The Insulin Resistance Syndrome
The insulin resistance syndrome describes the cluster of abnormalities which occur more frequently in insulin resistant individuals. These include glucose intolerance, dyslipidaemia, endothelial dysfunction and elevated procoagulant factors, haemodynamic changes, elevated inflammatory markers, abnormal uric acid metabolism, increased ovarian testosterone secretion and sleep-disordered breathing. Clinical syndromes associated with insulin resistance include type 2 diabetes, cardiovascular disease, essential hypertension, polycystic ovary syndrome, non-alcoholic fatty liver disease, certain forms of cancer and sleep apnoea.
Diagnosis Physiology And Treatment Of Diabetes
completed on the connections associated between the central nervous system and DM.Type 1 Diabetes MellitusType 1 diabetes occurs when the pancreas produces little to no insulin, a hormone the body requires providing glucose with the ability to enter cells . It is the absorption of glucose that allows the body to manufacture its energy . T1D affects roughly 5-10% of patients with diabetes and is escalating annually by 2-5% . T1D is a chronic
What Questions Should I Ask My Doctor
If youve been diagnosed with insulin resistance, it may be helpful to ask your healthcare provider the following questions:
- Whats causing my insulin resistance?
- What can I do to increase my insulin sensitivity?
- Whats my risk of developing prediabetes or Type 2 diabetes?
- Is there any medication I can take?
- Should I see a specialist for insulin resistance?
A note from Cleveland Clinic
Insulin resistance is a complex condition that can affect your health in several ways. Since it doesnt have any symptoms until it turns into prediabetes or Type 2 diabetes, the best thing you can do is try to prevent and reverse insulin resistance by maintaining a healthy weight, exercising regularly and eating a healthy diet. Unfortunately, though, not all causes of insulin resistance can be prevented or treated. If you have any questions about your risk of developing insulin resistance or conditions associated with it, talk you your healthcare provider. Theyre there to help you.
Last reviewed by a Cleveland Clinic medical professional on 12/16/2021.
References
You May Like: Hyperglycemia Prognosis
Other Functions Of Insulin In The Body
Along with glucose regulation, insulin also plays a crucial role in other areas of the body. To this end, involving insulin in:
- It modifies the activity of enzymes and the resulting reactions in the body.
- It builds muscle after disease or injury via the transport of amino acids to muscle tissue, which is required to repair muscle damage and increase size and strength.
- It can help to regulate amino acid absorption, DNA replication, and protein synthesis.
- It manages the synthesis of lipids by absorption into fat cells that convert to triglycerides.
- It manages protein and lipids failure due to changes in fat cells.
- Its absorption of amino acids and potassium into cells cannot occur in the absence of insulin.
- It manages sodium excretion and fluid volume in the urine.
- It increases the memory and learning capacities of the brain.
Insulin plays many essential roles in the body. It includes managing sugar levels in the blood and many other areas.
The Important Roles Of Insulin And Glucagon: Diabetes And Hypoglycemia
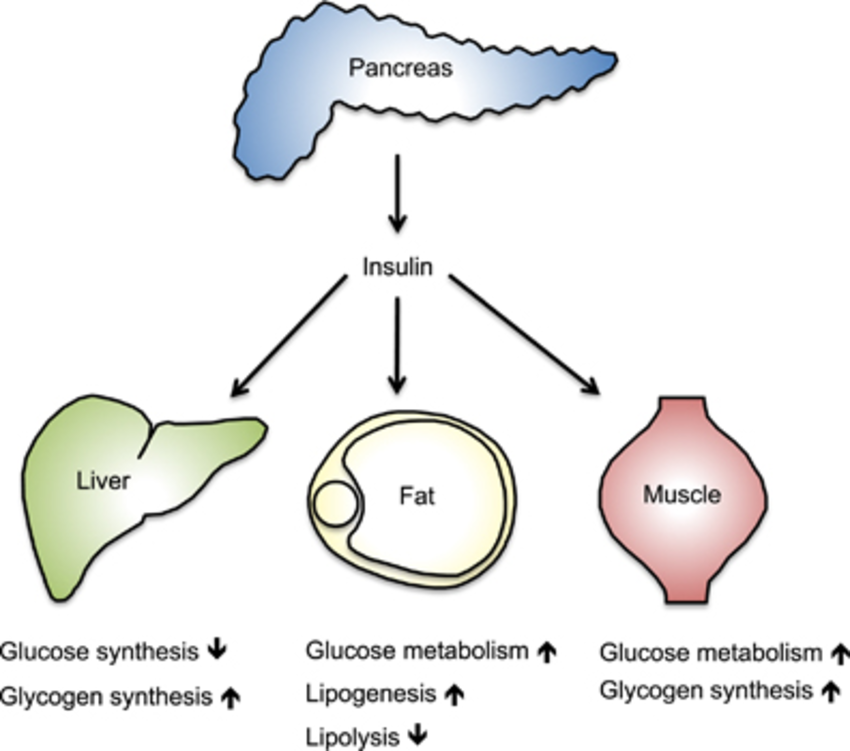
The human body wants blood glucose maintained in a very narrow range. Insulin and glucagon are the hormones which make this happen. Both insulin and glucagon are secreted from the pancreas, and thus are referred to as pancreatic endocrine hormones. The picture on the left shows the intimate relationship both insulin and glucagon have to each other. Note that the pancreas serves as the central player in this scheme. It is the production of insulin and glucagon by the pancreas which ultimately determines if a patient has diabetes, hypoglycemia, or some other sugar problem.
Read Also: Does Metformin Cause Sleepiness
Structure And Chemical Properties Of Insulin
Insulin was found to be a polypeptide in 1928 with its amino acid sequence identified in 1952. It is in fact a dipeptide, containing A and B chains respectively, linked by disulphide bridges, and containing 51 amino acids, with a molecular weight of 5802. Its iso-electric point is pH 5.5. The A chain comprises 21 amino acids and the B chain 30 amino acids. The A chain has an N-terminal helix linked to an anti-parallel C-terminal helix the B chain has a central helical segment. The two chains are joined by 2 disulphide bonds, which join the N- and C-terminal helices of the A chain to the central helix of the B chain. In pro-insulin, a connecting peptide links the N-terminus of the A chain to the C-terminus of the B chain.
What Happens If I Have Too Much Insulin
If a person accidentally injects more insulin than required, e.g. because they expend more energy or eat less food than they anticipated, cells will take in too much glucose from the blood. This leads to abnormally low blood glucose levels . The body reacts to hypoglycaemia by releasing stored glucose from the liver in an attempt to bring the levels back to normal. Low glucose levels in the blood can make a person feel ill.
The body mounts an initial ‘fight back’ response to hypoglycaemia through a specialised set of of nerves called the sympathetic nervous system. This causes palpitations, sweating, hunger, anxiety, tremor and pale complexion that usually warn the person about the low blood glucose level so this can be treated. However, if the initial blood glucose level is too low or if it is not treated promptly and continues to drop, the brain will be affected too because it depends almost entirely on glucose as a source of energy to function properly. This can cause dizziness, confusion, fits and even coma in severe cases.
Some drugs used for people with type 2 diabetes, including sulphonylureas and meglitinides , can also stimulate insulin production within the body and can also cause hypoglycaemia. The body responds in the same way as if excess insulin has been given by injection.
Recommended Reading: Can Type 1 Diabetics Donate Blood
What Else Does Insulin Do In The Organism
Except for regulating blood glucose levels in the organism, insulin hormone is responsible for many other vital functions, for example:
- enhancing the absorption of amino acids by cells
- enhancing the transport of potassium ions into the cell, as well as magnesium ions and phosphate ions
- enhancing DNA replication and protein biosynthesis
- enhancing the synthesis of fatty acids and their subsequent esterification: in adipose tissue and in the liver, insulin promotes the conversion of glucose into triglycerides with a lack of insulin, the opposite occurs the mobilization of fats.
- anti-catabolic effects:
- inhibition of protein hydrolysis reducing protein degradation
- reducing lipolysis reducing the flow of fatty acids into the blood.
As you see, insulins role in our bodies is more than significant, so we should take care to maintain a normal level of insulin in the bloodstream for the proper functioning of our systems and good health.
Functional Measures Of Insulin Resistance
Another approach is to identify insulin resistant patients, based on functional markers of insulin resistance. McLoughlin et al were able to identify insulin resistant individuals from an overweight-obese cohort by looking at plasma triglyceride concentration, ratio of triglyceride to high-density lipoprotein cholesterol concentrations and insulin concentration. Using cut points of 1.47 mmol/L for triglyceride, 1.8 mmol/L for the triglyceride-high-density lipoprotein cholesterol ratio and 109 pmol/L for insulin, they achieved comparable sensitivity and specificity to the Adult Treatment Panel III to diagnose the metabolic syndrome.
Recommended Reading: Side Effects Of Diabetes Type 1
When Should I See My Healthcare Provider About Insulin Resistance
If youve been diagnosed with insulin resistance or conditions related to insulin resistance, its important to see your healthcare provider regularly to make sure your blood sugar levels are in a healthy range and that your treatment is working.
If youre experiencing symptoms of high blood sugar or prediabetes, contact your healthcare provider. They can run simple tests to check your blood sugar levels.
If you have a family history of diabetes or conditions that can cause insulin resistance, talk to your healthcare provider about your risk of developing insulin resistance.
Measurement Of Insulin And Insulin Resistance
There are a variety of approaches to the laboratory assessment of insulin resistance. Over the years the limited specificity of older radio-immunoassays that cross-react with proinsulin have reduced the credibility of measuring insulin resistance in clinical settings. Current assays have improved specificity and precision. A comprehensive review of insulin assays is beyond the scope of this review and the reader is encouraged to consult Sapin in this regard. Insulin resistance may be measured by looking directly at insulin mediated glucose uptake in the basal or post-stimulated state, by inference from the relative concentrations of glucose and insulin, or by looking at surrogate markers of insulin action.
Don’t Miss: Metformin Withdrawal
The Mapk Signaling Pathway
The MAPK pathway is activated when IRS-1 binds to growth factor receptor-bound protein 2 . SOS binds to Grb2 and then to Ras, causing GDPâGTP exchange and the activation of Ras.
Activated Ras recruits c-Raf, which phosphorylates and activates MAPK/Erk kinase . MEK then phosphorylates extracellular signal-regulated kinase . Once activated, Erk is translocated to the nucleus, where its subsequent phosphorylation and transcriptional activation by transcription factors, such as ELK1, ultimately promote cell division, protein synthesis, and cell growth .
What Are The Different Types Of Insulin
The American Diabetes Association characterizes insulin by how fast it works. But everyones body is different. If you have diabetes, you should expect deviations in the amount of time any medication takes to reach your bloodstream. Here are a few useful terms related to how fast and how long insulin acts in your body:
- Onset is defined as the length of time before insulin hits your bloodstream and begins to lower blood glucose.
- Peak is the time during which insulin is at its maximum effectiveness at lowering your blood glucose levels.
- Duration is the length of time insulin continues to lower your blood glucose levels.
These are the five main types of insulin that doctors prescribe:
Recommended Reading: Is Metformin Bad For Your Heart
What Will Insulin Be Like In The Future
Pharmaceutical companies are working on very long-acting versions of insulin that could last for a week. There is also an ultra-fast version of insulin under development that will act in less than 15 minutes.
Another group of researchers is looking at glucose responsive insulin , which would react to the needs of your body in real time. It would have nanosensors bound to the insulin so that when insulin is needed, it releases, and when it isnt, it stops, according to Dr. Hirsch.
What Does Insulin Do In My Body
Diabetes mellitus , often referred to as diabetes, is characterized by high blood glucose levels that result from the bodys inability to produce enough insulin and/or effectively utilize the insulin. Diabetes is a serious, life-long condition and the sixth leading cause of death in the United States. Diabetes is a disorder of metabolism . There are three forms of diabetes. Type 1 diabetes is an autoimmune disease that accounts for five- to 10-percent of all diagnosed cases of diabetes. Type 2 diabetes may account for 90- to 95-percent of all diagnosed cases. The third type of diabetes occurs in pregnancy and is referred to as gestational diabetes. Left untreated, gestational diabetes can cause health issues for pregnant women and their babies. People with diabetes can take preventive steps to control this disease and decrease the risk of further complications.Continue reading > >
Also Check: Does Metformin Have Side Effects
Other Ligands For The Insulin Receptor
Insulin-like growth factors are so-called because they have significant structural homology with proinsulin but mainly mitogenic effects, significantly regulated by growth hormone. IGF-1 and 2 are coded for on the long arm of chromosome 12 and short arm of chromosome 11 respectively. They have specific receptors and bind with different affinities to the various IGF binding proteins. Insulin can bind to the receptors for IGF-1 and 2 but with much lower affinity respectively. IGF-1 binds weakly to the insulin receptor, with only 1.25×103 the affinity for the IGF-1 receptor it binds the IGF-2 receptor with 1/4 the affinity for the IGF-2 receptor. IGF-2 does not bind to the insulin receptor it does bind the IGF-1 receptor but with 1/3 the affinity for the IGF-2 receptor. Therefore overlap in physiological functions is more limited in vivo.
Energy Creation And Distribution
The function of insulin is to help transform glucose into energy and distribute it throughout your body, including the central nervous system and cardiovascular system.
Without insulin, cells are starved for energy and must seek an alternative source. This can lead to life threatening complications.
You May Like: Why Does Metformin Cause Gas
Physiological Roles Of Insulin
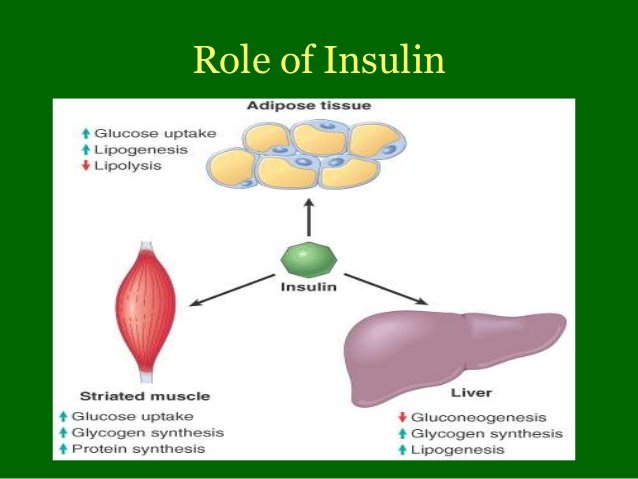
The major purpose of insulin is to regulate the bodyâs energy supply by balancing micronutrient levels during the fed state . Insulin is critical for transporting intracellular glucose to insulin-dependent cells/tissues, such as liver, muscle, and adipose tissue. Any imbalance in exogenous energy supplies results in the breakdown of fats stored in adipose tissue and eventually accelerates insulin secretion. In the following sections, we discuss the major role of insulin in regulating several insulin-dependent tissue/organ functions.
Types Of Insulin Treatments
All types of insulin produce the same effect. They are used to mimic the natural increases and decreases of insulin levels in the body during the day. The makeup of different types of insulin affects how fast and how long they work.
The type of insulin youll be prescribed will vary depending on things like:
- your age
- how long it takes your body to absorb insulin
- how long insulin stays active in your system
| Insulin type | ||
|---|---|---|
| varied peaks | 10 to 16 hours | Taken twice a day, commonly 10 to 30 minutes before breakfast and dinner. This type is a combination of intermediate- and short-acting insulin. |
Talk with a doctor about the right insulin for you and your lifestyle.
You May Like: Metformin Joint Pain Side Effects
How To Choose The Right Method For Injecting Insulin
Both syringes and insulin pens use a small needle to inject insulin into your body. There are pros and cons to each, and which one you ultimately end up with will depend on your lifestyle and your doctors advice.
Things to know about insulin syringes:
- They come in a few different sizes.
- Your doctor will tell you how much insulin you need per dose.
- You will usually draw the insulin into the syringe when you need it.
- Theyre not as discreet as an insulin pen.
Things to know about insulin pens:
- Some pens use cartridges that are manually inserted into the pen.
- Other pens are prefilled and thrown away after all the insulin is used.
- Needles in pens are often smaller than those in syringes.
- Not all types of insulin can be used with a pen.
- Pens can be more expensive than syringes and are sometimes not covered by insurance.
Insulin Basics: How Insulin Helps Control Blood Glucose Levels
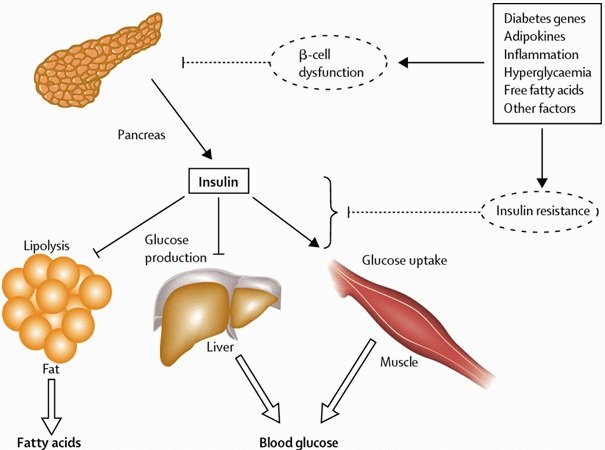
Insulin and glucagon are hormones secreted by islet cells within the pancreas. They are both secreted in response to blood sugar levels, but in opposite fashion!
Insulin is normally secreted by the beta cells of the pancreas. The stimulus for insulin secretion is a HIGH blood glucose…it’s as simple as that! Although there is always a low level of insulin secreted by the pancreas, the amount secreted into the blood increases as the blood glucose rises. Similarly, as blood glucose falls, the amount of insulin secreted by the pancreatic islets goes down.
As can be seen in the picture, insulin has an effect on a number of cells, including muscle, red blood cells, and fat cells. In response to insulin, these cells absorb glucose out of the blood, having the net effect of lowering the high blood glucose levels into the normal range.
Glucagon is secreted by the alpha cells of the pancreatic islets in much the same manner as insulin…except in the opposite direction. If blood glucose is high, then no glucagon is secreted.
When blood glucose goes LOW, however, more and more glucagon is secreted. Like insulin, glucagon has an effect on many cells of the body, but most notably the liver.
You May Like: Diabetes Complications Severity Index
How Should I Store My Insulin
Like food, insulin doesnt have a forever shelf life. Its recommended that you store any insulin youre not using in the fridge.
However, injecting cold insulin may make the injection feel more painful. Because of this, a best practice is to keep the bottle of insulin youre currently using in a safe place, away from direct heat and sunlight. Insulin kept at room temperature can last about a month.
Do not store insulin in the freezer, and always check the expiration date before using it.
Side effects from injecting or receiving insulin are rare, but can occur in certain cases. The symptoms of mild allergic reactions are swelling, itching, or redness around the injection area. More severe insulin allergies may include nausea and vomiting.
In either case, talk with your doctor if you notice any of these signs.
Hypoglycemia, or blood glucose levels that are too low, can sometimes occur when you take insulin.
Its important to balance the insulin that you give yourself with food or calories. If you exercise longer or harder than usual or dont eat the right amount of calories or carbs, your glucose level can drop too low and trigger low blood sugar. Symptoms of low blood sugar include:
Physiology Of Insulin Secretion
Glucose is the principal stimulus for insulin secretion, though other macronutrients, hormones, humoral factors and neural input may modify this response. Insulin, together with its principal counter-regulatory hormone glucagon, regulates blood glucose concentrations. Pancreatic cells secrete 0.251.5 units of insulin per hour during the fasting state, sufficient to enable glucose insulin-dependent entry into cells. This level prevents uncontrolled hydrolysis of triglycerides and limits gluconeogenesis, thereby maintaining normal fasting blood glucose levels. Basal insulin secretion accounts for over 50% of total 24 hour insulin secretion. Following secretion of insulin into the portal venous system, 60% is subsequently removed by the liver so portal vein insulin concentrations reaching the liver approach triple that of the peripheral circulation. In healthy lean individuals circulating venous fasting insulin concentrations are about 315 mIU/L or 1890 pmol/L. Meal-related insulin secretion accounts for the remaining fraction of the total daily output.
Also Check: Side Effect Of Glucophage 500 Mg

