating continually causes high blood glucose levelsthat is, the body never gets a break from converting food into glucose. This leads to chronically high insulin levels, since insulin releases to store all that glucose. Since were never out of glucose or glycogen, the body cant access its fat stores, burn them, and lose weight.
and when we deplete them, wed rather fill them back up than get money from the bank . By eating without long breaks, you prevent your body from accessing fat stores, and at the same time you keep your insulin levels high, which promotes increased storage of glucose as fat. In Fungs view, this leads to obesity.)
Recommended Reading: How Many Points Does Metformin Lower Blood Sugar
New Finding On Energy Expenditure
The mice ate similar amounts of food, which raised the question of where the extra calories went in the mice that did not gain weight. To explore the molecular mechanisms involved in this phenomenon, the researchers designed a real-time polymerase chain reaction miniarray of 45 key metabolic, inflammatory, and insulin target genes. They were surprised to find that one of the major sets of genes upregulated in the white adipose tissue of the haploid mice increased the activity of uncoupling proteinsmitochondrial proteins associated with burning energy in brown adipose tissue. This process has been referred to as browning of white fat.
High insulin programs the white fat to really hold onto its nutrients and not burn any of them, Johnson told Endocrine News. If you can reduce the hyperinsulinemia, you have an upregulation of these uncoupling proteins, which will burn energy and increase energy expenditure, with no difference in food intake.
Professor Roy Taylors Work At Newcastle University
Professor Roy Taylor is a professor of medicine and metabolism at the University of Newcastle. He and his research group have focused on understanding if, and how, you can reverse type 2 diabetes.
On the research groups university website, they have stated that type 2 diabetes can be reversed with major weight loss:
It has been possible to work out the basic mechanisms which lead to type 2 diabetes. Too much body fat within the liver and pancreas prevents normal insulin action and prevents normal insulin secretion. Both defects are reversible by substantial weight loss.
Heres our first interaction between weight loss and insulin function. Professor Taylor is saying that if you lose weight, you can also return insulin action and secretion to normal.
- Insulin action: refers to insulin sensitivity, i.e. proper insulin action means theres little or no insulin resistance in the body.
- Insulin secretion: the ability of the beta cells in the pancreas to release insulin into the blood.
The research group goes on to highlight one further critical point. The insulin-secreting function of the pancreas decreases once fat levels go above a persons individual fat threshold.
This threshold varies from person to person and is highly associated with genetics and heritage . This is what they say:
Professor Taylors research paper provides an explanation for the whole cycle, which he has called the Twin-cycle hypothesis.
You May Like: Diabetic Mac N Cheese
Obesity And Insulin Resistance Why Does Insulin Resistance Happen
Insulin resistance can happen due to a combination of genetics and lifestyle leading to an inflammatory process in the body. There are many biological stress factors that can set insulin resistance in motion, including excess nutrition.
When this happens, the body struggles to maintain blood sugar at the correct level. In an effort to keep blood sugar in the normal range, more insulin is secreted from beta cells in the pancreas. A veritable tug-of-war ensues between forces attempting to remove and store sugar in the bodys cells, and those cells themselves that are full and becoming less sensitive to the actions of insulin. At some point, tests for fasting blood sugar, postprandial blood sugars and/or HgbA1c will start to increase. Elevated triglycerides as well as LDL-C may also be seen.
What Happens In The Case Of Insulin Resistance:
– A large amount of sugar enters the blood stream
– Our body responds by signaling our pancreas to release a larger amount of insulin.
– Insulin travels to our cells to tell them to open and take in sugar.
– Instead of opening and taking in the sugar, our cells ignore or resist the insulin.
– Our pancreas reacts by producing more insulin to attempt to get our cells to respond.
– If our cells are not taking in the sugar, then it remains in our blood stream leading to higher blood sugars.
– Eventually our pancreas cannot keep up and blood sugar levels continue to rise putting us at risk for prediabetes and eventually diabetes.
Don’t Miss: Regular Insulin People Also Search For
How Much Exercise Should I Get Per Week
It’s recommended to do at least 150 minutes of moderately intense activity per week. Exercise can include:
- Walking
- Doing work around the house like gardening or vacuuming
It’s also recommended to do strength training exercises a couple of times a week.
Research shows that exercise, even without weight loss, improves blood sugar levels and helps with insulin resistance.
When increasing your exercise time or starting a new exercise program, first discuss how this will affect your medications and blood sugar levels with your healthcare provider before starting. Since exercise can affect these, you may need to make adjustments to your medications or have some snacks with you to prevent low blood sugar levels.
Insulin Sensitivity Vs Insulin Resistance
Insulin sensitivity is the term for how your body responds to insulin. If your body is sensitive to insulin, it means everything is on the right track. The key is turning the locks just fine and there is no need to worry.
But, things become different when resistance replaces sensitivity. When you become resistant to insulin, it means the key is not turning the locks the way it is supposed to. Glucose is not entering into the cells and fat synthesis is on the rise .
You May Like: How Many Points Does Metformin Lower Blood Sugar
Does Metformin Cause Weight Gain
Metformin is a biguanide. Besides the fact that its the most widespread type 2 diabetes and insulin resistance medication, its also the most powerful of its class.
Biguanides work by blocking glucose production in the liver. By impairing gluconeogenesis, it doesnt elevate insulin levels. For this reason, metformin doesnt support hypoglycemia and weight gain.
With this in mind, metformin also isnt worsening diabetes and obesity. Nevertheless, its also not fighting those diseases or weight gain. Hence, metformin is weight neutral .
Although metformin doesnt cause weight gain, it comes with the most common problem of medication.
Metformin is just targeting the symptom, not the root cause.
Since it cant fight the root cause of the diseases, hyperinsulinemia, metformin also cant reverse insulin resistance or type 2 diabetes.
Therefore, metformin is big business for big pharma, because it doesnt take away the illness, but impairs its development.
Once youve started taking it, you almost cant stop using metformin.
And the effective dosage of the drug needs to be increased over time, again and again.
In conclusion, it needs diet and lifestyle changes to reverse insulin resistance, obesity, and type 2 diabetes sustainably.
Losing Weight With Insulin Resistance: Why Is It So Hard
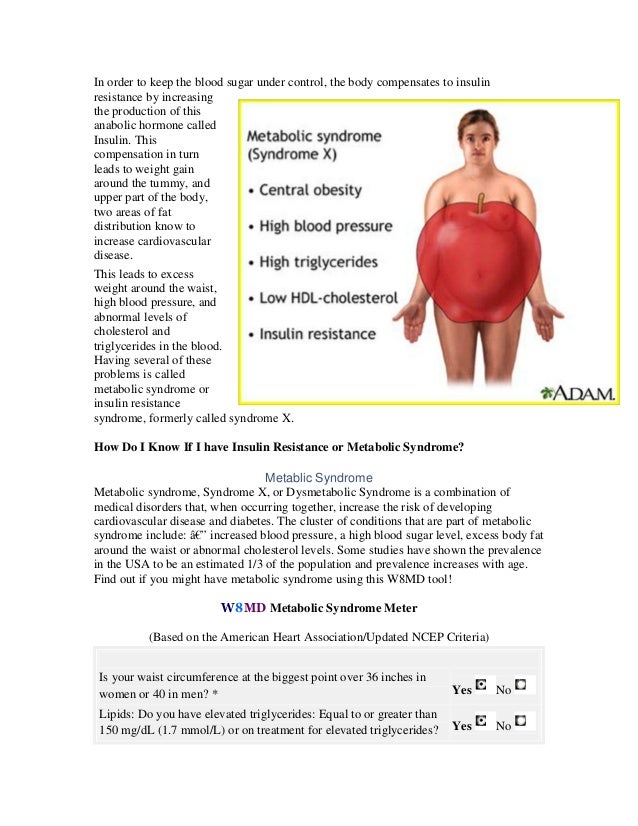
All carbohydrates break down into simple sugars upon digestion. Insulin is necessary to push sugars we ingest through diet into our cells to be used up for energy. When the body is unable to use this insulin efficiently, as is the case with insulin resistance, blood sugar levels spike. With nowhere to go, the body converts these extra sugars into fat and stores it to be used up later. Most of this fat is concentrated around the abdomen.
In a nutshell, losing weight with insulin resistance is difficult because cells are starved of fuel when theyre unable to absorb sugar and nutrients from the blood. This leads to metabolic changes and disturbed appetite regulation, which only adds to your weight loss woes. Ghrelin is a hunger hormone that stimulates appetite, increases food intake and promotes fat storage. Research has found that insulin resistance is linked to decreased plasma levels of active ghrelin and increased belly fat.
Scientists from University of Pittsburgh found that insulin resistance causes triglyceride accumulation in skeletal muscle, leading to obesity. Their findings suggest that the underlying cause was reduced capacity for fat oxidation and not fatty acid uptake. It has also been found that abdominal fat has a significantly stronger relationship with insulin sensitivity than fat gained anywhere else on the body.
Don’t Miss: What Level Of A1c Requires Insulin
What Is The Prognosis For Insulin Resistance
The prognosis of insulin resistance depends on several factors, including:
- The cause of insulin resistance.
- The severity of insulin resistance.
- How well your insulin-producing cells are working.
- How susceptible you are to developing complications from insulin resistance.
- Adherence to treatment and your bodys response to treatment.
People can have mild insulin resistance that never turns into prediabetes or Type 2 diabetes. People can also have insulin resistance thats reversible or very manageable with lifestyle changes. For some people who have inherited conditions that cause severe insulin resistance, it can be life-threatening or lead to death.
If you have insulin resistance, ask your healthcare provider about what you can expect and how best to manage it.
What Does The Hormone Insulin Do
Insulin is a hormone produced by the beta cells of the pancreas and is secreted when blood sugar levels rise. The role of insulin is to transport glucose into the cells so glucose can be used as a source of energy once inside the cells. Insulin acts as a key that locks into receptor sites on the cells to allow the entry of glucose from the bloodstream to get inside cells. Without insulin, glucose would not be able to enter the cell. Thus, cell starvation would result.
You May Like: What Can A Type 1 Diabetic Eat
Hyperinsulinaemia: The Bigger Picture
Inhibition of lipolysis/promotion of lipogenesis, hepatic gluconeogenesis and glucose uptake into insulin-sensitive cells via upregulation of glucose transporter GLUT4 all require different levels of insulin to signal effectively via their receptors. Currently, the most probable explanation is the activation of different insulin signalling pathways in the different tissues, such as the PI3K-Akt pathway versus the MAP kinase pathway . Insulin stimulates glucose transport via the canonical PI3K-Akt pathway, whereas lipolysis is suppressed via Akt-independent suppression of protein kinase A . A further concept is that of selective insulin resistance. Indeed, insulin resistance affects glucose uptake but does not interfere with ChREBP-ß-dependent de novo lipogenesis .
The inverse association between insulin-mediated lipolysis and lipogenesis in adipocytes means that decreased adipose tissue growth is accompanied by increased release of non-esterified free fatty acids from adipocyte triglycerides because of increased lipolysis. Systemic FFAs mostly come from upper body subcutaneous fat and do not reflect visceral adiposity . Individual fasting FFA concentrations vary substantially even if measured on consecutive days . One reason may be that the half-life of FFAs in the circulation is only 24 minutes .
What Causes Insulin Resistance
Scientists still have a lot to discover about how exactly insulin resistance develops. So far, theyve identified several genes that make a person more or less likely to develop insulin resistance. In addition, older people are more prone to insulin resistance.
Several factors and conditions can cause varying degrees of insulin resistance. Scientists believe that excess body fat, especially around your belly, and physical inactivity are the two main contributing factors to insulin resistance.
Acquired causes of insulin resistance
Acquired causes, meaning youre not born with the cause, of insulin resistance include:
Hormonal disorders that can cause insulin resistance
Your body makes hundreds of hormones, which are chemicals that coordinate different functions in your body by carrying messages through your blood to your organs, muscles and other tissues. These signals tell your body what to do and when to do it.
Issues with certain hormones can affect how well your body uses insulin. Hormonal disorders that can cause insulin resistance include:
Genetic conditions that cause insulin resistance
Certain inherited genetic conditions can cause insulin resistance for various reasons.
Theres a group of rare related conditions described as inherited severe insulin resistance syndromes that are considered part of a spectrum. Listed from most mild to most severe, these syndromes include:
Other inherited conditions that cause insulin resistance include:
Recommended Reading: How Long Do Type 2 Diabetics Live
How You Can Turn Tide
Your lifestyle defines your health. Among factors that trigger insulin resistance, an unhealthy lifestyle is the most important.
Here are the top 3 lifestyle changes you need to make right away! These changes will bring your insulin sensitivity and body weight back to normal.
1. Make Systematic Changes in Your Diet Plan
Your diet can make your health or take it away from you. Carbohydrates, proteins and fats are important ingredients of your diet. Heres how these ingredients should look in your diet:
2. Get Adequate Sleep
The importance of sleep cannot be stressed enough. Even a single night of sleep deprivation can reduce insulin sensitivity .
In further research, participants experienced as much as a 44% reduction in insulin sensitivity after only 12 days of shortened sleep . Now imagine what chronic sleep deprivation could do to your insulin sensitivity?
The solution is quite simple. All you need is 7-8 hours of quality sleep daily.
3. Exercise is Important
Exercise makes your insulin work better. It makes insulin open up the gates, just the way it would normally do!
Research shows that regular exercise can improve insulin sensitivity 4-fold .
According to researchers, you should do 150 minutes of moderate intensity workouts on weekly basis. Five sessions, each lasting 30 minutes, would be ideal – but you can still achieve beneficial effects by doing more sessions of, say, 10-20 minutes duration.

