Diabetic Ulcers And Sores: Treatment & Preventio
A leg ulcer is a long-lasting sore that takes more than 2 weeks to heal. They usually develop on the inside of the leg, just above the ankle. The symptoms of a venous leg ulcer include pain, itching and swelling in the affected leg. There may also be discoloured or hardened skin around the ulcer, and the sore may produce a foul. Pressure ulcer in the diabetic foot. All patients with neuropathic or neuroischaemic feet are at risk of pressure ulcers, especially of the heel. Pressure over heel ulcers can be off-loaded by pressure relief ankle foot orthoses. This orthosis is a ready-made device that has a washable fleece liner with an aluminium and polyproprylene. By the WoundSource Editors In patients with diabetes, the lifetime risk of diabetic foot ulcers is approximately 25%, and these wounds are frequently a source of pain and discomfort. Severe cases can even result in amputation of a portion of or the entire affected extremity. Proper classification of DFUs is essential for selecting the appropriate treatment course and coordinating care.
Yellow Reddish Or Brown Patches On Your Skin
Necrobiosis Lipoidica
This skin condition often begins as small raised solid bumps that look like pimples. As it progresses, these bumps turn into patches of swollen and hard skin. The patches can be yellow, reddish, or brown.
You may also notice:
- The surrounding skin has a shiny porcelain-like appearance
- You can see blood vessels
- The skin is itchy and painful
- The skin disease goes through cycles where it is active, inactive, and then active again
necrobiosis lipodica.
Take action
- Get tested for diabetes, if you have not been diagnosed.
- Work with your doctor to better control your diabetes.
- See a dermatologist about your skin. Necorbiosis lipodica is harmless, but it can lead to complications.
Diabetic Skin Conditions Pictures
So, the skin of a patient becomes woundable but even when it is undamaged there are other unpleasant conditions of diabetic skin . They develop on toes, fingers, legs and other parts of the body. It can be hard and waxy skin of the hands, when fingers can hardly bend. This thick and swollen-looking skin can spread all over the body even to face. It looks like an orange peel and shows that there is too much insulin in blood.
People suffering from high glucose level tend to get skin infections causing pain, tiny blisters with white discharge. Besides, there are several types and reasons for diabetic rash, which can be of various colors, sizes, and forms. For example diabetic yeast infection rash can be result of thrush, systemic candidiasis, and others. So, what does diabetic skin look like? The answer depends on the type of affect.
Read Also: What Is The Lowest Dose Of Metformin You Can Take
Is Diabetic Foot Curable
Diabetic foot infections are a frequent clinical problem. About 50% of patients with diabetic foot infections who have foot amputations die within five years. Properly managed most can be cured, but many patients needlessly undergo amputations because of improper diagnostic and therapeutic approaches.
What Does Diabetic Skin Rash Look Like
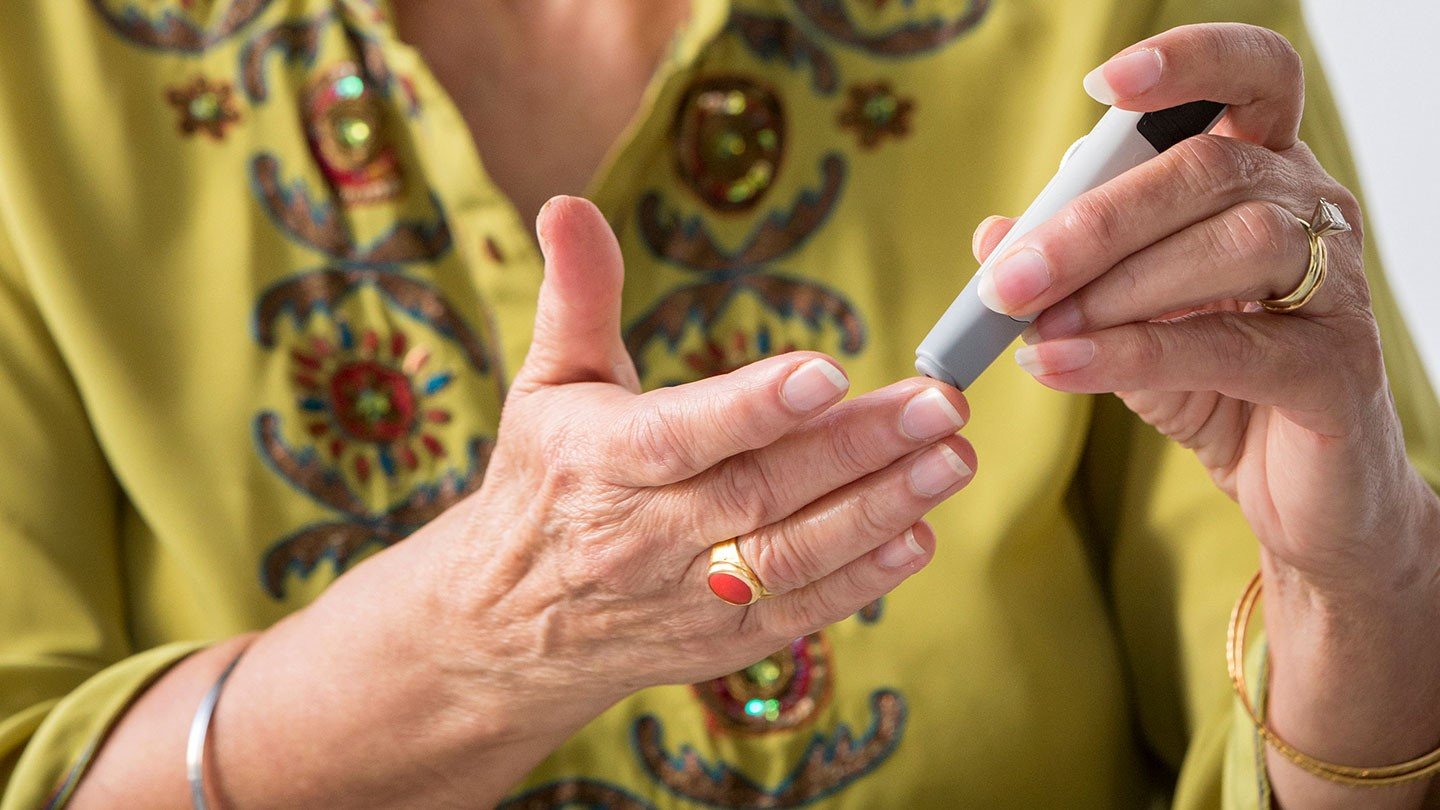
Diabetics are more vulnerable to several different kinds of skin issues because of the effects of their blood/glucose levels on the body. Its essential to check yourself very carefully for skin issues, and to make sure your diabetes is as well controlled as possible.
As well as some common issues, there are a few more complicated skin issues that are caused by diabetes, which are also worth knowing about. So how do you know whats what?
Dry skin: rashes related to diabetic circulation issues can look hyper- or hypo-pigmented or red , and are generally dry, cracked, hot, itchy or inflamed.
Injection site rash: diabetics can get rashes around injection sites, which look bumpy, itchy or spotty.
Fungal infections: fungal infections like thrush can cause itchy, red rashes in and on the genitals, warm or damp folds of skin, and on the tongue. Other fungal infections can cause sore, cracked rashes at the corners of the mouth or between the toes . Another fungal infection that diabetics are vulnerable to is ringworm, which appears as a circular, scaly, itchy ring on the skin.
Bacterial infections: bacterial infections can appear as rashes or inflamed areas, commonly as boils or styes on the eyelids, as well as on finger or toe nails.
Other conditions associated with diabetes that can cause rashes:
Disseminated granuloma annulare: itchy, raised rings or arcs of rashes on the skin, often found on fingers and ears, but also on the body.
Read Also: Type 1 Diabetes Tips And Tricks
Diabetic Dry Skin On Legs Pictures
Diabetic dry skin on legs is a very frequent complication of diabetes as far as the level of blood sugar is very high. In this case the derma becomes itchy and can crack easily welcoming the infection of different kinds. Here the deep sores can develop, which are discussed above. Sometimes one can observe diabetic rash on legs of small size and various colors: light yellow, or reddish, or even purple. In addition the spots can appear.
Anyway diabetes reduces blood flow to the skin damaging blood vessels, nerves and decreasing the blood circulation that causes the changes in collagen development and as a result in skin texture and other its features. The abnormal state of derma irritates, diabetic skin rash appears, it itches and leads to slow healing diabetic foot ulcer becoming deep and large involving all the other heavy consequences.
Can Diabetes Go Away
While diabetes is incurable, a person can stay in remission for a long time.
No cure for diabetes currently exists, but the disease can go into remission.
When diabetes goes into remission, it means that the body does not show any signs of diabetes, although the disease is technically still present..
Recommended Reading: How Does It Feel When Your Blood Sugar Is High
What Does A Diabetic Foot Look Like
A healthy diabetic foot should look like any other foot! A diabetes diagnosis doesnt automatically come with a pair of disfigured feet. However, it can be a challenge to keep the healthy feet you were born with. Diabetics are at a higher risk for many common foot problems than the general population, and are therefore often warned to be vigilant and keep an eye on their feet. Education in this area is evidently lacking, however, because many diabetics report not being given much direction about what to look for. They may understand that foot complications are a risk, but fail to grasp the severity of the risk or commonness of the ailments, and therefore turn their attention to more pressing tasks.
This lack of knowledge and complacency can be the biggest hazard when it comes to diabetic foot care. Taking an active role is absolutely essential to foot health and overall health when it comes to diabetes. Diabetics looking to take better care of their feet should start by keeping them clean and checking them at least once a day for anything out of the ordinary. Read on to discover what potential warning signs to look for and how to lower your risk for developing serious diabetic foot issues.
You should talk to your doctor if you notice any of the following issues, or anything else that looks unusual to you. Dont be afraid to call up your doctor, even if it seems silly. When it comes to your health, its always better to be safe than sorry. Look out for:
How Do Diabetic Foot Ulcers Form
Ulcers form due to a combination of factors, such as lack of feeling in the foot, poor circulation, foot deformities, irritation , and trauma, as well as duration of diabetes. Patients who have diabetes for many years can develop neuropathy, a reduced or complete lack of ability to feel pain in the feet due to nerve damage caused by elevated blood glucose levels over time. The nerve damage often can occur without pain and one may not even be aware of the problem. Your podiatric physician can test feet for neuropathy with a simple and painless tool called a monofilament.
Vascular disease can complicate a foot ulcer, reducing the bodys ability to heal and increasing the risk for an infection. Elevations in blood glucose can reduce the bodys ability to fight off a potential infection and also retard healing.
You May Like: Diabetic Face Rash
How Can I Reverse Diabetes Naturally
Scientists have not yet found a way to cure or reverse type 1 diabetes. Someone with type 2 diabetes may reverse the condition by losing weight. A person is in remission if their blood sugar levels are normal for six months or longer. However, remission is not a cure for type 2 diabetes because the disease may return.
When To See Your Doctor
If you experience any of these symptoms, dont wait for your next appointment. See your regular doctor or foot doctor right away:
- Pain in your legs or cramping in your buttocks, thighs, or calves during physical activity.
- Tingling, burning, or pain in your feet.
- Loss of sense of touch or ability to feel heat or cold very well.
- A change in the shape of your feet over time.
- Loss of hair on your toes, feet, and lower legs.
- Dry, cracked skin on your feet.
- A change in the color and temperature of your feet.
- Thickened, yellow toenails.
- Fungus infections such as athletes foot between your toes.
- A blister, sore, ulcer, infected corn, or ingrown toenail.
Most people with diabetes can prevent serious foot complications. Regular care at home and going to all doctors appointments are your best bet for preventing foot problems .
Recommended Reading: 112 Blood Sugar After Eating
Diabetes: 12 Warning Signs That Appear On Your Skin
Diabetes can affect many parts of your body, including your skin. When diabetes affects the skin, its often a sign that your blood sugar levels are too high. This could mean that:
-
You have undiagnosed diabetes, or pre-diabetes
-
Your treatment for diabetes needs to be adjusted
If you notice any of the following warning signs on your skin, its time to talk with your doctor.
What Does The Start Of A Diabetic Foot Ulcers Actually Look Like
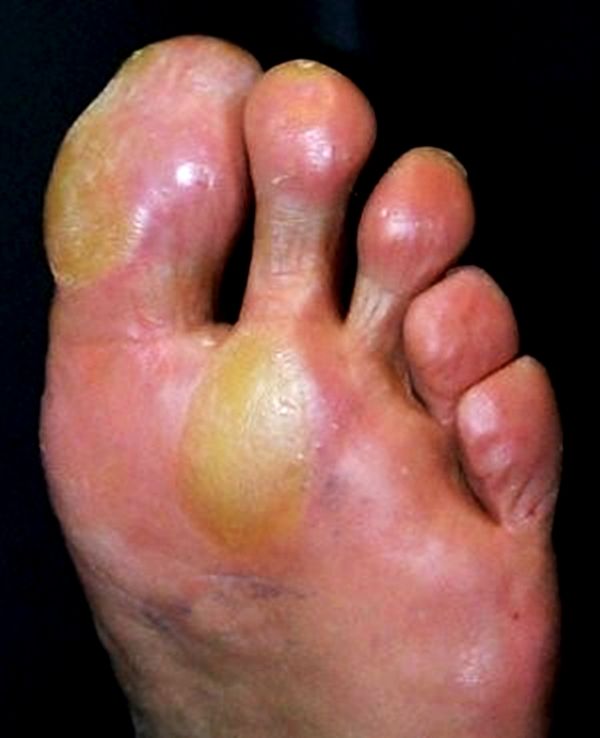
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
Ask U.S. doctors your own question and get educational, text answers â it’s anonymous and free!
HealthTap doctors are based in the U.S., board certified, and available by text or video.
Recommended Reading: Diuretics That Don’t Raise Blood Sugar
How To Prevent Diabetic Blisters
Its important to be vigilant about the condition of your skin if you have diabetes. Blisters and lesions may go unnoticed if you have neuropathy. There are steps you can take to prevent blisters and to keep from developing secondary infections when you have the lesions:
- Inspect your feet thoroughly each day.
- Protect your feet from injury by always wearing shoes and socks.
- Wear shoes that arent too tight.
- Break in new shoes slowly.
- Wear gloves when using scissors, hand tools, and gardening equipment that can cause blisters.
- Ultraviolet light causes blisters in some people. Apply sunscreen and limit exposure to the sun.
Contact your doctor if you develop blisters. Most blisters will heal themselves, but there is risk of secondary infection. The following symptoms warrant an immediate call to the doctor:
- redness around the blister
- warmth radiating from the lesion
- pain
What Do Diabetic Sores Look Like
Having uncontrolled high glucose during a continuous period of time a person can get nerve damage and poor blood circulation, which cause round, deep diabetic sores hard to be healed. Especially they are often on the feet. Such conditions of foot skin are also known as diabetic ulcers. The slightest cut can develop in a serious problem and even result in amputations. The color of an ulcer with puffed border is pinkish red to dark brown.
Even without damage the skin becomes thinner and even dragging on shoes can lead to diabetic wounds , which usually swell, and further inflammation can start. The doctor sometimes has to remove the upper tissue in order to prevent or to cure an infection if it penetrates and will recommend keeping a sore clean changing protective bandage. It should be mentioned that there is a popular term diabetic legs including wounds appearing from diabetic blisters . The blisters look like irregularly-shaped bumps with clear fluid inside mostly painless but itchy.
Don’t Miss: Greek Yogurt Diabetes
It Starts Because Of Trauma Of Any Nature
What do diabetic sores look like. Diabetic blisters are usually painless and heal on their own. Ulcers usually develop on the bottom of the foot. These are common signs of athletes foot.
Why does it appear. Stomach upset including constipation diarrhea. Darker area of skin that feels like velvet.
People suffering from high glucose level tend to get skin infections causing pain tiny blisters with white discharge. Open sores and wounds. Sores ulcers in diabetics usually appear upon your feet.
It can damage any place lower the ankle and continuously grow in size. Theyre often described as looking like blisters that occur when you get a. The ulcer can develop anywhere on your foot or toes.
Diabetic blisters can be as large as 6 inches though theyre normally smaller. What does diabetic dermopathy look like. Outbreak of small reddish-yellow bumps.
Having diabetes can be a serious medical condition especially when the disease is left unmanaged. Light brown oval and circular patches are also a hallmark of necrobiosis lipoidica diabeticorum NLD. Red or skin-colored raised.
If diabetes has been poorly controlled for years it can feel like you have pebbles in your fingertips. Diabetic blisters most often appear on your legs feet and toes. If diabetes affects any of the nerves that control these functions you may experience the following symptoms.
Rarely people with diabetes erupt in blisters. These sores look like burn blisters and often occur in people who have diabetic neuropathy.
Poor Blood Flow Results In Itchy Skin
Itchy skin can have many causes. In people with diabetes, a yeast infection, dry skin, or poor circulation can be the root cause. When poor blood flow is the culprit, the lower legs may be the itchiest part of the body. What can you do to stop your skin from crawling? Consider bathing less often, and use mild soap when you do. Slather on some lotion to moisturize dry skin, but avoid applying it between your toes.
Don’t Miss: Does Metformin Cause Hypoglycemia
How People With Diabetes Develop Sores On Legs
One of the greatest fears for diabetic people is to develop sores on their legs and feet. If you have these sores, it means your blood sugar levels are uncontrollably high and you need immediate medical attention. But what causes these sores? Lets find out!
Sores on legs for diabetics are caused by to two main things:
- 1. Damage to blood vessels:
When you have diabetes, it means your blood glucose levels are higher than they should be. This has a lot of ill effects on your body and one of the effects is cell damage. High blood sugar damages your cells in two ways. First, high blood sugar sucks water out of your cells and damages them. Second, high blood sugar acts as a toxin for your cells and damages them directly.
Almost all cells of the body can suffer some degree of damage due to high blood glucose, and cells of the bodies blood vessels are no exception. The blood vessels are like pipes that transport blood to your body cells. When the cells of your blood vessels are damaged they start to swell up. This distorts their architecture and they fail to deliver blood to your body parts.
Your body cells need to get a constant supply of blood to survive. Thats because blood gives your cells oxygen, glucose and other nutrients
- 2. Due to damage to the bodies nerves:
These two factors commonly add up for diabetics and result in sores on legs and feet.
What Are Foot Ulcers
A foot ulcer is an open sore on the foot.
A foot ulcer can be a shallow red crater that involves only the surface skin. A foot ulcer also can be very deep. A deep foot ulcer may be a crater that extends through the full thickness of the skin. It may involve tendons, bones and other deep structures.
People with diabetes and people with poor circulation are more likely to develop foot ulcers. It can be difficult to heal a foot ulcer. In people with these conditions, even a small foot ulcer can become infected if it does not heal quickly.
If an infection occurs in an ulcer and is not treated right away, it can develop into:
- An abscess
- A spreading infection of the skin and underlying fat
- A bone infection
- Gangrene. Gangrene is an area of dead, darkened body tissue caused by poor blood flow.
Among people with diabetes, most severe foot infections that ultimately require some part of the toe, foot or lower leg to be amputated start as a foot ulcer.
Foot ulcers are especially common in people who have one or more of the following health problems:
- Peripheral neuropathy. This is nerve damage in the feet or lower legs. Diabetes is the most common cause of peripheral neuropathy. When nerves in the feet are damaged, they can no longer warn about pain or discomfort. When this happens, tight-fitting shoes can trigger a foot ulcer by rubbing on a part of the foot that has become numb.
In addition to diabetes, other medical conditions that increase the risk of foot ulcers include:
Read Also: Max Daily Dose Of Metformin

